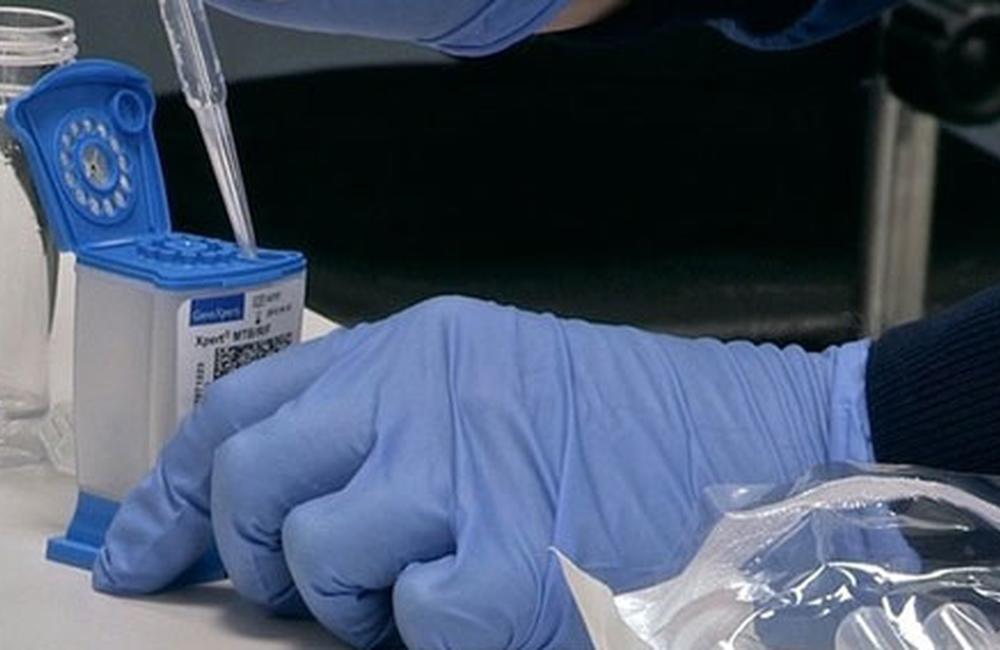
Decentralisation of drug-resistant tuberculosis (DR-TB) management and use of the Xpert MTB/RIF test improves the time from clinic presentation to treatment from 50 days to 7 days in a population with a high burden of HIV and TB co-infection, according to a study from Khayelitsha, South Africa, presented at the 20th International AIDS Conference (AIDS 2014) on Monday.
Xpert MTB/RIF is a rapid test for identification of TB and rifampicin-resistance. The test is being rolled out as a new diagnostic for TB management in countries with a high burden of TB and HIV co-infection, but there is limited evidence on the impact of the test in improving access to care.
Reducing the time between identification of symptoms that suggest TB and the start of treatment is critically important. A long delay between seeking health care and starting treatment increases the risk of death from TB. People with TB may be lost from care and in the meantime pass on TB to their close contacts.
The South African study found that the decentralisation of treatment for drug-resistant TB reduced the time from diagnosis to treatment initiation from nine weeks to less than four weeks. Xpert MTB/RIF further reduced the time to treatment initiation to a median of seven days, with more than 90% of people living with HIV who had rifampicin-resistant TB starting treatment.
More than 14,000 people are diagnosed with drug-resistant TB in South Africa every year, with 65% estimated to be living with HIV (often referred to as HIV and TB co-infection). While case detection of drug-resistant TB is high, only 50% of people identified start second-line TB treatment, with delays often up to several months. This leads to high mortality, particularly for people living with HIV, and ongoing transmission.
Khayelitsha is a large township 40km outside Cape Town with a population of approximately 400,000 people. The antenatal HIV prevalence is 37% and there are currently 26,000 people on antiretroviral therapy (ART). Approximately 5100 TB cases are registered each year, with approximately 200 rifampicin-resistant cases per year, 75% of both are in people living with HIV.
Between 2007 and 2013, decentralised management of drug-resistant TB was implemented progressively. Simultaneously, over 2007-2008, first-line drug susceptibility testing (DST) moved from culture-based DST to line probe assay (LPA).
The decentralised programme diagnosed 1368 people with drug-resistant TB (rifampicin-resistance), of whom 51% were female and 72% were living with HIV. Prior to decentralisation (2003-2006), the median time to treatment was 71 days, using culture DST (IQR 22-120 days), declining to 50 (IQR 12-88) with LPA and some decentralisation during 2007-08 (p< 0.0001). Further decentralisation in 2009, 2010 and 2011 reduced the median delay to 39 days (IQR: 11-67), 32 (IQR 12-52), and 27 (IQR: 12-42) days respectively using LPA (p< 0.0001 for trend).
