Twice-yearly treatment injections for multidrug-resistant HIV
Lenacapavir is a new antiretroviral medication, which can be given just twice a year. In this study, presented to the 11th International AIDS Society Conference on HIV Science (IAS 2021) this week, it was given as a subcutaneous (under the skin) injection in the belly.
Professor Jean-Michel Molina of Hôpital Saint-Louis in Paris presented results from the first six months of the study. One group of 24 people received oral lenacapavir for two weeks, followed by an injection of lenacapavir and an optimised background regimen (i.e. the best combination of other drugs given the resistance profile of that person’s HIV). Another 12 participants received placebo pills for two weeks, then oral lenacapavir for two more weeks plus an optimised background regimen, then the injections.
By week 26, 81% had viral loads below 50 and 89% below 400. This was despite the fact that in more than half of these participants, researchers were unable to construct an optimised background regimen that had more than one active drug in it. Further results from the study will be assessed at week 52.
Lenacapavir is also being studied for use with people new to treatment. Early results from this study will be reported to IAS 2021 today.
People with HIV should be prioritised for COVID-19 vaccination

WHO carried out a study of over 15,000 cases of COVID-19 in people living with HIV, mostly in South Africa (94.6%). The study found that:
- People living with HIV were 13% more likely to be admitted to hospital with severe or critical COVID-19, after controlling for age, gender and co-morbidities.
- They were more likely to die after admission to hospital with COVID-19; people living with HIV had a 30% increased risk of death independent of age, gender, severity at presentation, and co-morbidities.
- Among people living with HIV, diabetes, high blood pressure, being male or over 75 years old were each associated with an increased risk of death.
Although the increase in risk of severe COVID-19 is modest, it is especially important in countries like South Africa where the number of people with HIV is large, Dr Silvia Bertagnolio of WHO told aidsmap.
Last week, WHO recommended that people living with HIV should be prioritised for vaccination. But countries also need access to vaccine supplies.
“There’s a critical need for vaccine equity; in lower- and middle-income countries we have only 3-4% vaccine coverage and we need to get the first dose into everyone,” Dr Meg Doherty, director of WHO’s Global HIV, Hepatitis and STI Programmes told a press briefing.
Hepatitis C virtually eliminated in people with HIV in the Netherlands
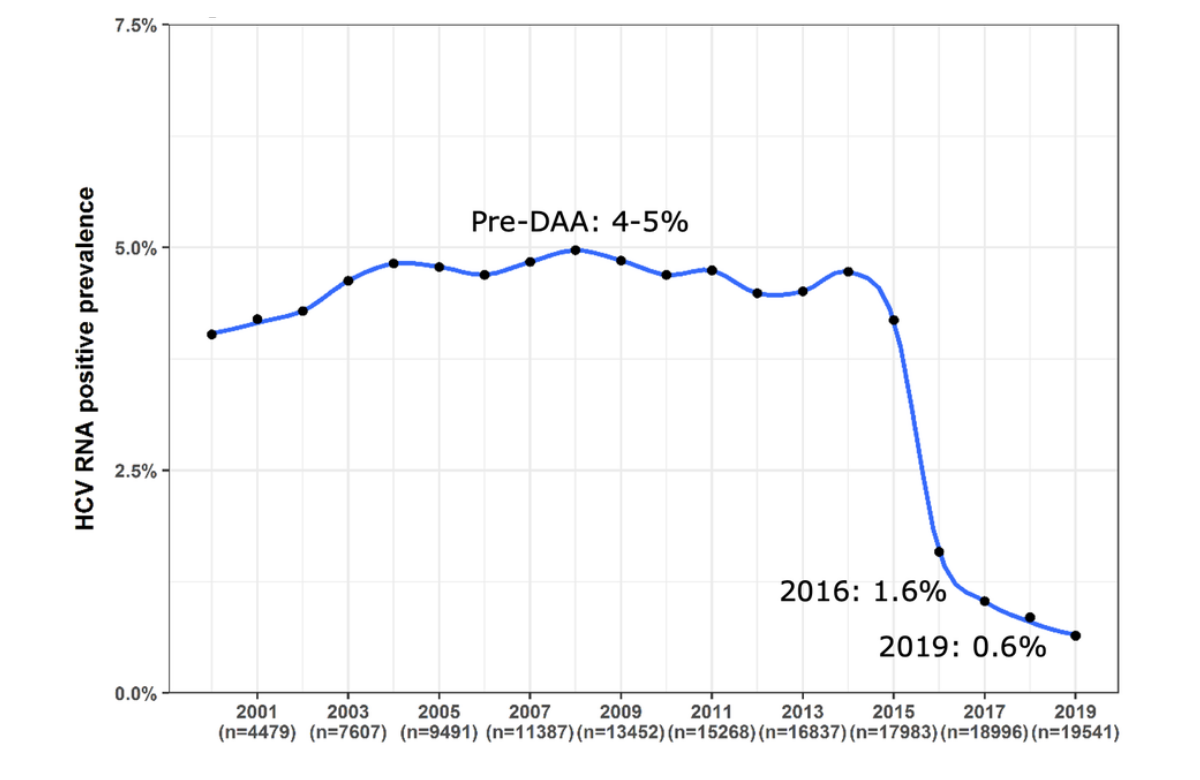
The World Health Organization has set targets for global hepatitis C elimination by 2030, so that 80% of people with chronic hepatitis C infection have been treated and new cases have fallen by 90% compared with 2015. At a national level, elimination of hepatitis C depends on screening, diagnosis and linkage to treatment, as well as availability of treatment. Population groups with a high prevalence of hepatitis C, such as people living with HIV, have been prioritised for micro-elimination campaigns.
