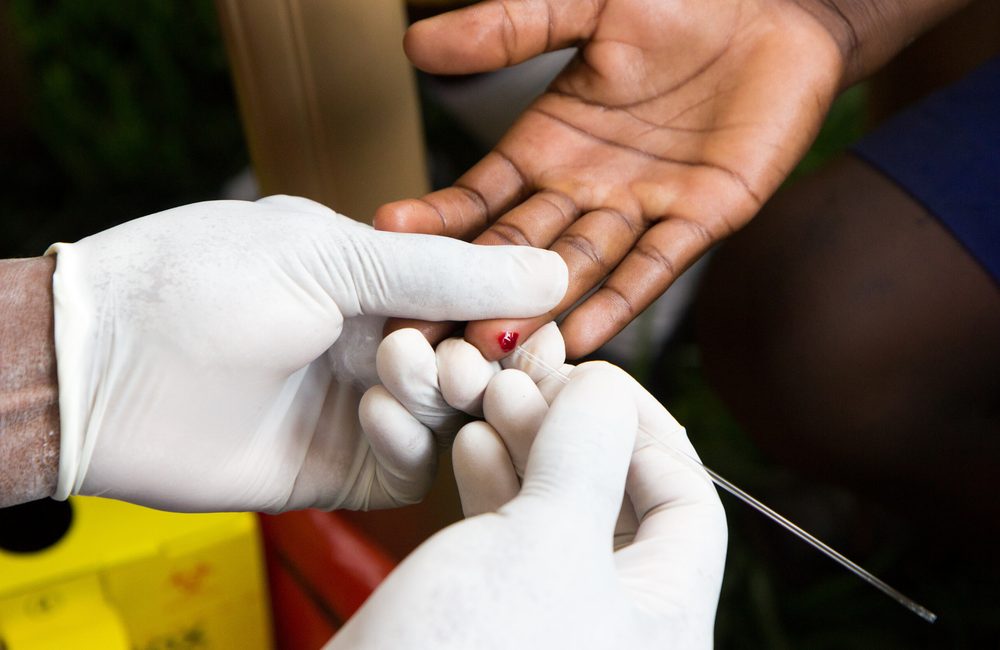
Socioeconomic inequalities in the uptake of HIV testing have persisted despite the massive scale-up of HIV testing in sub-Saharan Africa, according to a study by Pearl Anne Ante-Testard published in the June issue of The Lancet Global Health. People living in the richest households were around three times as likely as those in the poorest households to have tested for HIV in the previous year.
“Inequality in access to HIV testing is relevant from not only a human rights perspective but also an epidemic control perspective, particularly if the people who do not get tested are at higher risk of HIV infection,” say the authors of a linked comment article. “HIV programmes therefore need to carefully review who is being reached by their services and to implement interventions specifically tailored to engage people who might be missed.”
The study
Data were taken from the Demographic and Health Surveys, which are nationally representative cross-sectional surveys collecting data on a wide range of health issues in low- and middle-income countries.
The researchers selected sub-Saharan African countries where at least two surveys with relevant data had been done – one prior to 2008 (before the global scale-up of HIV testing) and one after that date. Sixteen countries had eligible data: Cameroon, Côte d'Ivoire, Democratic Republic of Congo, Ethiopia, Guinea, Kenya, Lesotho, Liberia, Malawi, Mali, Niger, Rwanda, Sierra Leone, Tanzania, Zambia and Zimbabwe. In the majority of countries, the most recent surveys had been done between 2012 and 2014, with none done after 2016.
Wealth was assessed at the unit of the household by taking into account assets and characteristics, such as televisions, access to water and electricity, type of floor, number of rooms, and agricultural land. Individuals from the poorest 20% of households were compared with individuals from the richest 20%.
Over half a million people took part in the surveys.
Key findings
Gender differences increased over time. A higher proportion of women than men had recently tested in five of the 16 countries in the pre-2008 surveys, and in 14 of 16 countries in the later surveys. This probably reflects the scale-up of HIV testing in antenatal clinics.
