A study at the 11th International AIDS Society Conference on HIV Science (IAS 2021) is the first to investigate drug levels and drug resistance in people who become infected with HIV despite taking PrEP in the real-world setting of four African countries’ rapidly expanding PrEP programmes.
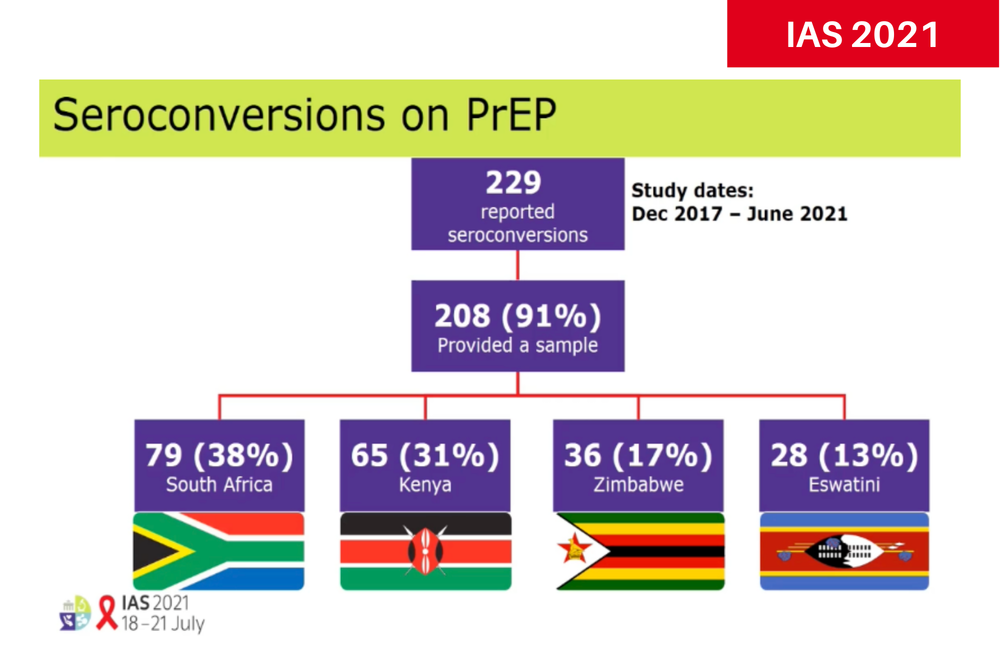
Dr Urvi Parikh of Pittsburgh University told the conference that the GEMS (Global Evaluation of Microbicide Sensitivity) project had found 229 cases of HIV infection among an estimated 104,000 people taking PrEP in South Africa, Kenya, Zimbabwe and Eswatini. This may not be the total number of infections, as some may not have been reported, but it does suggest that HIV infections on PrEP are proving to be rare.
The GEMS study was described as an "observational cross sectional study" meaning that it only investigates the characteristics of cases – people who caught HIV – rather than controls, the vast majority who did not.
This has important limitations, most notably that while drug resistance mutations to the PrEP drugs emtricitabine and tenofovir were detected in people who seroconverted after starting PrEP, the researchers can’t be sure whether they arose as a result of taking PrEP or may in some cases have already been there in the HIV that people acquired.
The rates of drug resistance found were higher than those seen in general among people in the region, but so were the rates of resistance to another class of drugs, NNRTIs, that are not included in PrEP.
Of 229 people seroconverting who were notified to GEMS, 208 (91%) provided a dried blood spot sample. Levels of intracellular tenofovir in the samples were measured, and in 118 (57%) of them, drug resistance genotyping was performed. (The main reason it was not done in the others was because in 30% of samples, viral load was too low.)
Among the 208 people tested for drug levels, 38% were from South Africa, 31% from Kenya, 17% from Zimbabwe and 13% from Eswatini.
Three-quarters of the participants tested for drug levels were women, and half were aged 16-24. The group included partners of HIV-positive people (23%), female sex workers (10%), men who have sex with men (7%), and transgender women or men (6%).