Xpert MTB/RIF was introduced in late 2011. This resulted in median delays of 13 (IQR: 7-19) and 7 (IQR: 3-11) days for 2012 and 2013 (p< 0.0001 when compared to the use of LPA). While HIV infection was associated with longer delays across 2009 to 2011 using LPA (p = 0.02), this significant difference disappeared in 2012-13 once Xpert MTB/RIF was being used. Across 2009 to 2011, 94% of HIV-negative patients initiated treatment, compared to 86% among people living with HIV (p = 0.001). Corresponding figures for 2012-13 using Xpert MTB/RIF were 100% and 89% respectively (p = 0.001).
High specificity for Xpert MTB/RIF in low TB prevalence settings
Another study presented at the conference found that the Xpert MTB/RIF test can identify TB with high specificity in low TB prevalence settings and may facilitate timely evaluation and treatment in HIV-positive and HIV-negative patients.
The study compare the performance of Xpert MTB/RIF in settings with low versus high TB prevalence, in people living with HIV versus HIV-negative people, using induced versus expectorated sputum, and using unprocessed versus sedimented (digested, decontaminated and concentrated) sputum.
In the low TB prevalence setting, a single Xpert MTB/RIF identified all acid-fast bacillus (AFB)-positive and culture-confirmed TB (AFB+/TB culture+) and 58.8% of AFB-negative and culture-confirmed TB (AFB-/TB culture+), with 99.3% specificity. The specificity of a test is the percentage of results that will be correctly negative when a disease is not present. Lower rates of specificity will produce more false-positive results.
The performance of the Xpert MTB/RIF was not significantly impacted by region, HIV status or sputum collection method in the study.
A total of 994 people with suspected pulmonary TB took part in the study. Participants from the low prevalence setting of the United States (71%, n = 776) and the two high prevalence sites of Brazil (10%, n = 99) and South Africa (19%, n = 119) had one unprocessed or sedimented sputum tested by Xpert MTB/RIF) (G4 cartridges) and compared to two sputa, each evaluated with AFB smear and mycobacterial culture on liquid and solid media. All participants had an HIV test. Fisher's exact test compared sensitivity and specificity. Susceptibility to rifampicin was done by the agar proportions method.
Required test results were available for 720 of 994 participants. The sensitivity of Xpert MTB/RIF was 100% (95% CI: 94.6-100) among AFB+/TB culture+ regardless of HIV status, region, sputum processing, or induced/expectorated collection. The sensitivity of a test is the percentage of results that will be correctly positive when a disease is actually present. Lower rates of sensitivity will produce more false-negative results.
Among AFB-/TB culture+, sensitivity was 61.5% (95% CI: 45.9-75.1). Sensitivity among AFB-/TB+ was significantly higher for sedimented (69.7%, n = 23 of 33) compared to unprocessed sputum (16.7%, n = 1 of 6) (p = 0.02). There was no significant difference in sensitivity when induced (63.6%) or expectorated sputum (56%) (p = 0.73) was used. There was also no significant difference in sensitivity for HIV-positive (57.9%) and HIV-negative participants (65%) (p = 0.75), or in the sensitivity for low-prevalence regions (58.8%) and high-prevalence regions (63.6%) (p = 0.99).
Overall specificity was 98.9% (100% AFB+/TB culture+, 98.8% AFB-/TB culture+) and did not differ significantly by HIV status, sputum type, or TB prevalence.
These data support the use of Xpert MTB/RIF in low-prevalence settings and for people living with HIV and may have important implications for the roll-out of this diagnostic.
Luetkemeyer A et al. Performance of Xpert MTB/RIF testing for M.tuberculosis (TB) detection in HIV+ and HIV- pulmonary TB suspects in low versus high TB prevalence settings: the ACTG 5295/TBTC 34 study. 20th International AIDS Conference, abstract MOAB0205, Melbourne, 2014.
View this abstract on the conference website.
View this presentation on the conference website.
Cox H et al. Reduced treatment delays for drug-resistant TB/HIV co-infected patients with decentralized care and rapid Xpert MTB/RIF test in Khayelitsha, South Africa. 20th International AIDS Conference, abstract MOAB0203, Melbourne, 2014.
