Undetectable viral load and criminalisation of HIV transmission

In England, Wales and Northern Ireland, not telling a sexual partner that you have HIV is not viewed as a sexual offence. This is unlike Scotland and several other countries that criminalise HIV non-disclosure. However, in some circumstances, transmission of HIV can be viewed as a form of grievous bodily harm that can result in criminal charges.
Almost all cases taken to the court in England, Wales and Northern Ireland are of ‘reckless’ transmission. In the law, ‘reckless’ doesn’t mean that the person passed on HIV deliberately, but that HIV was transmitted and the person didn’t try to stop it from happening.
Until now, it has been clear that the person with HIV would have a legal defence if condoms were used. In other words, if the condom failed and HIV was passed on, the court would find that the person with HIV was not being ‘reckless’ – they had tried to stop HIV from being passed on.
But what about having an undetectable viral load? Can a person with HIV rely on their undetectable status as a legal defence?
Until last week, this was not clear. But new Crown Prosecution Service guidance clearly states that when someone has an undetectable viral load, “the current medical consensus is that there is no risk of HIV transmission, even where no condoms are used”.
As a result, from now on, cases should no longer be taken to court in England and Wales when a person has an undetectable viral load and is aware that Undetectable = Untransmittable (U=U).
This change is a result of several years of lobbying by the National AIDS Trust (NAT) and other advocates.
Transmission facts

HIV can only be passed on when one person's body fluids get inside another person.
Our easy-to-read and illustrated page on HIV transmission shares the ways in which HIV can be passed on, and the activities where there is no risk of HIV transmission.
An A4 version can be downloaded and printed out from the clinic portal, for members of our patient information subscription scheme.
Injectable HIV treatment
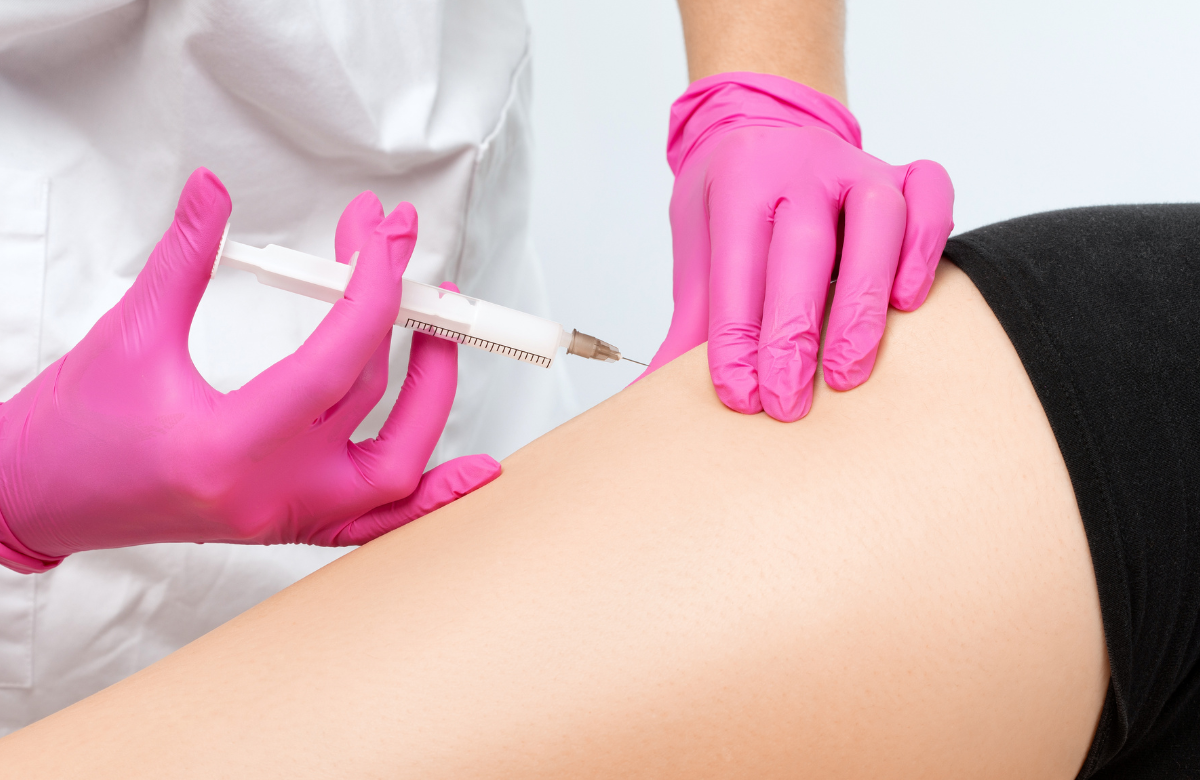
The medications cabotegravir and rilpivirine, taken by injection once monthly or every other month, provide the first complete antiretroviral regimen without daily pills. In Europe, the drugs are known as Vocabria and Rekambys respectively, whereas in North America and Australia they are marketed together as Cabenuva.
The studies showing that the injections are effective were all done in people whose HIV was already under control on a standard oral antiretroviral regimen. As a result, drug regulators and treatment guidelines say that the injections should only be used by people in this situation.
Injectable treatment may seem to have advantages for people who find adherence to daily pills challenging or whose current HIV treatment is not working. But the requirement to already have an undetectable viral load means that people in these circumstances haven’t been able to use it.
Clinicians in San Francisco decided to go beyond drug regulators’ requirements and try the injections with a group of people who have struggled with standard HIV treatment. Their HIV clinic takes care of many people facing challenges with low incomes, homelessness, substance use and poor mental health. Importantly, the clinic has enough staff to offer holistic care and support, and this may have been key to their success with the injectable treatment.
A majority of the 57 people who had detectable HIV at baseline had never achieved viral suppression with oral therapy. With extensive support from the clinic, 55 people in this group achieved an undetectable viral load after switching to the injections.
Larger studies will be needed before this approach will be officially recommended. In San Francisco, people started out with monthly injections, but they could switch to injections every other month if things went well. However, in the UK and Europe, only the dose required for injections every other month is available, and this would be riskier if people are late or miss a dose.
Another challenge with injectable HIV treatment is that the injections are given into the muscle of the buttocks by a healthcare professional. As cabotegravir and rilpivirine must be injected into a large muscle, it has been thought that the buttocks are the only feasible part of the body. But there is work being done to see if injection into the thigh is possible – and this might open up possibilities for people to inject themselves, without needing to go to a healthcare professional.
In a new study, healthcare professionals provided thigh injections for four months to 118 people who had previously been having injections in the buttocks. After injection, drug levels were similar for injection in the thighs or buttocks. Some people preferred having the injections in the thighs, but more people preferred the buttocks. People generally preferred the site they found less painful (for some this was the buttocks, for other people the thighs), and those who preferred thigh injections also often said they were more convenient.
Where did HIV come from?

