The latest annual report on HIV diagnosis, treatment and testing in the UK should have come out, as they normally do, in advance of World AIDS Day, 1 December last year. It did not, due to the embargo on government publications during the general election campaign.
Out today, the largely positive findings from Public Health England (PHE) provide evidence, via several different indicators, that new HIV infections within the UK are continuing to fall at such a rate that new diagnoses are outstripping them. Indeed, if new diagnoses continue at the same rate, they will exceed the total number of people with undiagnosed HIV in the UK by 2022, even if you add in the same number of new infections each year.
That won’t happen – because the majority of new diagnoses are now from the minority of people who have had HIV for some time and do not fall into the populations who test frequently, or at all. These are often older people or have come from other countries.
However, the fact that the positivity rate among people who test for HIV, in most populations and in most settings, has more than halved in the last few years shows that, if progress is maintained, the UK could be a very low-incidence country by 2030.
Public Health England cites, as measures we must improve if we are to reach this goal:
- more testing in non-traditional settings such as A&E departments, prisons and via self-testing;
- more consistent testing of people who come to clinics with symptomatic STIs (over a third of STI attendees who fell within HIV testing criteria were not tested last year); and
- instituting routine commissioning of PrEP in England which, it says, may bring about a further “rapid fall in new HIV diagnoses in gay and bisexual STI clinic attendees from 2019 onwards”.
New diagnoses and incidence
The report says that 4453 people were diagnosed with HIV in the UK in 2018, a fall of 29% since 6278 diagnoses in 2014. The decline was most marked in gay and bisexual men, where there was a 35% fall, from 3480 to 2250, during the same period. The fall from the 7887 diagnoses in the peak year of 2004 is 44%.
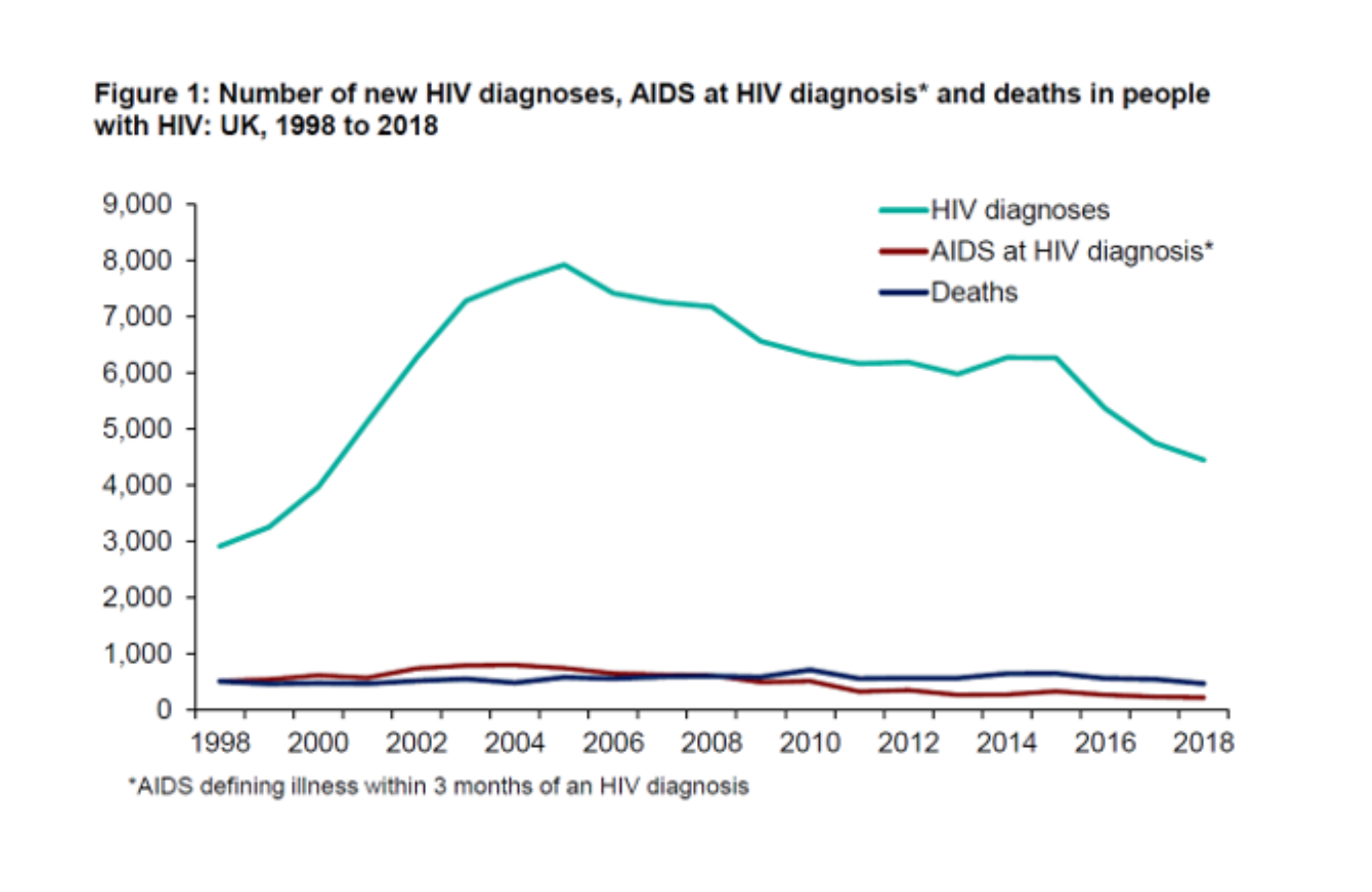
Image credit: Graph from the PHE report
There has been a greater fall in diagnoses of recent HIV infection. The proportion of people for whom incidence assays suggest HIV was acquired in the four months before diagnosis has decreased from 35% to 26%. This enables PHE to estimate that HIV incidence – the real annual rate of new infections, whether diagnosed that year or not – has decreased by no less than 71% in gay and bisexual men since 2012, from approximately 2800 infections in 2012 to just 800 in 2018. Between 2014 and 2018, incidence fell by 65%. Incidence in heterosexual men, it estimates, fell by 55% in the same period, and in women by 22%.
This leads to an approximate total of new infections in the UK of about 1450 a year – around a third of the number of new diagnoses. Even if you take the current estimate that 7500 people were living with undiagnosed HIV in the UK in 2018, and add to it another 1450 new infections per year (a figure that is likely to decline further) – then, if the same 4453 are diagnosed each year, you reach a situation where there are more diagnoses than people remaining undiagnosed by 2022.
