People with low CD4 counts have weaker response to COVID-19 vaccines
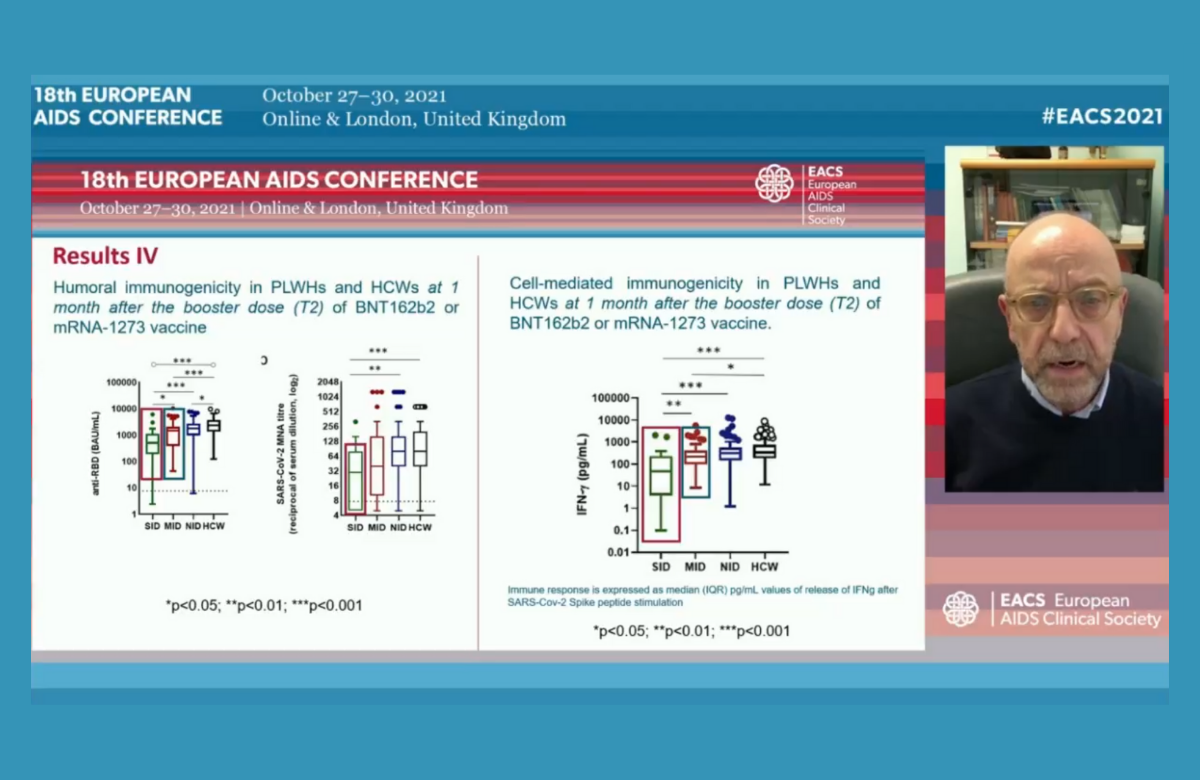
People with CD4 counts below 200 were significantly less likely to generate strong antibody and cellular immune responses to the Pfizer or Moderna mRNA COVID-19 vaccines compared to people with better immune function, Dr Andrea Antinori of the Italian National Institute for Infectious Diseases reported on Friday at the 18th European AIDS Conference (EACS 2021) in London.
The majority of previous studies on COVID-19 vaccine response in people with HIV have been conducted with individuals who have mostly had robust CD4 cell counts.
The researchers compared antibody and cellular immune responses after vaccination in 32 people with HIV with severe immune deficiency (current CD4 count below 200), 56 people with HIV with moderate immune deficiency (CD4 count between 200 and 500) and 78 people without immune deficiency (CD4 count above 500). All participants were taking antiretroviral therapy but 31% of people with CD4 counts below 200 had an unsuppressed viral load.
The study assessed antibody responses by measuring receptor binding domain IgG antibody levels and neutralising antibody levels at three time points. On all measures, people with CD4 counts below 200 had antibody or neutralisation measurements approximately one-third of those observed in people with CD4 counts above 500. Cellular immune responses, measured by interferon-gamma release assay, also showed statistically significant differences, after adjusting for confounding factors including age, nadir CD4 count, type of vaccine received, detectable viral load and current or prior malignancy.
Lower antibody numbers after the second vaccine dose imply a greater need for a third dose in people with a CD4 count below 200. Further research is needed to clarify the impact of a third dose in this group, on both the level of antibody response achieved and the speed at which antibody levels decline after a third dose.
