In just two years, the incidence of new HIV infections in men who have sex with men attending English sexual health clinics fell by 55%, according to data presented by Dana Ogaz of Public Health England at the Conference on Retroviruses and Opportunistic Infections (CROI 2019) in Seattle today.
Modelling studies have previously suggested that incidence began to fall in 2012 and reports of new diagnoses have been falling since 2014. The figures presented today come from routinely collected data from gay, bisexual and other men who have sex with men (MSM) who attend the same sexual health clinic twice or more in the same year. In any given year, this is around a third of the MSM who use the clinic. However, they may not be representative of the wider population of MSM.
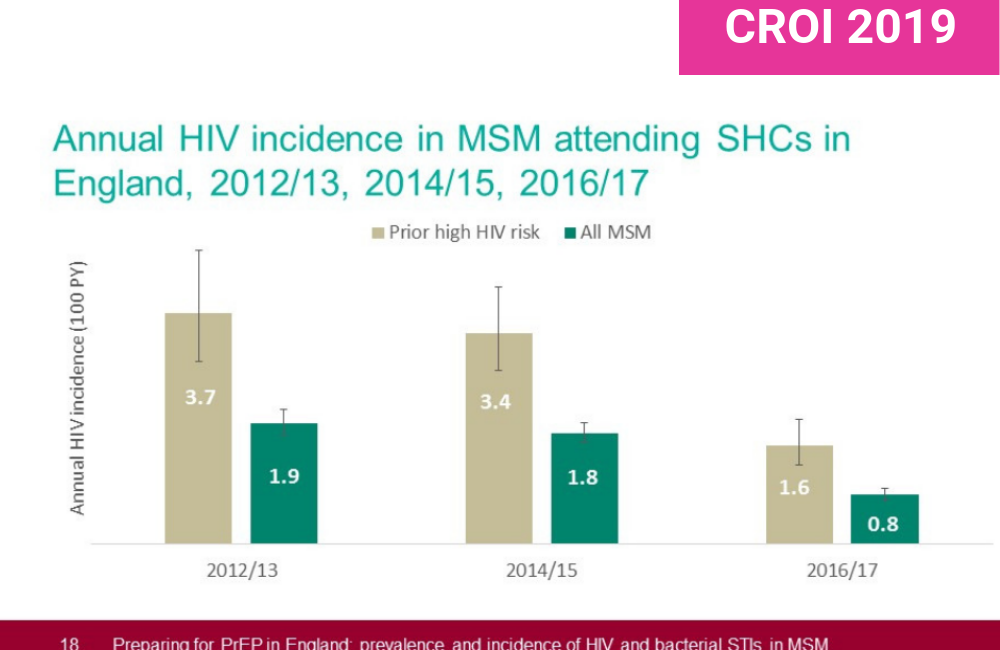
Incidence was measured in 2012-2013, then in 2014-2015, and again in 2016-2017. In the first year, incidence was 1.9% (meaning that two in every 100 men acquired HIV during the year), remaining stable at 1.8% in the second time period. But just two years later, incidence was only 0.8%.
A similar pattern was seen in MSM who had both had an HIV-negative test and a bacterial STI in the past year – a group at higher risk of HIV infection. Incidence fell from 3.7% to 3.4% and then to 1.6% (a 53% fall in the last two years).
Over this time period, diagnoses of sexually transmitted infections have been rising. Between 2012 and 2017, there was a 90% increase in gonorrhoea diagnoses, 80% increase in chlamydia diagnoses and 160% increase in syphilis diagnoses among gay men attending sexual health clinics.
In 2017, 12.1% of gay men attending clinics had gonorrhoea (a third had a rectal infection), 9.0% chlamydia (half had a rectal infection) and 2.7% had syphilis.
The fall in HIV diagnoses coincides with a period when increasing numbers of men accessed pre-exposure prophylaxis (PrEP), while efforts to improve testing and prompt initiation of HIV treatment continued.
Ogaz said Public Health England conducted the exercise in order to provide a baseline for monitoring infections as the country rolls out PrEP. She said that as the situation evolves, untangling the contribution of PrEP to already falling HIV incidence and increases in STI diagnoses will require careful consideration.
Ogaz D et al. Preparing for PrEP in England: prevalence and incidence of HIV and bacterial STIs. Conference on Retroviruses and Opportunistic Infections, Seattle, abstract 48, 2019.
View the abstract on the conference website.
Watch the webcast of this presentation on the conference website.
