Genetics and kidney disease

The researchers focused on genes called APOL1. Certain types (variants) of the APOL1 gene provide some protection against a parasite that can cause sleeping sickness. Sleeping sickness is common in some parts of Africa which may explain why these gene variants are more commonly found there. But the same gene variants also increase the risk of various forms of kidney disease. The new study shows that this is also the case among people with HIV.
Almost 3000 people of Black ethnicity living with HIV in the UK were enrolled in the study. People’s regions of descent were based on their parents’ countries of birth. These were mostly east African (19%), south African (27%) and west African (30%), with a further 12% of Caribbean ancestry.
The researchers found that 12% of the people in the study had two of the ‘high risk’ APOL1 gene variants (i.e. the ones associated with kidney disease). People with roots in west Africa or the Caribbean were more likely to have these high-risk variants than people from other parts of Africa.
The number of people who had serious kidney disease was small. But the majority of people with kidney disease had two of these APOL1 gene variants. They were found in 55% of people who needed dialysis or a kidney transplant.
We can’t change our genes, so the researchers highlight the importance of paying attention to other risk factors for kidney disease that we can change. These include having a low CD4 count, high blood pressure and diabetes. A healthy diet, exercise, regular blood tests and medication to manage these conditions are all important.
Positive Fitness

We are delighted to launch Positive Fitness, an online exercise class designed to support people living with HIV to get fit and stay active.
Regular physical activity supports health for everyone. It is even more important for people living with HIV as it can help to prevent a range of health conditions that they are more likely to experience.
Our Positive Fitness class is led by SMASH Mind and Body and is suitable for all levels. All of the class participants are openly living with HIV.
Peer support

Many people living with HIV find it helpful to meet other people who are also living with HIV. It can be good to talk to someone with personal experience of what it means to live with HIV who may have been through similar things to you. As well as happening informally and in support groups, some HIV clinics help to arrange what is known as ‘peer support’.
Researchers talked to people living with HIV about their experience of getting peer support at outpatient HIV clinics in Norway. At these clinics, the support was ongoing, flexible and individualised. The peer supporters were chosen from clinic users, and were both trained and paid.
For many of the people interviewed, confidentiality was an important issue. For them, the outpatient clinic was the only safe place to discuss HIV and having peer meetings there was valued. Many of the interviewees were not open about their HIV status, which shaped their need for peer support. People who were more open about having HIV felt less need for peer support.
Talking to peers living with HIV provided a sense of belonging. It offered an opportunity for participants to share their worries with others living with HIV, as this person said:
“It gave me an understanding in a completely different way, and it made it less scary. It became easier to grasp. When you hear that they recognise what you feel... they tell you that it is completely normal to feel like this. You then understand why you feel it.”
Being told something by another person living with HIV is different to being told it by a medical professional:
“The doctor has told me several times that you do not have to believe that you will die right away. However, this is not understood inside here [pointing to the head and heart]... I had a very nice doctor, but I believed nothing of what he said. However, when I got to talk to someone living with HIV, I realised that it worked.”
aidsmapCHAT