The majority of HIV infections occurred in people who had been on PrEP for some time: 35% acquired HIV in the first three months on PrEP, 40% from three months to a year on it, and 18% in people who had taken it for more than a year.
Among the 118 people tested for drug resistance, 55% had no HIV drug resistance mutations. Another 22% had resistance mutations to drugs other than emtricitabine or tenofovir. These were to the NNRTI drugs nevirapine, efavirenz, rilpivirine and etravirine.
This left 23% (27 people) who had resistance mutations to emtricitabine or tenofovir. All but one person had the M184V/I resistance mutation to emtricitabine. This arises easily and is the most common one seen in people who acquire HIV while on PrEP. Thirteen people had M184V/I alone and ten people had it alongside various NNRTI mutations.
The four others, including the person without M184V/I, had the signature resistance mutation to tenofovir, K65R. Three also had NNRTI resistance; the one who didn’t also had another tenofovir mutation called K70E.
Probably the biggest surprise of the study was that while people who caught HIV while on PrEP and did not have drug resistance tended also to have low levels of tenofovir in their blood – indicating poor adherence – the ones with drug resistance appeared to have good adherence.
Eighty-two per cent of those who had no resistance had levels of tenofovir consistent with taking two or fewer PrEP pills a week, as did 60% of those who only had NNRTI resistance. But 78% of people who had PrEP drug resistance had tenofovir levels consistent with taking four to seven does a week – which should be enough to prevent HIV.
What was the explanation for this? Firstly, resistance only arises when HIV is trying to reproduce in a situation where there are significant drug levels, so people with very low adherence will tend to catch the HIV, but not get the resistance.
Secondly, while samples for the GEMS study were taken on or close to the day of diagnosis, we don’t know how long people had been infected before diagnosis, so some could have acquired HIV during a period of poor adherence or drug supply interruption, but when diagnosed had good adherence. Dr Parikh said that, in the absence of incidence assays, the study will evaluate viral load in seroconverters; very high viral loads would tend to indicate recent infection.
There may also have been a few people who were given ART on the day they were diagnosed and the drug level tests detected this, not PrEP. But it still doesn’t entirely explain why nearly all the people with drug resistance had high adherence.
One question asked was whether the study showed that women on PrEP needed near-perfect adherence to prevent HIV infection, unlike gay and bisexual men. However Dr Parikh said that if so, one would expect that an even higher proportion of people with PrEP drug resistance would be women than the 75% in the overall study. In fact the proportion who were women was somewhat lower – 69%. However, she did agree that the general-population effectiveness of PrEP in women needed further study.
"So as long as PrEP remains effective overall, it is unlikely to contribute more than a small proportion of circulating HIV drug resistance."
The proportion of seroconverters on PrEP who had resistance (23%) was considerably higher than the rate of this type of resistance reported in other people newly diagnosed with HIV (approximately 10%); but then so was the rate of NNRTI resistance. The NNRTI resistance could only have been transmitted, not arisen in response to PrEP, so it is possible that the data on resistance in southern Africa are out of date.
Does this higher level of resistance matter? Firstly, it is important to remember that of the estimated number taking PrEP, the 229 infections represent only 0.22% of the estimated 104,000 PrEP takers. So as long as PrEP remains effective overall, it is unlikely to contribute more than a small proportion of circulating HIV drug resistance.
Secondly, Dr Parikh commented, with dolutegravir-based regimens becoming increasingly common in Africa, the high levels of M184V/I seen might not have a significant clinical on the efficacy of regimens. Even with the rarer tenofovir mutations, which wipe out most of the NRTI drugs, effective and available regimens can be substituted for this class.
The GEMS study is ongoing; Dr Parikh commented that even since her presentation was finalised, 13 new cases of people acquiring HIV on PrEP had been detected and will be evaluated.
Parikh U et al. High rates of drug resistance in individuals diagnosed with HIV in tenofovir disoproxil fumarate (TDF)-based pre-exposure prophylaxis rollout programs in Kenya, Zimbabwe, Eswatini and South Africa. 11th IAS Conference on HIV Science, abstract no OALC01LB02, 2021.
Correction: this article was amended on 16 September 2021 to correct the figures on participants' demographics.

