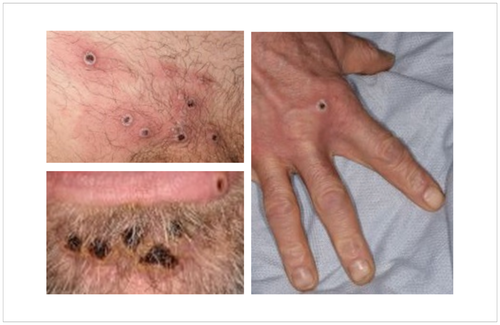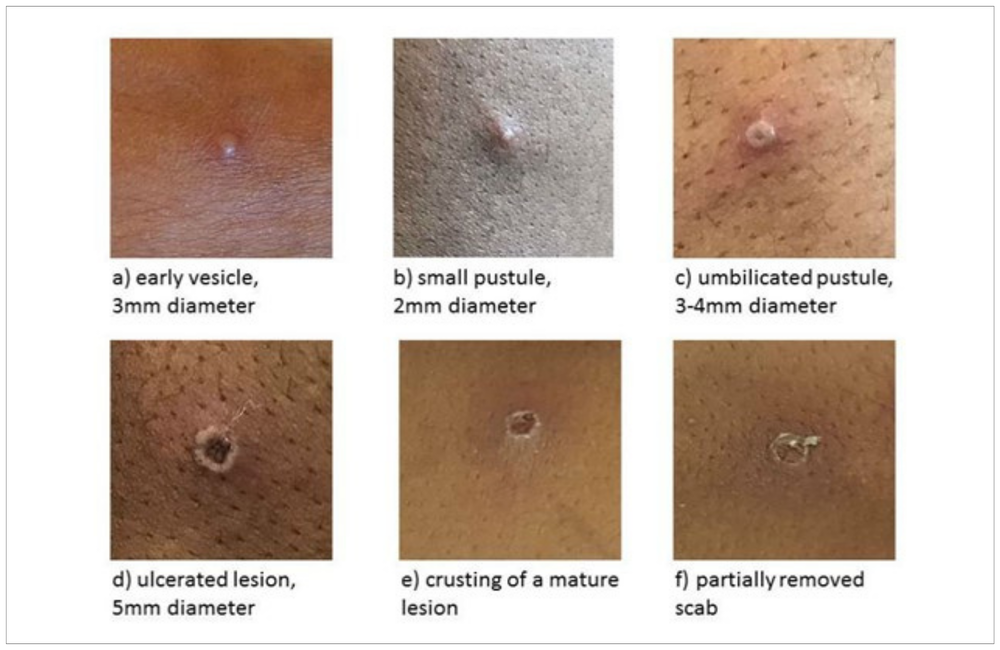
The World Health Organization (WHO) has now confirmed nearly 100 cases of monkeypox in over a dozen countries, with the largest number in the UK. While most cases so far are among gay and bisexual men, health officials emphasise that anyone can contract the virus through close personal contact.
The UK Health Security Agency (UKHSA) reported the first case in the current outbreak on 7 May in a man who had recently travelled to Nigeria, where monkeypox is endemic. This was soon followed by two additional cases who share a household and four cases among gay and bisexual men, all of whom appear to have contracted the virus locally. As of 23 May, UKHSA has reported 70 confirmed cases in England and one in Scotland.
The latest WHO update on 21 May listed 92 confirmed and 28 suspected cases. After the UK, the most cases have been reported in Spain and Portugal, with smaller numbers in several other European countries, Canada, the United States and Australia. An informal tally by Global.health, compiled from various sources, listed more than 300 confirmed or suspected cases worldwide as of 25 May.
Cases so far have “mainly but not exclusively been identified amongst men who have sex with men,” according to WHO. Among the Global.health cases with a known sex and age, all but three are young or middle-aged men. Many of the affected men identify as gay or bisexual or sought care at sexual health clinics. Several cases are reportedly linked to a sauna in Spain and a fetish festival in Belgium. Many of the men reported recent international travel.
Monkeypox background
Monkeypox, which is related to smallpox, is not a new disease. Despite its name, it is most commonly associated with rodents. Although primarily seen in Central and West Africa, isolated cases are occasionally reported in Europe and elsewhere, often involving travellers. The current outbreak is the largest ever seen outside of Africa.
Smallpox vaccination prevents monkeypox as well, and monkeypox cases have been rising over the past few decades since routine smallpox vaccination was discontinued; WHO declared that smallpox had been eradicated worldwide in 1980. This means only older people have vaccine-induced immunity.
Less severe than smallpox, monkeypox typically causes flu-like symptoms (e.g., fever, fatigue, muscle aches), swollen lymph nodes and a rash. The rash can appear on the face, genitals, palms, soles of the feet and elsewhere on the body. The sores can be flat, raised or pus-filled, and may resemble other conditions such as herpes, syphilis or chickenpox. In the current outbreak, several cases initially presented with a genital rash, and some did not report other symptoms. The virus has an incubation period of up to three weeks, and the illness typically lasts two to four weeks.