Human immunodeficiency virus (HIV) is a zoonosis – an infection that originated in animals and passed into human hosts. HIV is closely related to the simian immunodeficiency virus (SIV) found in chimpanzees in central Africa.
Find out more about where HIV came from and what caused it to spread in our new research briefing.
HIV treatment and heart disease

Integrase inhibitors are a modern group of anti-HIV medications that are very widely used, especially dolutegravir (Tivicay, also included in Triumeq, Dovato and Juluca) and bictegravir (included in Biktarvy). Two slightly older integrase inhibitors are raltegravir (Isentress) and elvitegravir (included in Stribild and Genvoya).
The reason these medications are so widely used is that they have a particularly powerful effect against HIV while having fewer side effects than their alternatives. This is why there was concern last year when a large study linked these medications with serious heart disease and strokes.
As with any new type of medication, large-scale study of their effects on heart disease takes time. Although integrase inhibitors are less likely to cause increases in cholesterol than other medications, weight gain is often seen in people starting HIV treatment with an integrase inhibitor. This might raise the risk of heart disease.
A new study is more reassuring. Researchers assessed the risk of a serious cardiovascular event (stroke, heart attack or an invasive procedure such as angioplasty or stenting) in over 5000 people with HIV who started HIV treatment in Switzerland from 2008 onwards. A third of them took an integrase inhibitor.
Over half the people remained in the study for at least five years. During follow-up, there were 116 serious cardiovascular events overall. After adjusting for other factors that could affect the results, people using an integrase inhibitor were no more likely to have a serious cardiovascular event than other people.
The researchers believe that differences in the way the studies were done probably explain the different results. They believe there were potential biases in previous studies on this topic.
HIV and the heart
We have recently published six new or updated pages on HIV and the heart.
Find out about high blood pressure and cholesterol, as well as coronary heart disease, heart attack, stroke and peripheral artery disease.
Mpox (monkeypox) in people with low CD4 counts