Data came from a national cohort which includes 98% of adults and children with HIV who are in medical care. Researchers found that chronic hepatitis C prevalence was stable in the cohort between 2000 and 2014, in the range of 4 to 5%. By 2016, prevalence had fallen to 1.6% after rapid uptake of treatment and fell to 0.6% by 2019.
The prevalence among gay and bisexual men rose from 1% in 2000 to over 4% in 2014, before declining sharply, reaching 0.5% in 2019. In people who inject drugs, prevalence fell from 70% in 2000 to 58% in 2014, and to 12% in 2019.
Only 29 people in the cohort still had chronic hepatitis C infection by the end of 2020.
People who were less engaged with HIV care and people who inject drugs were more likely to remain untreated for hepatitis C.
Presenting the results, Dr Cas Isfordink concluded, “The Netherlands is close to hepatitis C virus micro-elimination in people living with HIV.”
Countries with most HIV still not recommending dolutegravir for all
The integrase inhibitor dolutegravir was first recommended by WHO as part of an alternative first-line regimen in 2016. However, preliminary data on a possible raised risk of neural tube defects (a type of birth defect) from a study in Botswana in 2018 led to safety warnings, and WHO responded by recommending dolutegravir for women of childbearing age only if reliable contraception were available.
Follow-up data from Botswana and elsewhere provided reassurance about the safety of dolutegravir in pregnancy and in 2019, WHO recommended dolutegravir as part of first-line treatment for all adults. However, the concerns appear to have had long-lasting effects.
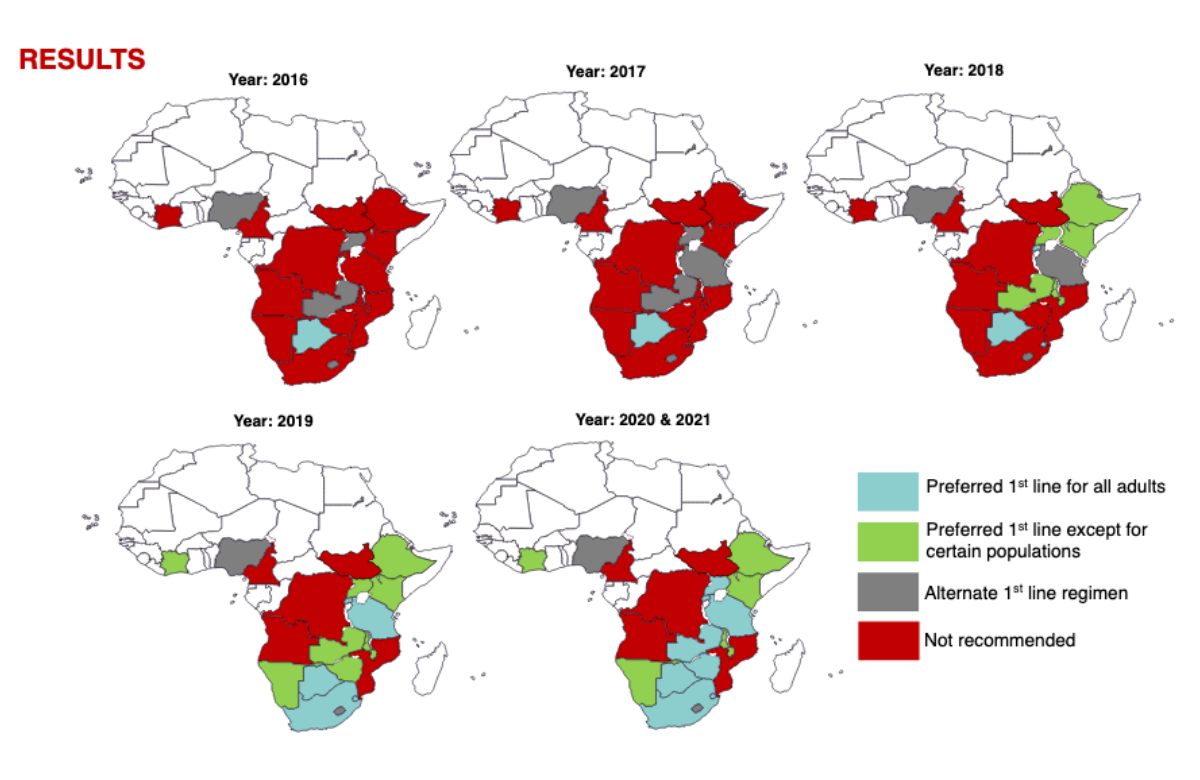
Researchers looked at treatment guidelines published by the 20 sub-Saharan African countries with the greatest burden of HIV. Eight countries recommended dolutegravir for all, in line with current WHO guidelines. However, five countries recommend dolutegravir for everyone except pregnant women (the 2018 guidelines), two countries recommend it only as an alternative regimen (2016 guidelines) and five countries do not recommend it at all.