The monkeypox virus is transmitted through close personal contact, including skin-to-skin contact and kissing. Close contact may involve household members and health care workers. The virus can also spread via clothes or linens that have been in contact with fluid from sores. Health officials say monkeypox can be transmitted via respiratory droplets at close range, but the virus does not appear to spread through the air over longer distances in the same way as the SARS-CoV-2 coronavirus that causes COVID-19.
Monkeypox is generally not considered a sexually transmitted infection, and it is not known whether it can be transmitted through semen during intercourse. “Monkeypox is not a sexually transmitted infection in the typical sense, but it can be transmitted during sexual and intimate contact,” Dr John Brooks, an epidemiologist with the US Centers for Disease Control and Prevention, said during a 23 May media briefing.
Experts historically thought monkeypox was not easily transmitted between humans, and it is unclear why it is now spreading more extensively. Some have suggested the virus may have evolved to become more easily transmissible, but so far genetic sequencing does not support this hypothesis. More likely, the virus entered a social or sexual network by chance and found favourable conditions for transmission.
Public health advice
Health officials are urging anyone with an unusual rash or lesions on any part of their body, especially the genitals, to contact their health care provider or a sexual health clinic. People who suspect they may have monkeypox are advised to refrain from close social contact until they get tested. High-risk contacts of known cases should isolate and self-monitor for symptoms for up to 21 days. People with confirmed monkeypox should isolate, abstain from sexual activity and avoid close physical contact until the rash heals completely, according to the European Centre for Disease Prevention and Control (ECDC).
“If anyone suspects they might have rashes or lesions on any part of their body, particularly if they have recently had a new sexual partner, they should limit their contact with others and contact NHS 111 or their local sexual health service as soon as possible—though please phone ahead before attending in person,” said UKHSA chief medical adviser Dr Susan Hopkins.
People with monkeypox usually recover without treatment. The strain circulating in Europe has a fatality rate of around 1%; there have been no deaths reported in the current outbreak. Monkeypox is more likely to cause severe illness in children, pregnant women and immunocompromised people.
However, people with HIV who are on antiretroviral treatment with viral suppression and a CD4 count above 200 “are not at any particular risk of becoming significantly more unwell,” Dr Claire Dewsnap, president of the British Association for Sexual Health and HIV, said during a 23 May aidsmapCHAT.
“There is little data currently to gauge the impact of HIV on morbidity and mortality associated with monkeypox,” according to the European AIDS Clinical Society. “It is likely that persons with advanced and uncontrolled HIV may be at a higher risk of severe disease and prolonged viral shedding.”
Monkeypox can be controlled through ring vaccination, in other words targeted smallpox vaccination for close contacts of an infected individual. The outbreak has spurred calls for resuming universal smallpox vaccination, but experts say this is not necessary to control monkeypox in the general population at this time.
The older live smallpox vaccine (made from a virus called vaccinia) can cause adverse events, especially in immunocompromised people, but there is a newer, safer non-replicating smallpox and monkeypox vaccine (brand names Imvanex or Jynneos). It was approved by European and US regulators in 2013 and 2019 respectively, and is recommended for use in the current outbreak by UK authorities. The UK and other countries maintain a stockpile of smallpox vaccine in case of bioterrorism and are increasing their supplies.
Smallpox vaccines are now being given to high-risk contacts of known cases and health care providers. Because the monkeypox incubation period is so long, vaccination up to two weeks after exposure can reduce the risk of symptomatic infection or severe illness. The new vaccine has been tested and shown to be safe for people with HIV. For people on antiretrovirals with a high CD4 count, Dewsnap advised, “If you’re offered a smallpox vaccine, you should take it.”
Antiviral medications used to treat smallpox can also be used for monkeypox, including tecovirimat (TPOXX), which prevents viral egress from cells, and the nucleoside analogues cidofovir (Vistide; familiar as a treatment for cytomegalovirus retinitis) and brincidofovir (Tembexa).
Health officials and researchers are still learning about the ongoing outbreak, but monkeypox does not spread as easily as COVID-19, and most do not expect a new pandemic of that scale. Experts expect monkeypox cases to increase as new people within social and sexual networks are exposed and previously-exposed individuals move through the incubation period. But they hope contact tracing, isolation and vaccination can bring the outbreak under control.
Based on an ECDC epidemiological assessment, “the likelihood of monkeypox spreading in persons having multiple sexual partners in the European Union/European Economic Area is considered high.” But given that the disease has so far been mild, the overall risk is considered moderate for this group and low for the broader population.
Meanwhile, many in the LGBT community are concerned that a disease primarily striking gay and bisexual men could lead to the same kind of blame and stigma seen with HIV and AIDS. Acknowledging who is most affected is important for targeting education and resources, but stigma could discourage ill or exposed people from seeking care, and calling it a “gay disease” could lead others to assume they’re not at risk.
“It’s a virus – it doesn’t choose, it doesn’t judge, it doesn’t have any morality to it,” aidsmap executive director Matthew Hodson said. “Fight the disease, don’t fight people who might be a greater risk for acquiring the infection.”