Mpox (formerly known as monkeypox) can be much more severe in people living with HIV who have a very low CD4 count – so much so that some experts are calling for it to be classified as an AIDS-defining infection.
In last year’s outbreak of mpox in Europe and North America, a substantial number of the people affected were living with HIV. Most were taking HIV treatment, had an undetectable viral load and a healthy CD4 cell count. In these cases, mpox was no more dangerous than for people who don’t have HIV.
Now researchers have looked more closely at the impact of mpox in 382 people living with HIV who all had a CD4 cell count below 350. Many had very low CD4 counts, indicating a severely weakened immune system – a quarter had between 100 and 200 CD4 cells and a fifth had fewer than 100. These people came from 19 countries all around the world, including many in Latin America.
Although about 90% were people previously diagnosed with HIV, just 60% were taking HIV treatment and only half had an undetectable viral load. Only 7% had received an mpox vaccine.
Many people had distressing symptoms, including large rashes and lesions all over their bodies. Severe symptoms and complications affecting internal organs were more common in those with the lowest CD4 counts.
A little under a third of the people needed hospital care and 27 people died. All of those who died had a CD4 count below 200, and most had a CD4 count of less than 100.
“When I saw the fatality rate, I felt horrified,” Professor Chloe Orkin told aidsmap. “If there’s someone in your life who hasn’t had an HIV test and may have low CD4 count without knowing it, if they get mpox it could have catastrophic outcomes.”
The only encouraging finding is that no one with well-controlled HIV and no one who received an mpox vaccine died, which suggests that starting and staying on HIV treatment can prevent severe outcomes.
But Professor Orkin warned that doctors who care for untreated patients with severe mpox need to be alert for immune reconstitution inflammatory syndrome, or IRIS. This is a worsening of symptoms that can occur when people start antiretrovirals with a very low CD4 count.
aidsmapLIVE: mpox special

Last month, we broadcast our first aidsmapLIVE of 2023.
In our mpox special, NAM aidsmap's Susan Cole spoke to Professor Chloe Orkin from Queen Mary University of London; Dr Mateo Prochazka from the World Health Organization; HIV advocate Harun Tulunay, who had severe mpox in 2022; Dr Will Nutland from PrEPster and The Love Tank CIC; and Michael Akanji from the African Key Populations Expert Group.
Editors' picks from other sources
UK: Illegal Migration Bill could be ‘death sentence’ for people on HIV/AIDS medication, MPs warn | Pink News
MPs debating the controversial Illegal Migration Bill have warned that a lack of provision for those receiving treatment for HIV/AIDS would effectively be a “death sentence”.
HIV advocacy on Tik Tok | POZ
TikTok continues to delight its users, especially young people. Some of them are also using the platform to spread awareness of HIV and sexual health.
HIV charity that supported thousands in Scotland over 30 years to close | Metro
HIV Scotland has not given the exact reason for its closure but issued a statement on its website citing a ‘number of significant challenges’. This has included ‘some recent changes within the organisation’s governance which have caused concern’.
WEP Clinical has partnered with TaiMed Biologics to launch a Trogarzo named patient programme | WEP Clinical press release
The Named Patient Program is designed to ensure that physicians in Europe and other regions around the world, where Trogarzo (ibalizumab) is not commercially available, can request Trogarzo on behalf of individual patients who have trouble achieving viral suppression using standard HIV regimens.
Swift condemnation for ‘world worst’ Uganda Anti-Homosexuality Act | Health Policy Watch
UNAIDS has warned that, if the Act becomes law, it will curtail “the human rights of people living with HIV and some of the most vulnerable people of Uganda to access life-saving services”.
