According to a US study in the 1 July issue of AIDS, HIV-positive men are at a higher risk of abnormal pulmonary gas exchange than HIV-negative men. These data reinforce the evidence that people living with HIV are more exposed to lung function impairment than HIV-negative individuals.
The study was conducted in 2017-18 within MACS (Multicenter AIDS Cohort Study), an ongoing US cohort study of men who have sex with men, living with or without HIV, which began enrolling in the mid-1980s.
Its main objective was to compare lung function among HIV-positive and HIV-negative participants, with the use of spirometry and single-breath diffusing capacity for carbon monoxide, commonly termed DLCO in medical practice.
Measuring your breathing
Spirometry and DLCO are easy to perform and measure different aspects of lung function.
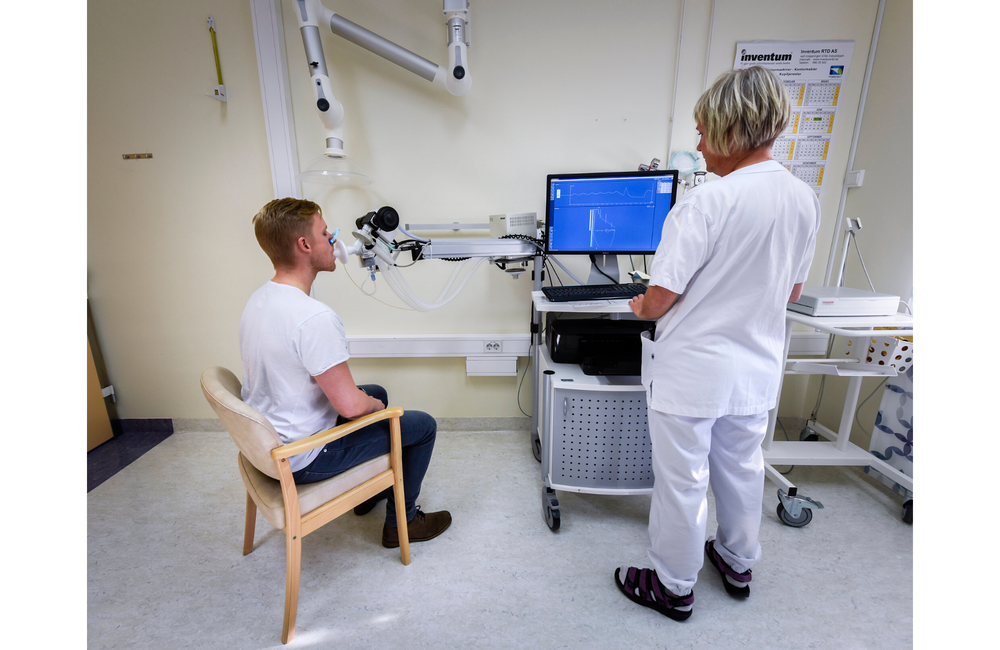
Spirometry measures airflow into and out of your lungs with a spirometer, a device inserted in your mouth. It helps detect pulmonary obstruction, caused by conditions such as chronic obstructive pulmonary disease (commonly termed COPD) or asthma. The most common measurements are:
- The forced expiratory volume1 or FEV1, that is, the maximal amount of air you can forcefully exhale in one second.
- The forced vital capacity or FVC, that is, the total amount of air you can blow out in one complete breath, after taking a deep breath.
- The percentage of air blown out in the first second is calculated by dividing your FEV1 by your FVC and multiplying by 100. In normal, healthy lungs, this will be 70% or above.
DLCO is a calculated value that determines the ability of the lungs to transfer oxygen to blood through the air sacs of your lungs, called alveoli. You are asked to inhale, then exhale, a small quantity of carbon monoxide (CO), used because of its better affinity than oxygen for the red cells circulating in the blood vessels behind the alveoli.
Test results are compared with the individual’s predicted normal value, based on a calculation that includes their gender, height, weight and race. For example, when DLCO is below 75% of the predicted value, it indicates a problem that may impair exercise and affect long-term survival from lung diseases and disorders.
DLCO is less often used than spirometry, although it may be a more sensitive test for identifying lung abnormalities. It is sometimes referred to as a lung diffusion or gas transfer test.
The study
HIV has been identified as a risk factor for emphysema (damaged alveoli), expiratory airflow limitations, gas exchange abnormalities and respiratory symptoms. This brought Dr Ken Kunisaki and colleagues to test the hypothesis that HIV-positive men would have worse measures of lung airflow than their HIV-negative counterparts.
Of note, so far, studies had small numbers of participants, not measured DLCO and not always compared HIV-positive to HIV-negative individuals.
A total of 1176 out of 1305 (90%) of MACS participants were recruited in the study, and 1067 spirometry and 1042 DLCO test results were available for analysis. Participants also reported breathlessness and other “symptoms of quality of life” in two different questionnaires.