Varying levels of COVID-19 vaccination in people with HIV in central and eastern Europe
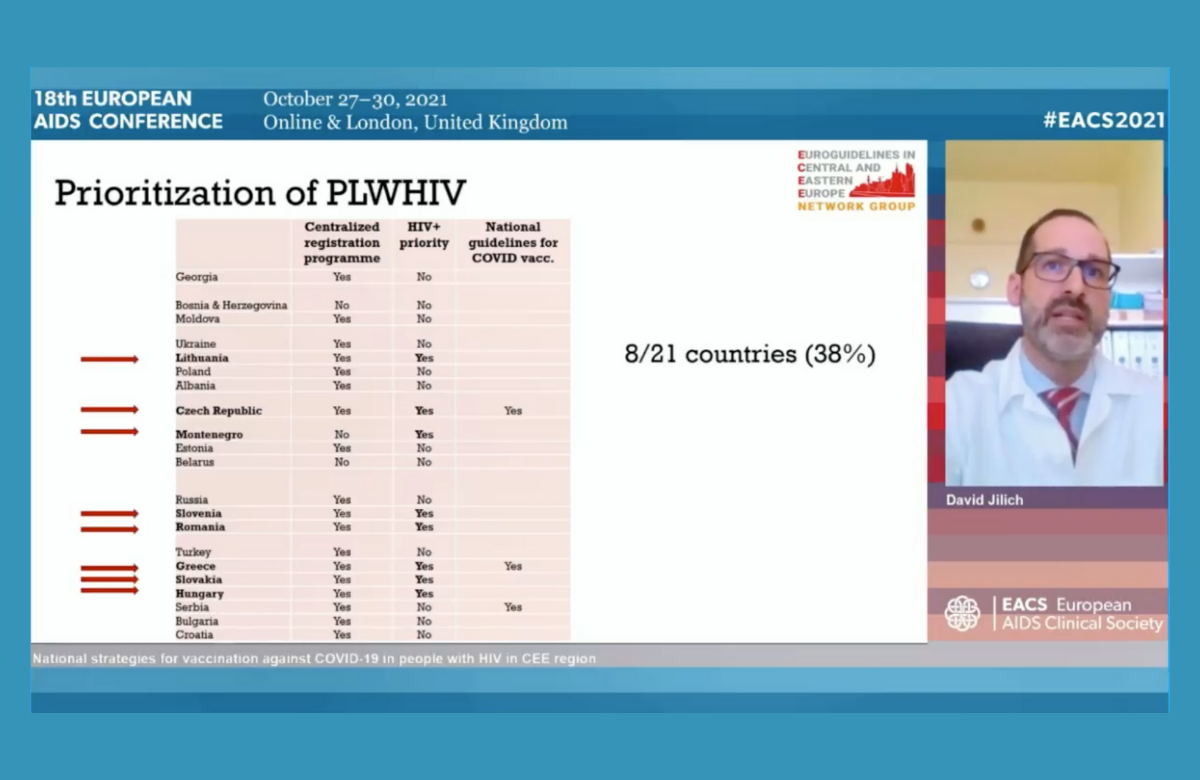
People with HIV are not being prioritised for COVID-19 vaccination in all countries in central and eastern Europe and vaccination rates in this vulnerable population remain low in some countries, Dr David Jilich of Charles University, Prague, told the conference.
Information came from 22 countries in central Europe, eastern Europe, the Baltic, the Caucasus, the Balkans and Turkey.
People with HIV had been prioritised for vaccination in only eight of the 22 countries and only three of the 22 countries had formulated guidelines for the vaccination of people with HIV. Only 12 countries had started vaccinating by mid-March 2021, reflecting difficulties in obtaining vaccine supplies and completing registration procedures.
By September 2021, whereas 85-90% of people with HIV have been vaccinated in Greece and the Czech Republic, coverage was 50% or less in Estonia, Hungary and Bulgaria, partly reflecting much lower levels of general population vaccination in some of these countries.
The findings highlight the need for further research on COVID-19 and vaccination in people with HIV across a wide range of settings in order to explore the implications of these variations and apparent inequalities in access.