On Monday's episode of aidsmapCHAT, Susan Cole and Matthew Hodson were joined by Jacquelyne Alesi from the Prevention Access Campaign, Andy Seale from the World Health Organization and Dr Michael Brady from NHS England.
The final episode in this season of aidsmapCHAT will be broadcast on Monday 20 June at 6pm (UK time) on Facebook and Twitter.
Monkeypox
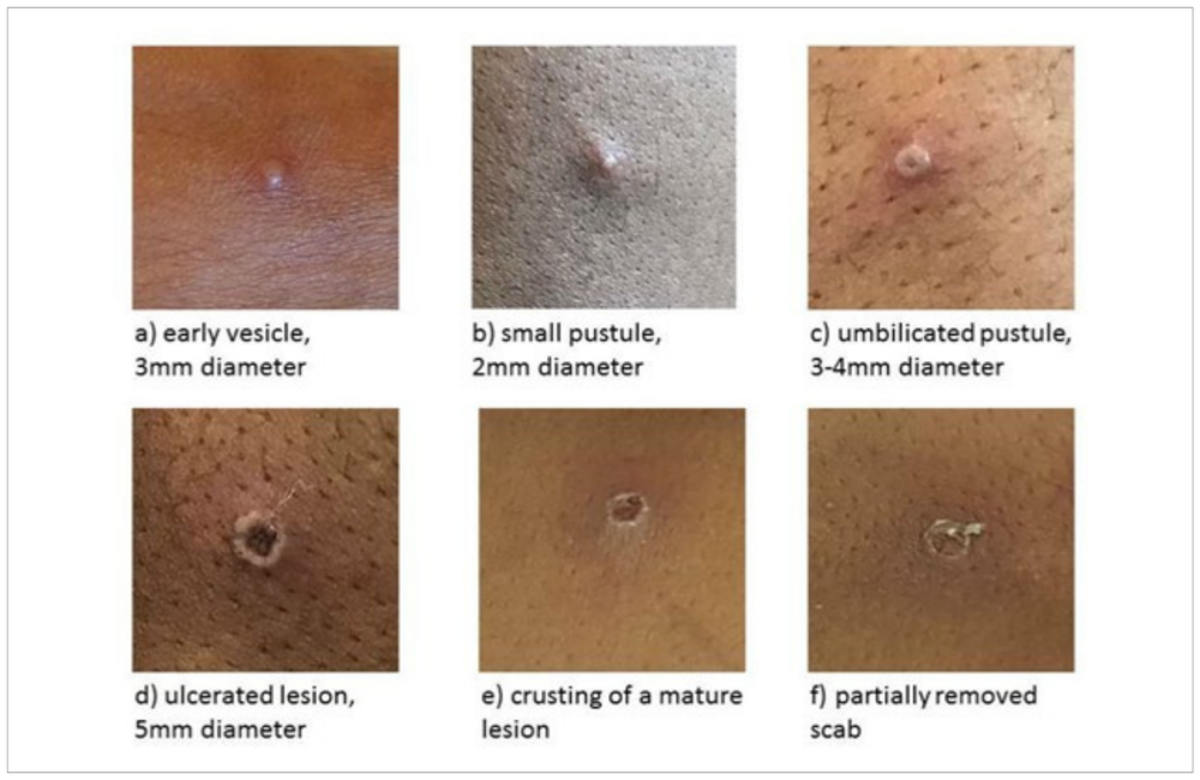
The spread of monkeypox in countries outside of Africa continues. While most cases so far are among gay and bisexual men, health officials emphasise that anyone can contract the virus through close personal contact.
Health officials are asking anyone with an unusual rash or lesions on any part of their body, especially their genitals, to contact their healthcare provider or a sexual health clinic. People who think they may have monkeypox are advised to avoid close social contact until they get tested.
People with monkeypox usually recover without treatment. So far, it seems that people with well-controlled HIV are not more likely to have serious illness compared to other people. But people with advanced and untreated HIV may be at a higher risk. The modern vaccine against smallpox (which also protects against monkeypox) has been tested and shown to be safe for people with HIV.
Hepatitis C treatment factsheets
We have updated all our hepatitis C treatment factsheets on our hepatitis website infohep.
Read about how the treatments work, who can use them, how they're taken, side effects and drug interactions.
Health conditions

A large study looking at medical records in UK primary care services gives a comprehensive picture of the health concerns of people living with HIV in recent years. Close to a million GP records were included, representing 1.8% of the UK population over 18. Of these, 964 had HIV.
The most common conditions were experienced in similar numbers in people with HIV and people without HIV. There were large numbers of people with HIV who had raised cholesterol or triglycerides (41%), skin conditions (39%), gynaecological or sexual health problems (30%) and gastrointestinal conditions (24%).
But people with HIV were more likely to have some of the rarer conditions. Many of these are infections – suggesting the influence of impaired immune systems in people with HIV. For example, fungal infections were seen in 0.05% of the general population but 5% of the people with HIV.
Tuberculosis, viral hepatitis and gastrointestinal infections were all much more common in people with HIV.
Infertility problems, immune disorders and blood problems such as anaemia were all more common in people with HIV. Several mental health conditions, including depression, drug or alcohol dependency and bipolar disorder were much more common in people with HIV. (Rates of mental health problems were looked at in more detail in another recent study.)
At the same time, several conditions were less common than in the general population. For instance, rheumatoid arthritis was only a quarter as common in people with HIV as in people without it, even though autoimmune processes are involved in both. The more common form of arthritis, osteoarthritis, and other bone/joint problems such as carpal tunnel syndrome and wrist fracture were also less common.
Several conditions related to cardiovascular disease were also less common in people with HIV including high blood pressure, atrial fibrillation and coronary artery disease.
Editors' picks from other sources
550… and counting | The Nation
Gregg Gonsalves: "Monkeypox is not a gay disease. But it has arrived in our community – and our decades of experience dealing with HIV give us the chance to get things right from the outset."
Born with HIV: disclosure during adolescence does not harm mental health | Be In The Know
South African study finds adolescents who learn they have HIV are no more likely to experience mental health issues than those who remain unaware.
Chile apologises to woman forcibly sterilised for HIV status | Associated Press
Chile’s president publicly apologised to a woman who was sterilised without her consent at a public hospital two decades ago because she was HIV positive, ending a years-long legal process that included taking her case to the Inter American Commission on Human Rights.
Using antibiotics to prevent STIs found effective in early SF study results | San Francisco Chronicle
Researchers studying the use of antibiotics to prevent sexually transmitted infections in high-risk individuals abruptly stopped enrolling new participants in a clinical trial after early results showed the intervention was effective and it would be unethical not to offer it more widely.
