Worse COVID-19 outcomes for people with HIV in New York
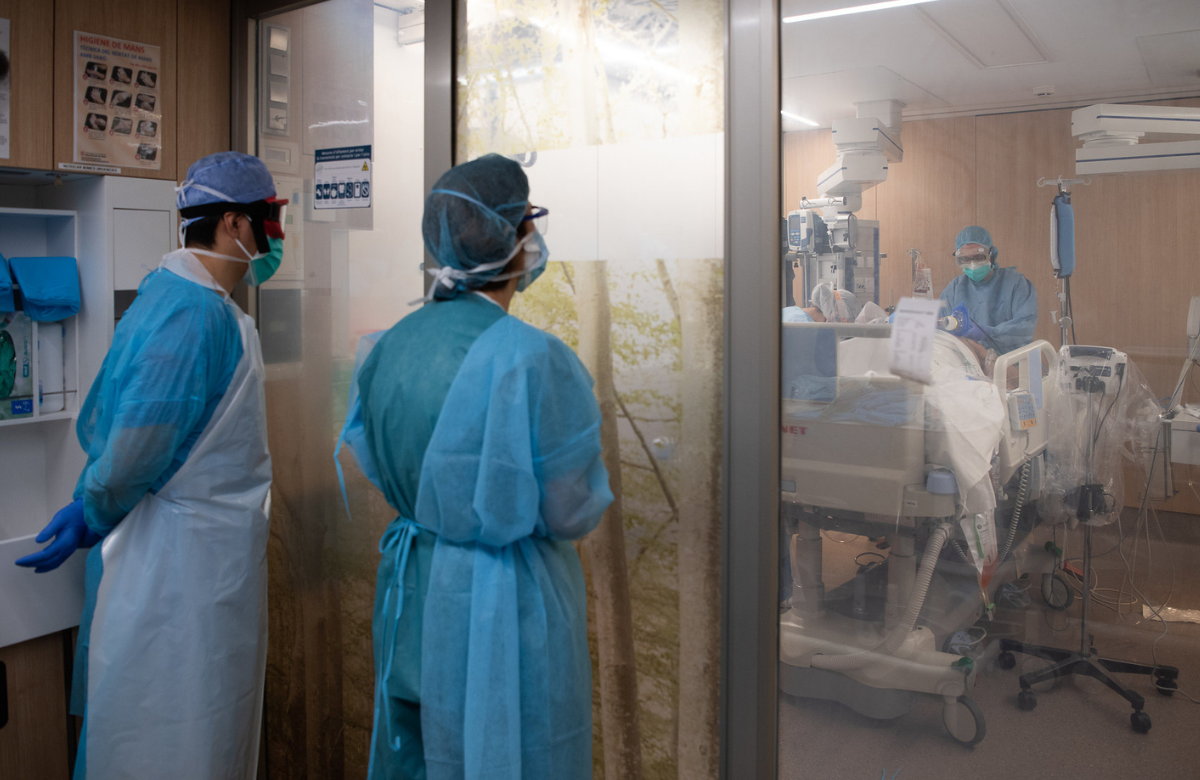
Since the beginning of the COVID-19 pandemic, studies in various countries have had different findings about COVID-19 risks in people with HIV. They generally don’t suggest that people with HIV are more likely to acquire COVID-19, but some have found that people with HIV are at greater risk of worse outcomes if they get ill with COVID-19. This increased risk is relatively small in comparison with the risks associated with older age or some other health conditions.
The latest study to report on this issue comes from New York state, covering almost 380,000 people who were diagnosed with COVID-19 between March and early June. Fewer than 1% also had HIV – people with HIV were not more likely to have COVID than HIV-negative people.
However, among those who had COVID, people with HIV were 38% more likely to be admitted to hospital. They were also 23% more likely to die than HIV-negative people with COVID. As in the general population, these severe outcomes were more common in older people with HIV.
This study also showed that people with advanced HIV disease were at greater risk of needing hospital treatment. Compared to those in better health, those with a CD4 count between 200 and 500 had a 27% greater risk and those with a CD4 count below 200 had a 54% greater risk. People with a viral load over 200 had a 70% greater risk of being admitted to hospital.
These are the kinds of data that are likely to have encouraged policymakers to include people with HIV in one of the priority groups for COVID-19 vaccination in the UK. Everyone who has HIV is in ‘group 6’ along with people with other long-term health conditions, meaning that they will be eligible for vaccination once people over the age of 65 have been vaccinated.
World AIDS Day film: U=U

NAM aidsmap has teamed up with award-winning animation studio Animade to produce U=U for World AIDS Day 2020. The film fights stigma with knowledge by reinforcing the ‘Undetectable = Untransmittable’ consensus statement that people with HIV on effective treatment can’t pass on the virus.
Women with HIV want clearer information on infant feeding