Half of Swiss mothers with HIV choose to breastfeed
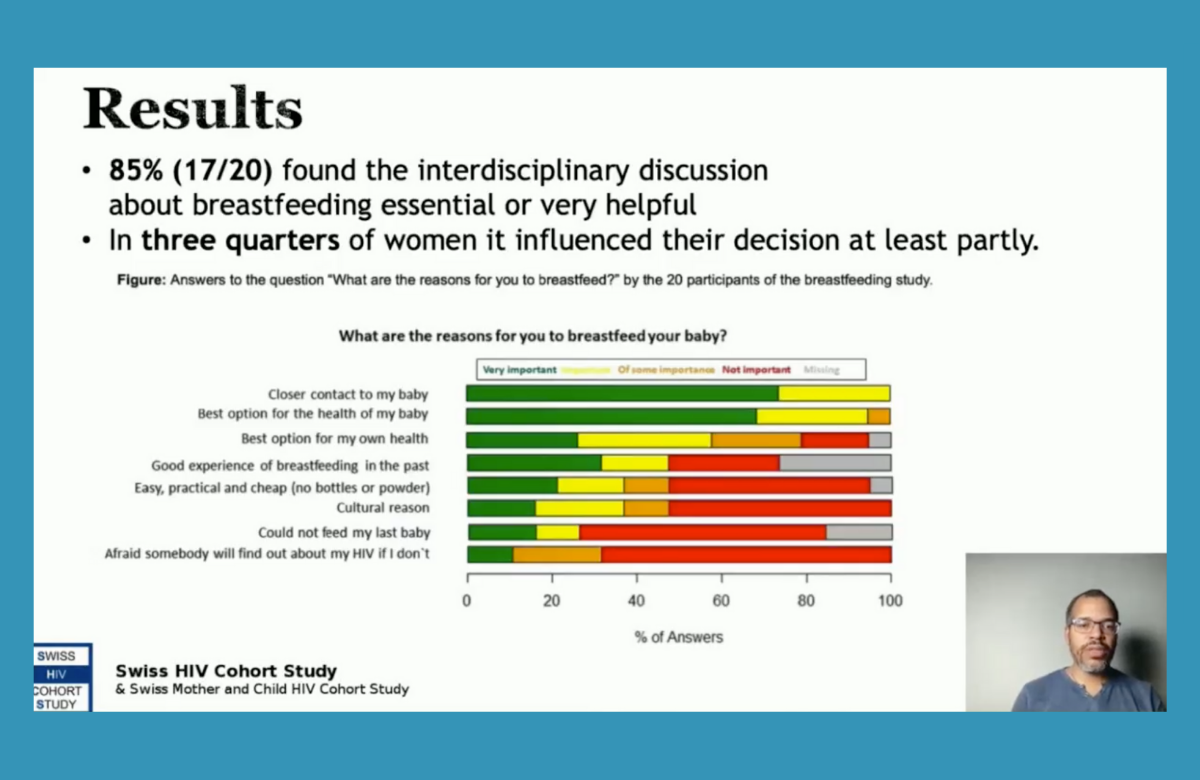
Swiss HIV guidelines were revised in 2019 to offer mothers living with HIV a discussion of the respective risks and benefits of breastfeeding and formula feeding, allowing them to make a choice on their preferred way to feed their baby, provided they have an undetectable viral load.
Expectant mothers attend a multidisciplinary meeting with a midwife, an obstetrician, and adult and paediatric HIV doctors where the possibility of transmission and how to avoid it is explained. Mothers who opt for breastfeeding receive intensified viral load monitoring and their infants are tested for HIV more regularly.
At EACS 2021, Dr Pierre-Alex Crisinel of Lausanne University Hospital reported on the first 41 mothers to have given birth since the policy change. Almost half (20) decided to breastfeed despite the additional monitoring requirements. Women who had been diagnosed with HIV for longer were more likely to choose to breastfeed.
Asked why they decided to do so, closer contact and bonding with their baby was an ‘important’ or ‘very important’ reason for all women, and all but one woman said that breastfeeding being the best option for their baby’s health was an important factor. Only six women said cultural expectations about breastfeeding were important and only two said that fear of HIV disclosure was important.
The feeling of being involved in shared decision-making with their healthcare staff was greatly valued, Dr Crisinel said.
Lung function declines faster in people living with HIV

Dr Rebekka Thudium from the University of Copenhagen told the conference that people living with HIV who are taking effective antiretroviral therapy have a faster rate of lung function decline than HIV-negative people.
Chronic lung disease is common among people with HIV. Both risk factors also found in the general population and HIV-related risk factors may contribute to the condition. Only a few studies have measured lung function over time in people with HIV.
A total of 1130 members of two HIV-positive cohorts in Denmark and the United States were compared with HIV-negative controls from the Danish general population, matched on age and sex.
The study’s primary outcome was the annual rate of decline in Forced Expiratory Volume1 (FEV1), which is the maximal amount of air a person can forcefully exhale in one second. On average, participants living with HIV had an additional decline of 8.5ml a year.
Compared to HIV-negative people of the same smoking status, faster declines were seen in HIV-positive current smokers, former smokers and people who had never smoked. However, the largest difference was in current smokers living with HIV: an extra 16.8ml a year decline of lung function, when compared with HIV-negative smokers.
