Low drug concentrations do not automatically lead to virologic rebound in people receiving injectable treatment with cabotegravir and rilpivirine, Swiss researchers found in a study of people receiving injections for up to six months. They say they are uncertain why some people experience virologic rebound when they have low drug levels while others remain virologically suppressed, as well as why drug levels seem to be so much lower in everyday clinical practice than in clinical trials.
The study found that levels of cabotegravir were lower than those reported in clinical trials. Approximately half of all cabotegravir measurements in the study were below the target level.
However, only three people out of 186 (1.6%) experienced virologic rebound during a median follow-up of 25 weeks for men and 16 weeks for women. The proportion of people experiencing virologic failure in this non-randomised study was the same as in clinical trials of injectable cabotegravir and rilpivirine.
The Swiss researchers measured plasma concentrations of cabotegravir and rilpivirine at each clinic visit and repeated these tests when drug concentrations were abnormally low. They collected 725 samples from 186 people with HIV receiving treatment in Switzerland with long-acting injectable cabotegravir and rilpivirine.
The study population was predominantly male (82%) and White (57%) and had a median age of 45 years.
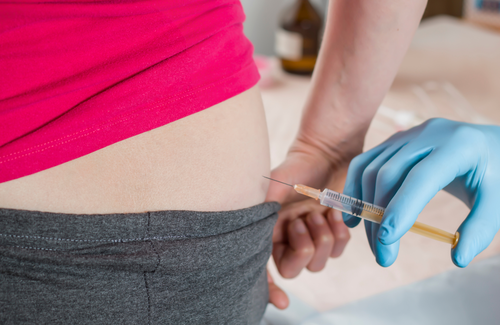
The median body mass index was 25.5 (just above the normal range) and 15% of the study population were living with obesity. Obesity may affect concentrations of injectable cabotegravir and rilpivirine because the needles normally used to inject the drugs are not long enough to penetrate through fat in the buttocks, and the drugs are less well absorbed through fat. Health care workers are recommended to use longer needles when injecting people with obesity. (A recent study found that injecting cabotegravir and rilpivirine into thigh muscle was acceptable to participants and achieved adequate drug concentrations in people with obesity).
Wherever possible, plasma samples were collected immediately prior to the next injection from week 8 of treatment so that drug concentrations could be measured at trough level (the lowest level before the next dose).
The study found that more than half of cabotegravir concentrations were below the pooled trough level observed in clinical trials (1120ng/ml). Thirty percent of cabotegravir levels were below the minimum concentration recommended in clinical practice (664ng/ml).
Similarly, more than half of rilpivirine concentrations were below the pooled trough level observed in clinical trials (32n/ml) and 7% of rilpivirine levels were below the minimum concentration recommended in clinical practice (12ng/ml).
For both drugs, concentrations were higher during the one-month oral dosing lead-in and far less often below the minimum concentrations.
A total of eight samples showed suboptimal cabotegravir concentrations (all in men) but no study participant who provided at least two plasma samples was found to have suboptimal concentrations in both samples. Three samples showed suboptimal rilpivirine concentrations (all in women) and in one person, two samples showed suboptimal rilpivirine concentrations. Cabotegravir trough levels were significantly lower (-35%) in men.
During the follow-up period, three people experienced virologic failure. In one case, virologic rebound occurred despite all drug concentrations being adequate. In this case, viral rebound to 17,000 copies/ml was detected at the time of the second injection visit. Viral load had resuppressed below 50 copies/ml at the third injection visit two months later but the participant was switched to bictegravir / tenofovir alafenamide / emtricitabine as a precaution.
In the two other cases of virologic rebound, drug concentrations were suboptimal at second or third injection visits. In one case, viral rebound did not occur until after injection visit 6, despite suboptimal cabotegravir concentrations at most previous injection visits.
Treatment with cabotegravir and rilpivirine was discontinued as a precaution in a further three people without virologic rebound.
A statistical analysis found that the only variable affecting drug levels was gender: cabotegravir trough levels were 35% lower in men, broadly consistent with two previous studies. Perhaps owing to the number of people switched from injectable treatment owing to low drug concentrations, the analysis found no significant relationship between low trough levels and detectable viral load.
Body weight did not affect levels of either drug. A recently published post-hoc analysis of phase 3 and 3a trials of injectable cabotegravir and rilpivirine also found that obesity alone was not associated with virologic rebound; people with obesity (body mass index of 30 or above) who experienced virologic failure in those studies had at least one other known risk factor for virologic rebound.
The Swiss HIV Cohort study investigators conclude that in a real-world cohort where participants may be delayed in returning for injections, cabotegravir trough levels were substantially lower than those observed in clinical trials. A small number of people displayed consistently suboptimal levels of one or both drugs but had no baseline characteristics known to predict virologic failure of injectable cabotegravir and rilpivirine treatment. And some people showed low drug concentrations on plasma samples taken one or two weeks after injection.
Although the findings are reassuring for the majority of people treated with cabotegravir, the “erratic pharmacokinetic profiles” seen in a minority of people require further investigation, the researchers say. It’s unclear if poor absorption at the injection site or rapid elimination of the drugs is responsible, and the investigators say that factors like vigorous physical exercise or massage could speed up absorption. Variations in the drug transporters in muscle tissue and subcutaneous fat could also affect absorption.
The researchers say that as the study was not a randomised trial, their results may have been somewhat affected by decisions made by doctors regarding changes in treatment and by variations in the time and frequency of sampling between participants. They are now carrying out a case-control study to investigate further what factors might influence concentration of injectable antiretrovirals.
Thoueille P et al. Real-world trough concentrations and effectiveness of long-acting cabotegravir and rilpivirine: a muticenter prospective observational study in Switzerland. Lancet Regional Health – Europe, 36: 100793, 2024 (open access).
Elliott E et al. Efficacy, safety and pharmacokinetics by BMI category in phase 3/3b cabotegravir + rilpivirine long-acting trials. Journal of Infectious Diseases, 22 December 2023 (open access).