Many of the participants in a recent study had migrated from countries in sub-Saharan Africa or the Caribbean, where the care of newborn babies is different. In those countries, the World Health Organization recommends breastfeeding for women living with HIV because of the lack of clean water and formula milk, which could lead to malnourishment and infection. In wealthy countries, formula feeding is a feasible option and does not carry the potential risk of HIV infection from mother to baby so is recommended instead.
The different advice in different countries needs to be explained, the mothers told researchers. Several had already had children in their home country, as one woman explained:
"You come here, you breastfed two kids back home, and here you are not going to breastfeed. We need to understand. We need to talk about it to accept it."
Some women felt that their ability to make informed decisions had been taken from them by having their baby in Canada. It was felt that healthcare providers were not making a recommendation but instead telling women what to do.
In particular, women wanted information about the risks of passing HIV on through breastfeeding when their viral load is undetectable.
aidsmapCHAT
Last week we broadcast the final episode of this year's aidsmapCHAT.
Joining NAM's Susan Cole were Dr Tristan Barber from the Royal Free Hospital, doctor and radio host Sindi van Zyl and 'London patient' Adam Castillejo, who has been cured of HIV.
Psychosis in young people with HIV

Psychotic disorders are severe mental health illnesses that lead to a person losing some contact with reality. This affects their ability to function day-to-day. Symptoms are largely described as hallucinations and/or delusions. Hallucinations are when a person senses something that is not real. They might see, hear, taste or feel something that feels very real to them, but is not happening. Delusions happen when a person has strong beliefs that are not shared by other people. A common delusion is someone believing there’s a conspiracy to harm them.
A small UK study has found that cases of psychotic disorders are higher than expected among young people born with HIV. Of 184 young people over the age of 18 living with HIV, 12 (6.5%) had experienced an episode of psychosis. In the general population, rates are below 1% in the same age group.
This is the first study to look into this issue and the possible reasons are not well understood. However, growing up with HIV may expose a person to a number of biological and social factors known to increase the risk of developing psychosis. For example, HIV and opportunistic infections can affect the central nervous system. Many young people born with HIV in the UK have grown up in difficult social circumstances, including racism, poverty and the death of close family members.
The researchers say that healthcare professionals supporting young people born with HIV must consider their mental health support needs and integrate mental health care in HIV services.
PrEP in Europe webinar

On Thursday 17 December (13:00 GMT/14:00 W Europe) PrEP in Europe is holding a webinar on PrEP and the trans community.
The webinar will combine scientific research by, and for, trans people on HIV and PrEP, and the recommendations from PrEP in Europe's recent meeting for European trans advocates.
The webinar will include presentations by Sari Reisner (Harvard Medical School, Boston), Akarin Hiransuthikul (Department of Medicine, Chulalongkorn University, Bangkok), and Dinah Bons (Trans United Europe, Amsterdam).
A plan to end new HIV cases in England
Senior government ministers have backed a plan developed by an independent group, the HIV Commission, to eliminate HIV transmission in England over the next decade. At a launch event, health secretary Matt Hancock committed to reducing new cases by 80% by 2025 and to less than 100 a year by 2030. Michael Gove said that Boris Johnson had asked him to work with Hancock to ensure that the necessary resources are available.
The HIV Commission was set up by Terrence Higgins Trust, National AIDS Trust and Elton John AIDS Foundation to create a plan for meeting the 2030 target. One of its key recommendations is for opt-out HIV testing to become routine in the NHS.
Editors' picks from other sources
SARS-CoV-2 vaccine advice for adults living with HIV: British HIV Association (BHIVA) & Terrence Higgins Trust (THT) guidance – Plain English version | BHIVA
People will receive the vaccine in strict order of priority based on their age, health, occupation, whether they live in a care or residential home and who they live with. Everyone with HIV is automatically in priority group 6 so you will get the vaccine earlier than many people. If your clinic thinks you are at higher risk you can be put into priority group 4, and get the vaccine sooner, but you will need to be added to a central NHS list to be put into priority group 4.
Study explores pain in HIV-positive people | CATIE
Researchers in Ireland and the UK have been studying the issue of pain in HIV-positive people. They found that chronic pain is relatively common in people with HIV, particularly in those aged over 50 years.
Top 10 HIV clinical developments of 2020 | TheBodyPro
In this exclusive series of articles, David Alain Wohl, M.D., calls attention to ten developments that have tremendous short-term implications for our day-to-day efforts to improve HIV prevention, treatment, patient care, and policy in the US, and analyses each development with his trademark wit and clinical savvy.
Tortoise and the hare: Why a COVID vaccine is outrunning its HIV counterpart | Bhekisisa
Four COVID jabs’ efficacy results have been released within less than a year after the trials had started. But this is far from the norm. Researchers have been working on HIV vaccines for over three decades – and we still don’t have one. Here’s why.