This won’t happen, of course, because diagnoses will fall as incidence does; because infections from people outside the UK will continue to be diagnosed; and because the remaining undiagnosed people will be harder to find. But new HIV stands to become relatively rare, as deaths due to AIDS are now.
Late diagnosis
The number of people diagnosed late – many of whom may be in that 'harder to find' category – has also fallen, from 3353 in 2009 to 1883 in 2018 ('late' is defined as with a CD4 count below 350). However, because diagnoses in the recently infected have also fallen, the proportion of people who are late-diagnosed has remained fairly steady at 43%, and is much higher among some groups such as black African heterosexual men (65%) and people aged over 50 (59%).
In the latter case, this is partly because people aged over 50 have simply on average had more time to live undiagnosed with HIV, but also because CD4 counts tend to fall faster in older people with untreated HIV. The proportion of people diagnosed over the age of 50 years has increased from 13% to 21% in the last decade.
One new, or newly published, fact in this year’s report is that many late-diagnosed people who were born abroad may actually have been diagnosed before their arrival in the UK but had probably not been taking treatment for some time. It’s estimated that 21% of new diagnoses, and 23% in gay and bisexual men, were in people who’d in fact been previously diagnosed abroad. This group accounts, it is estimated, for about 13% of the late-diagnosed.
Country of birth and ethnicity
In gay men, the general fall in HIV diagnoses was echoed in migrants from other countries, though not as strongly: the decline was 52% since 2014 in UK-born gay men and 36% in men born abroad. There is one exception: new diagnoses among gay men born in Latin America (where prevalence in gay men is very high) and the Caribbean have not followed this clear trend and have oscillated around 225 cases a year since 2014. This means they have risen as a proportion of the total, forming about one in seven diagnoses in gay men in 2018.
One question that is often asked about people born abroad is whether they acquired HIV in their home country or their new one. Here there have been approximately equal numbers of people who acquired HIV abroad and in the UK. However, and perhaps contrary to expectations, the number acquired in the UK has gone down, from about 600 in 2014 to 400 now, while the number acquired in the home country has stayed steady at about 600 a year. This may be due to lower UK incidence generally.
Diagnoses in African men and women have been in decline since the early 2000s, reflecting both lower immigration rates from high-prevalence countries and reduced prevalence in those countries. However the PHE report notes that for this group, diagnoses seem to have stopped going down – or at least, in 2018, there were slightly more of them than the previous year (643 in 2018 compared to 626 in 2017).
Regional differences
Diagnoses have fallen faster in London than elsewhere. Up till 2014 London accounted for about half of new diagnoses in gay men; this has now fallen to 39%. Among heterosexuals, London is no longer the single region with the most HIV diagnoses: there were 461 among people from the Midlands and east of England, followed by 416 in London. In addition, twice as many undiagnosed people are living outside London (approximately 4500) than within London (about 2100).