As ageing can affect lung function, it should be noted that in the MACS cohort, most participants were aged between 49 and 65 years (median age 57). Likewise, many participants smoked or had smoked:
HIV-positive participants:
- Marijuana use: 35%.
- Current tobacco smoking: 26%.
- Former tobacco smoking: 42%.
HIV-negative participants:
- Marijuana use: 25%.
- Current tobacco smoking: 20%.
- Former tobacco smoking: 49%.
At the time of pulmonary testing, 90% of HIV-positive participants were taking antiretroviral therapy and 88.8% had an undetectable viral load. Current CD4 cell counts were high, with an average of 674 cells/mm3, while the CD4 cell nadir ranged from 235 to 525/mm3. Also, among HIV-positive participants, the prevalence of a history of AIDS (7.6%), Pneumocystis pneumonia (2.9%), hepatitis B (3.1%) and hepatitis C (7.3%) was low.
The researchers highlight that “compared with HIV-negative study participants, the HIV-positive participants were younger, more commonly of African ancestry, more likely to report current smoking and illicit drug use, more commonly infected with hepatitis B or C, and less commonly enrolled in the initial 1984-1985 wave of enrolment.” Some of the researchers’ analyses were adjusted for these potential confounders.
Results
In the overall cohort, median FEV1 and DLCO were 97% and 85% of predicted normal values, respectively. In the unadjusted analysis, FEV1 was similar in both populations, but after adjustment for potential confounders, it appeared worse in HIV-positive individuals (2.2% worse score).
HIV-positive participants also showed lower DLCO predicted values (2.6% worse score). Furthermore, 39% of HIV-positive participants had a DLCO below 80% of their predicted value, compared to 33% of HIV-negative participants. Concerning the more severe impairment of DLCO below 60% of the predicted value, this was seen in 5.8% of HIV-positive and 3.2% of HIV-negative participants. Those with HIV had triple the risk for this outcome (adjusted odds ratio 2.97; 95% confidence interval 1.36 to 6.47).
The study investigators say that their main finding is that HIV status is more closely associated with impairments in measures of gas exchange (DLCO) than measures of airflow obstruction (FEV1 or spirometry).
FEV1 and airflow obstruction tended to be worse among HIV-positive participants than among their HIV-negative counterparts, although the differences were not statistically significant. This is a surprising finding, as the literature has so far reported that odds for COPD – whose diagnosis is partly based on FEV1 – among HIV-positive individuals are significantly higher.
Still, in line with previous scientific papers, COPD prevalence was 9.7% among HIV-positive participants, which is not a low rate. The researchers comment: “Given the impact of COPD on mortality, quality of life and work productivity, the presence of COPD in nearly 10% of HIV-positive persons should prompt further research into HIV-specific case-finding, treatment and prevention strategies”.
Other findings and associations
Some of the study’s other findings deserve our attention.
Concerning patient reported outcomes, no statistically significant differences between the two groups were found. However, HIV-positive participants reported worse symptom scores, even if it is unclear what they mean clinically.
The data suggested that more years of antiretroviral therapy exposure might be associated with worse DLCO values and higher odds of DLCO impairment, but showed no association with FEV1. Cautiously, the investigators evoke a potential harmful role of antiretrovirals on lungs or an impact of the immune reconstitution on gas exchange.
"HIV status is more closely associated with impairments in measures of gas exchange (DLCO) than measures of airflow obstruction (FEV1 or spirometry)."
A higher nadir CD4 cell count was associated with a higher DLCO predicted value and a lower risk of DLCO impairment, confirming a relationship between CD4 cell count nadir and DLCO that has been reported before. Mechanisms for this relationship are currently unclear, but may result from alterations in the microbiome (‘good’ and ‘bad’ bacteria and other microbes) in the airway or co-infections with other chronic viruses like cytomegalovirus or herpes viruses.
One result is flagged as “unexpected” by the paper’s authors and has seemingly never been reported before. Among HIV-positive participants, a higher CD4 cell count was associated with a lower FEV1 and with higher odds of FEV1 impairment, but with lower odds of DLCO impairment (the higher the CD4 count, the better the DLCO).
Trying to answer the obvious question brought here, the paper states that, although unclear, the reasons for the discrepancy between current CD4 counts and measures such as FEV1, versus gas exchange, could reflect complex relationships between immune function and different types of COPD, for which either of the two tests will be more sensitive.
Nearly as unclear is the reason why, “compared with HIV-seronegative men, HIV-positive men are at increased risk of abnormal pulmonary gas exchange, as measured by DLCO.” Several hypotheses to explain this phenomenon emerge, that would warrant future thorough explorations.
Kunisaki KM et al. Lung function in men with and without HIV. AIDS 34: 1227-1235, 2020.
doi: 10.1097/QAD.0000000000002526
Full image credit: 'Spirometri - lungesykdommer' by Helgelandssykehuset. Available at www.flickr.com/photos/135766077@N03/38034462881 under a Creative Commons licence CC BY-NC-ND 2.0.
