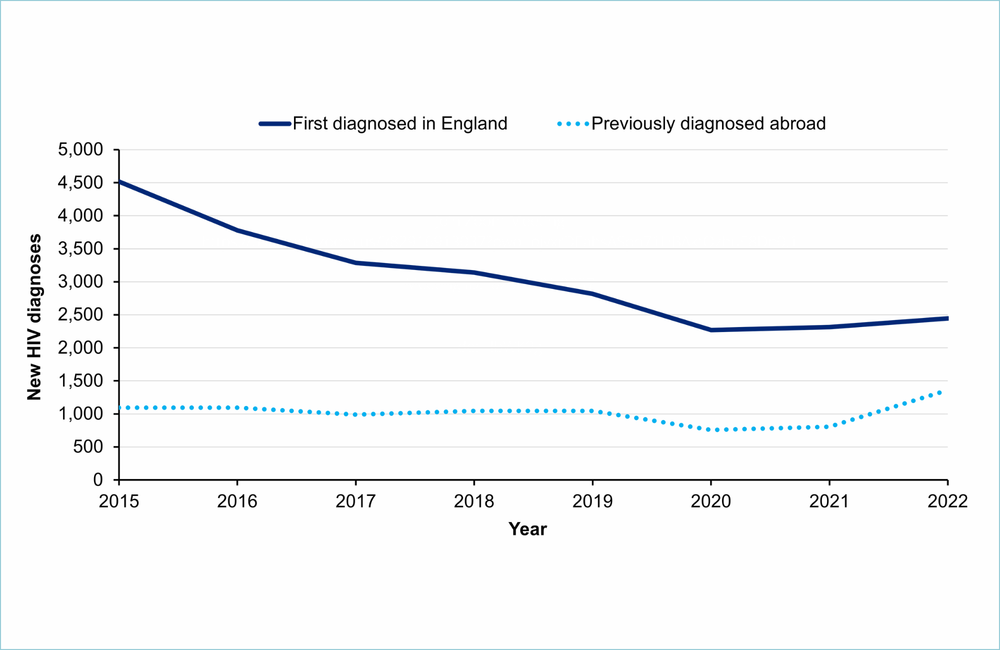
HIV diagnoses rose in England in 2022, but much of the increase was due to the arrival of people with HIV already on antiretroviral treatment rather than an increase in HIV transmission, the UK Health Security Agency reported today in its annual report on HIV in England.
New HIV diagnoses (cases not diagnosed previously abroad) increased by 12% in heterosexual men and women but continued to decline in gay and bisexual men.
However, the Health Security Agency warns that any changes in the HIV statistics need to be interpreted with caution due to ongoing challenges in collecting data as a result of the COVID-19 pandemic.
They also note that the COVID-19 pandemic and the mpox outbreak in 2022-23 have affected sexual behaviour, patterns of HIV testing and access to sexual health services.
Almost all data in the report describe the situation in England. Public Health Scotland published a Scottish report last week (see below).
HIV diagnoses
Overall, HIV diagnoses rose by 22% in 2022. This increase is largely attributable to a 69% increase in the number of people with HIV previously diagnosed abroad and subsequently diagnosed again in England. Two-thirds (67%) arrived in England in 2022. Encouragingly, most of these individuals were rapidly linked to care, with 91% receiving care within one month of diagnosis. Moreover, 87% of them were virally suppressed at the time of their diagnosis in England.
The long-term downward trend in HIV diagnoses in gay and bisexual men continued. New HIV diagnoses (cases not diagnosed previously abroad) fell by 8% in gay and bisexual men, from 784 in 2021 to 724 in 2022. The decline was greater outside London (down 10%) than in London (down 3%). New HIV diagnoses fell by 17% among White gay and bisexual men but rose by 17-25% among men of Asian or mixed ethnicity. Forty percent of new diagnoses in gay and bisexual men occurred in ethnic groups other than White in 2022 compared to 35% in 2021.
New HIV diagnoses (cases not diagnosed previously abroad) attributed to sex between men and women increased by 12% from 870 in 2021 to 976 in 2022. Diagnoses in women rose by 26% but fell in men by 3%. The increase in new diagnoses among women exposed through sex between men and women was greater outside London (up 31%) than in London (up 16%).
HIV testing
In 2022, 192,503 gay and bisexual men took an HIV test, a 23% increase on 2019 and the highest number ever. But testing levels in heterosexual men and women were still below 2019 levels (69% and 81% of 2019 levels respectively).
Half of all HIV tests were taken by people ordering through internet services compared to 19% in 2019. Although 48% of eligible attendees at sexual health services were tested for HIV in 2022, this figure remains lower than the 2019 rate of 65%.
HIV care and treatment
There were 94,397 people living with diagnosed HIV and accessing care in the UK in 2022, a rise of 3% from 91,368 in 2021. Among those diagnosed in 2022, the median CD4 count at diagnosis was 361, a slight increase compared to 2021. Forty-four percent of people diagnosed with HIV had a CD4 count below 350 (late diagnosis) and the total number of late diagnoses was 27% higher in 2022 than in 2020. Late diagnosis was more common in men exposed to HIV through sex with women (57%) than in women exposed through sex with men (52%) or gay and bisexual men (37%).
Ninety-eight percent of people with HIV accessing care were taking antiretroviral treatment in 2022. Viral load results were available for 93% of those on treatment and of these, 98% were virally suppressed. Viral suppression was lower in those exposed through vertical transmission (91%) or injecting drug use (94%). There was no substantive difference in treatment or viral suppression by ethnicity.
Half of all people with HIV accessing care in England in 2022 were aged 50 and over, compared to 27% in 2013.
PrEP use in the UK
The proportion of HIV-negative people accessing sexual health services in the UK who were defined as at substantial risk of HIV and in need of PrEP increased from 7.5% (88,216 of 1,183,155) in 2021 to 9.7% in 2022 (121,547 of 1,249,511). In 2022, this equates to 83,223 gay and bisexual men, 2,607 heterosexual men and 2,695 heterosexual and bisexual women.
In 2022, 71% of people in need of PrEP started or continued PrEP (72,457 gay and bisexual men, 1,599 heterosexual men and 1,676 heterosexual and bisexual women)
Scotland
The majority of HIV diagnoses reported in Scotland in 2022 had been previously diagnosed elsewhere (209 of 317).
The long-term downward trend in HIV diagnoses among gay and bisexual men continued in Scotland too. Scotland recorded 31 new HIV diagnoses in gay and bisexual men in 2022 compared to 63 in 2022. Testing for recent HIV acquisition could be carried out in 25 cases; only four were judged to have been acquired in the previous three to four months.
New HIV cases acquired through sex between men and women increased from 20 in 2021 to 45 in 2022, but the number of new diagnoses attributable to sex between men and women remained below the 2019 level (59) and the level of diagnoses during the previous decade.
By December 2022, approximately 6,600 people were living with HIV in Scotland, of whom 93% had been diagnosed. Eighty-four percent of those diagnosed had attended HIV services for care between July 2021 and December 2022, 98% of those attending were receiving antiretroviral treatment and 93% of those had suppressed viral load.
The number of people accessing PrEP in Scotland has grown. Between July and December 2022, 1,142 individuals accessed HIV PrEP for the first time, an average of 190 per month. This is the highest number in any six-month period since the Scottish PrEP programme began in July 2017.
UK Health Security Agency. HIV testing, PrEP, new HIV diagnoses and care outcomes for people accessing HIV services: 2023 report. Published online 3 October 2023.
Public Health Scotland. HIV in Scotland. Update to 31 December 2022. Published online 26 September 2023.