This suggests that the association between HIV and lung function decline is amplified by smoking, which appears to be more harmful in people with HIV than those without. However, lung function also declines faster in people living with HIV who never smoked, suggesting that mechanisms independent of smoking also play a role.
High participation of trans people in English PrEP trial
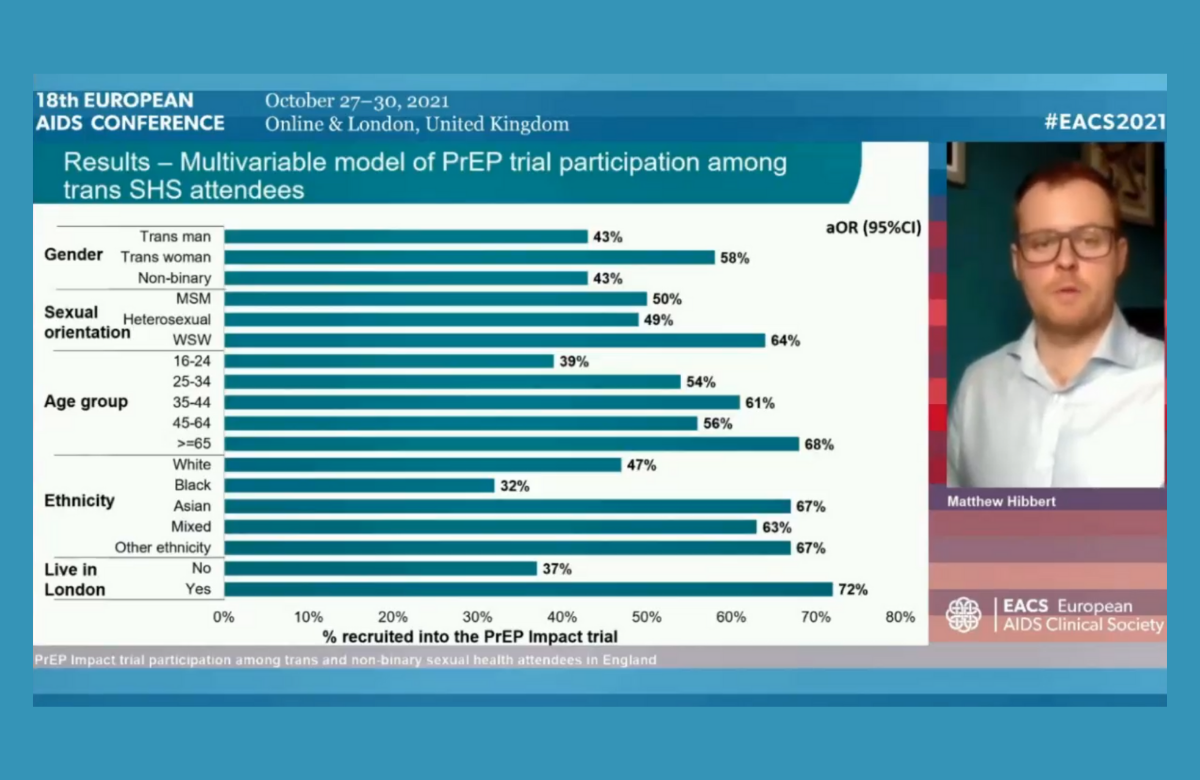
Just over half the trans and non-binary people who attended sexual health services in England during the period of the IMPACT trial ended up participating in it, Dr Matthew Hibbert of the UK Health Security Agency told the conference.
IMPACT was the large English PrEP implementation study run between October 2017 and July 2020, before PrEP became routinely available. The vast majority of its 24,255 participants were cisgender gay and bisexual men, with smaller numbers of cisgender heterosexual men and women taking part. Concerted efforts were made by trans community advocates and the specialist sexual health service CliniQ in London to engage trans and non-binary people.
As a result, 501 trans and non-binary people took part (of 978 attendees recorded by sexual health clinics as having a different gender to the one assigned to them at birth). Of the attendees who did not join the study, the majority were not thought to have a sufficiently high risk of HIV for a PrEP referral. However, 75 individuals who were eligible for PrEP were not offered it.
The strongest predictor of whether people took PrEP was having had an STI (84% of those with a recent bacterial STI diagnosis in the previous three months joined the study). However, trans people under the age of 25 or of Black ethnicity were less likely to join the study.
People living in London more than twice as likely to receive PrEP, showing the value of specialist services where trans people feel safe and their needs understood.
Nonetheless, the total size of the adult trans and non-binary population in England is estimated to be around 70,000 people, suggesting that many trans and non-binary people are not being reached by sexual health services.