Positivity rate and where people test
As well as the incidence estimates derived from assays, the positivity rate of HIV tests are evidence of a steep decline in incidence.
In 2018, about 1.1 million people attending specialist health services tested for HIV, 6% more than in 2017, representing 58% of the 1.9 million eligible for a test. Of the 42% who were not tested, 45% declined a test. Heterosexual women (74% of those not tested or 24% of all female attendees) were most likely to decline a test compared with 12% of all heterosexual male attendees and 4% of gay men.
The percentage of those who tested positive has declined from 0.3% (one in 333) in 2014 to 0.13% (one in 770) in 2018. Positivity has gone down by about two-thirds in all high-prevalence groups. In gay men it has declined by 65%, from 2% in 2014 to 0.7% now; in African heterosexual men from 0.9% to 0.3%; and in African heterosexual women from 1.3% to 0.4%. This shows that positivity has declined less in low-prevalence groups such as white UK-born heterosexuals, though it has still declined. Positivity has not declined only among people diagnosed in primary care in low-prevalence areas of the UK, where the 0.2% positivity rate has remained steady.
Positivity has also declined, while the overall number of tests has increased, in other settings such as A&E departments (57,000 tests in 2018, 0.7% positive; hospital in-patients (120,000 tested, 0.42% positive); and prisons (58,000 tested, 1.2% positive).
There is also now significant uptake of self-sampling and self-testing in the UK. In 2018 138,000 people ordered a self-sampling kit from their local sexual health service website (eSHS); 24,000 from the national HIV self-sampling service at www.freetesting.hiv; and 56,000 bought a self-testing kit online or at a pharmacy. In the national self-sampling service overall ‘reactivity’ was 0.9% and strong reactivity suggesting a likely positive result (all reactive results need to be confirmed) was 0.5%. The eSHS local self-sampling services were mainly used by heterosexuals, and the national one by gay men, possibly because of how they were advertised.
90-90-90
It was announced in 2018 that based on 2017 figures the UK had reached the UNAIDS 90-90-90 target, meaning that 72.9% of all people with HIV were tested, on treatment and virally suppressed, and that London had exceeded the 95-95-95 target, or 85.7% of all people with HIV virally suppressed.
These trends continue, with 93% of people with HIV diagnosed in the UK in 2018, 97% of those on treatment and 97% of those virally suppressed (85.7% of all people with HIV virally suppressed). It is estimated that London has reached, or is very close to, the highly symbolic milestone of having over 90% of its HIV-positive population suppressed (95% diagnosed, 98% of those on treatment, 97% of those virally suppressed = 90.3%).
Of an estimated 13,100 people with detectable viral loads in the UK, 7,500 were undiagnosed, 2800 were not on treatment, and another 2800 were on treatment but not virally suppressed. In the latter case, some may have started treatment very recently.
PrEP
At the time the figures were collected in 2018, there were an estimated 12,000 people on PrEP in the UK via the English IMPACT trial or through programmes in Scotland, Wales and Northern Ireland. At least 5000 were buying PrEP online. The IMPACT trial is in the process of expanding and by the summer there should be 26,000 people accessing PrEP through that alone. PHE comments that as yet PrEP does not seem to have had an additional effect on reducing HIV incidence, but may well produce further falls by this time next year.
Mortality
Finally, the end result of all of this is to further reduce deaths from HIV. The PHE report finds that just 473 people with HIV died from all causes in the UK in 2018, with a median age of 55. It estimates that anything from 22% to 47% of these deaths could be due to AIDS, implying that 104 to 222 deaths could have been stopped, mainly by diagnosing people earlier, as deaths due to AIDS now overwhelmingly occur in the first year in people who are diagnosed late.
The report confirms something that has been reported elsewhere: people aged under 60, who are diagnosed in good time, with CD4 counts over 350, are now less likely to die than the general population in the same age group, probably due to better medical care. In 2018, the mortality rate among this group was 0.119% (one person in every 840 dying per year) compared with 0.161% in the general population (one person in 621 per year). In men with HIV, annual mortality was one death in 714 a year compared with one in 507 in the general population; in women it was one in 1369 versus one in 806. This is a remarkable change for a disease where, at the peak of AIDS, that annual figure was more like one in five.
O’Halloran C et al. HIV in the United Kingdom: towards zero HIV transmissions by 2030: 2019 Report. Public Health England, 2019.
Correction: This article was amended on 17 January 2020. Incidence figures were updated following a correction in PHE's own report.