The 12 countries not currently recommending dolutegravir in line with current WHO guidelines cover around 39% of people living with HIV in sub-Saharan Africa.
The study authors call for speedier processes to translate scientific knowledge into policy and services.
Sexual violence against women in Uganda increased during COVID-19
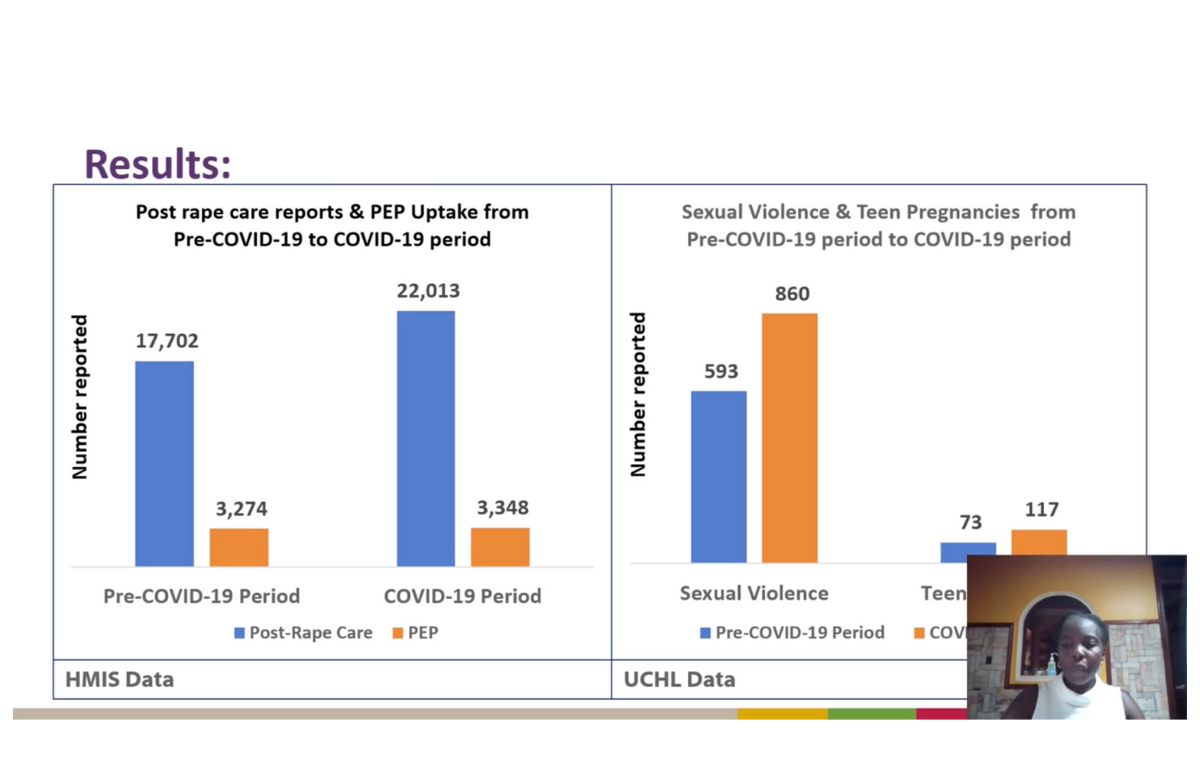
Reports of rape and sexual violence increased among women and girls in Uganda during the COVID-19 pandemic, while uptake of PEP (emergency treatment to prevent HIV infection) decreased. These outcomes, reported to IAS 2021, suggest that women and girls in Uganda may have had increased HIV exposure during the COVID-19 pandemic.
Rose Apondi of the Centers for Disease Control and Prevention and colleagues analysed routine programme data to compare outcomes of six-month periods before (October 2019 to March 2020) and during (April 2020 to September 2020) the COVID-19 pandemic. The team reviewed post-rape reports and PEP uptake for women and girls of all ages from routine health records, as well as reports of sexual violence and teen pregnancy among girls under 18 to the Uganda Child Helpline.
In the six months before COVID-19, 17,702 women reported for post-rape care and 3274 received PEP. In the six-month period studied during COVID-19, 22,013 women sought post-rape care and 3348 received PEP. Over 50% of the post-rape care reported during COVID-19 was done after the recommended 72 hours, with lockdown being cited for the delay in seeking care.
In the six months before COVID-19, 593 girls under the age of 18 reported sexual violence compared to 860 girls in the six months during COVID-19.
Gender-based and sexual violence often go unreported, so the actual increases may have been higher, since this study relied on reports to healthcare workers or a helpline. The authors call for flexible and adaptive gender-based violence services to be prioritised during pandemics, especially during lockdowns.