In both men and women, there was a pattern of higher uptake of testing by richer people than poorer people. Relative inequalities were sharper in men than in women: overall, in the more recent surveys, the wealthiest female participants were 2.8 times more likely to report HIV testing in the previous 12 months than the poorest participants (95% confidence interval 1.4-5.4). The corresponding ratio among male participants was 3.6 (95% CI 1.9-6.8).
Inequalities were also observed in relation to education and location (favouring urban over rural residents), but the wealth inequalities persisted even when these other factors were statistically adjusted for.
The researchers investigated how wealth inequalities changed over time, by comparing data from surveys done before and after 2008. Over time, inequalities decreased significantly, especially in women. In the surveys done before 2008, the wealthiest women were 9.8 times more likely to test, reducing to 2.8 in more recent surveys. In the earlier surveys, the wealthiest men were 7.3 times more likely to have recently been tested, reducing to 3.6 in the post-2008 surveys.
Why are some countries doing better?
Inequalities tended to be greater in western and central African countries than in eastern and southern African countries. Over time, they reduced in countries such as Malawi, Rwanda, Zambia, and Zimbabwe, but rarely seen in western and central African countries. The situation may be easier to grasp by looking at two countries in more detail.
Zambia is a southern African country in which 11% of its 17 million people are living with HIV. Surveys were done in 2007 and 2013-14, with over 30,000 participants taking part in the second one. Reflecting massive investment from global health bodies, HIV testing increased from 21% to 48% in women, and from 13% to 39% in men, between the two surveys.
Inequalities along the lines of wealth decreased between the two surveys and were relatively modest in 2013-14. Among the poorest 20% of women, 43% had tested in the previous year, compared to 46% of the richest women. The comparable figures for men were 36% and 41%.
In the west African country of Côte d’Ivoire, around 2.6% of the 25 million people are living with HIV. Surveys were done in 2005 and 2011-12, with around 15,000 participants in the latter. Recent testing was the exception rather than the norm, but did increase over time, from 5% to 15% in women, and 4% to 10% in men.
Inequalities were marked in the most recent survey. Among the poorest women, 8% had recently tested, with a step-wise increase as wealth increased, up to 23% among the richest women. Recent testing was reported by 4% of the poorest men, rising to 19% of the wealthiest.
"High prevalence countries have prioritised ambitious HIV testing programmes which appear to have reduced health inequalities."
Similarly, 11% of women with no education had recently tested, whereas 25% of those with secondary schooling or more had tested. Comparable figures for men were 4% and 17%. People living in urban areas were twice as likely to have tested as rural residents.
The authors note that countries with a high HIV prevalence, such as Zambia, have prioritised ambitious HIV testing programmes, which appear to have had the effect of reducing health inequalities. Lower prevalence countries, such as Côte d’Ivoire have had less spending on HIV generally and on HIV testing specifically.
“Low-to-moderate efforts to promote and offer HIV testing might perpetuate socioeconomic inequalities in testing uptake, whereas larger efforts might decrease these inequalities, even when they are not specifically targeted at socioeconomically disadvantaged populations,” they comment.
Across the continent, the setting in which the offer of provider-initiated opt-out testing has been scaled up most consistently has been antenatal clinics. This is reflected in a gender gap that became larger over time. The authors suggest that integrating HIV testing into a wider range of clinical settings could help to reduce the effect of socioeconomic inequalities on HIV testing in men and boys.
“Greater priority should be given to socioeconomic equity in assessments of HIV testing programmes,” they conclude.
Ante-Testard A et al. Temporal trends in socioeconomic inequalities in HIV testing: an analysis of cross-sectional surveys from 16 sub-Saharan African countries. Lancet Global Health, 8: E808-818, June 2020 (open access).
DOI: https://doi.org/10.1016/S2214-109X(20)30108-X
Sibanda EL & Taegtmeyer M. Inequalities in uptake of HIV testing despite scale-up. Lancet Global Health, 8: E744-745, June 2020 (open access).
DOI :https://doi.org/10.1016/S2214-109X(20)30208-4
