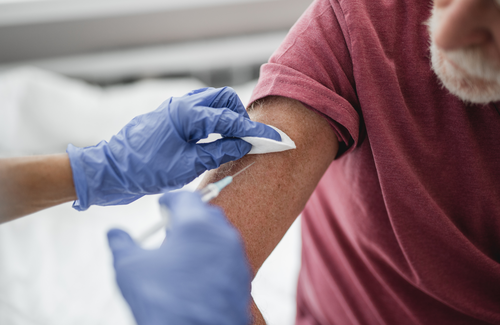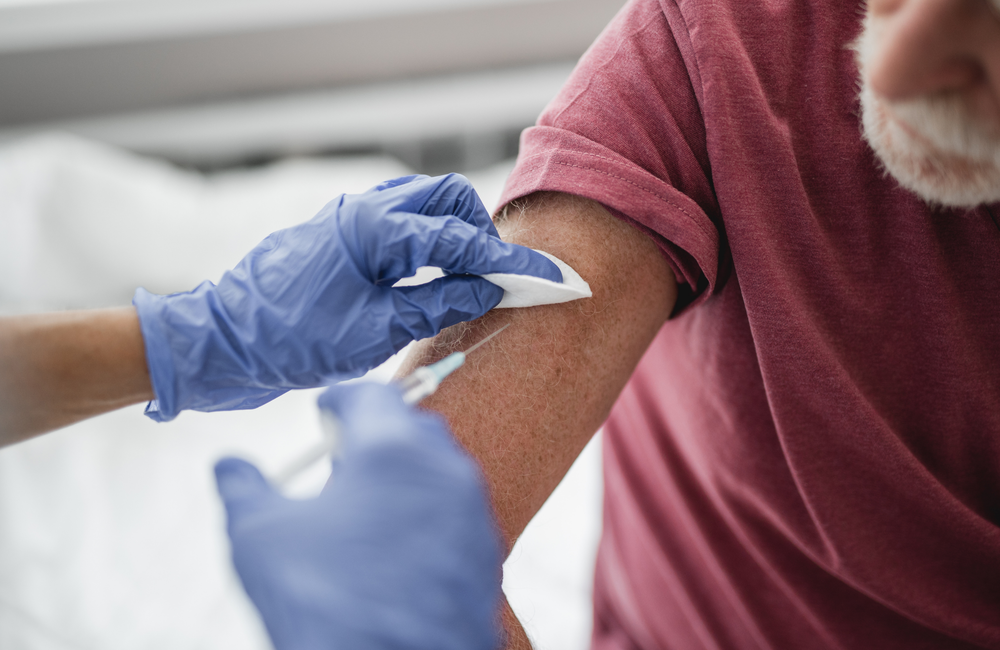
Two studies of immune responses to the Oxford/AstraZeneca COVID-19 vaccine show that the vaccine produced similar immune responses in people with or without HIV. People with HIV did not experience more side effects from the vaccine.
The findings have been made available as pre-prints, which means that they have not been peer-reviewed yet.
There is some evidence that people with HIV have weaker or less durable responses to various vaccines, including the annual flu vaccine and some hepatitis B vaccines. But the quality of immune responses produced by any of the COVID-19 vaccines licensed for use is unknown in people with HIV.
Two research groups have now reported on responses to the Oxford/AstraZeneca vaccine (ChAdOx nCov-19).
London
As part of the phase 2/3 study of the Oxford/AstraZeneca vaccine, a sub-study in people with HIV was carried out, led by Professor John Frater of the University of Oxford. It recruited 54 people with HIV at hospitals in London and all received the vaccine. Results were compared with a control group of 50 HIV-negative people drawn from the larger vaccine study.
People with HIV were eligible to join the study if they were aged 18-55 years, on antiretroviral treatment with a fully suppressed viral load (< 50 copies/ml) and a CD4 count above 350. The study excluded people with previous COVID-19 infection, confirmed by SARS-CoV-2 antibody testing.
The 54 people with HIV were all male whereas the control group was evenly split between men and women. Participants in both groups were approximately 80% White. The median CD4 count in people with HIV was 694.
Participants received two standard doses of the vaccine four to six weeks apart. (The 12-week interval between doses was adopted in some countries after a secondary analysis of the phase 2/3 trial showed that this schedule was associated with greater protective efficacy.)
"Further data are needed in people with CD4 counts below 350 or detectable viral load."
Participants were followed for 56 days after their first jab and blood samples for immunological tests were taken at baseline and on days 14, 28, 42 and 56. Samples were tested for the number of antibodies to the SARS-CoV-2 spike protein, the neutralising capacity of the antibodies (how well the antibodies reduce virus-infected cells), the quantity of virus-specific T-cells and their ability to proliferate in the presence of the SARS-CoV-2 spike protein.
Tests showed no differences in antibody or cellular immune (T-cell) responses between people with HIV and the HIV-negative control group at any point after vaccination. Antibody responses were not affected by CD4 count in people with HIV. Immune activation in people with HIV did not affect antibody or cell-mediated responses.
The study also compared adverse reactions between people living with HIV and the HIV-negative control group, finding no significant difference in the incidence of the most common reactions such as injection site pain (reported by 49% of people with HIV), fatigue (47%), headache (47%) and muscle or joint pain (36%). The incidence of most reactions was lower after the second jab.
“The measured immunological responses are similar to those seen in HIV negative participants for whom there is increasing evidence that vaccination leads to a reduction in symptomatic cases and hospitalisations,” the authors conclude. They say that the findings show that people with HIV should be supported to receive the vaccine and do not need a different vaccination regimen from the rest of the population. However, they warn that further data are needed in people with CD4 counts below 350 or detectable viral load.
South Africa
The second study was carried out in South Africa, as part of the phase 1b/2a safety and immunogenicity studies for the Oxford/AstraZeneca vaccine. People with HIV were eligible to join the study if they were on antiretroviral treatment and had a viral load below 1000 copies/ml. The study randomised participants to receive the Oxford/AstraZeneca vaccine or a placebo injection in two doses, 28 days apart.
The study enrolled 104 people with HIV and 70 people without HIV. Twenty-six per cent of people with HIV were men compared to 62% of HIV-negative people. All participants but one were Black. The median age of participants with HIV was 40 years, whereas HIV-negative participants were younger (32 years). Most of those living with HIV had an undetectable viral load and a median CD4 cell count of 695.
The study measured antibody responses to the vaccine in people with HIV, as well as safety. It found no difference in antibody responses between people with HIV and HIV-negative people 28 and 42 days after the first dose.
There was no difference in the frequency of adverse reactions between people with and without HIV. Mild or moderate headache, joint or muscle pain and weakness were each reported by around a quarter of recipients of the vaccine after the first dose – but most of these effects were almost as common in the placebo group. Fever and chills were uncommon reactions to the vaccine in this population.
Participants with HIV who tested positive for SARS-CoV-2 by PCR testing (indicating active infection) after randomisation showed stronger antibody responses after one dose than seen in HIV-negative participants after two doses (approximately six times higher). A similar pattern has been observed in HIV-negative people who received a first dose of the Pfizer or Moderna vaccines.
The researchers say that while the vaccine produced strong antibody responses against SARS-CoV-2 in people with high CD4 counts, the results may not be generalisable to people with CD4 counts below 500. They also highlight the need for further studies of vaccine efficacy in people with HIV in Africa.
Frater J et al. Safety and immunogenicity of the ChAdOx1 nCoV-19 (AZD1222) vaccine against SARS-CoV-2 in HIV infection. SSRN pre-print, posted online 19 April 2021.
Update: Following the pre-print, this research was published in a peer-reviewed journal:
Frater J et al. Safety and immunogenicity of the ChAdOx1 nCoV-19 (AZD1222) vaccine against SARS-CoV-2 in HIV infection: a single-arm substudy of a phase 2/3 clinical trial. The Lancet HIV, 8: e474-e485, June 2021. DOI: https://doi.org/10.1016/S2352-3018(21)00103-X
Madhi S et al. ChAdOx1 nCoV-19 (AZD1222) vaccine in people living with and without HIV. Research Square pre-print, posted online 17 March 2021.
Update: Following the pre-print, this research was published in a peer-reviewed journal:
Madhi S et al. Safety and immunogenicity of the ChAdOx1 nCoV-19 (AZD1222) vaccine against SARS-CoV-2 in people living with and without HIV in South Africa: an interim analysis of a randomised, double-blind, placebo-controlled, phase 1B/2A trial. The Lancet HIV, 8: e568-e580, September 2021. DOI: https://doi.org/10.1016/S2352-3018(21)00157-0