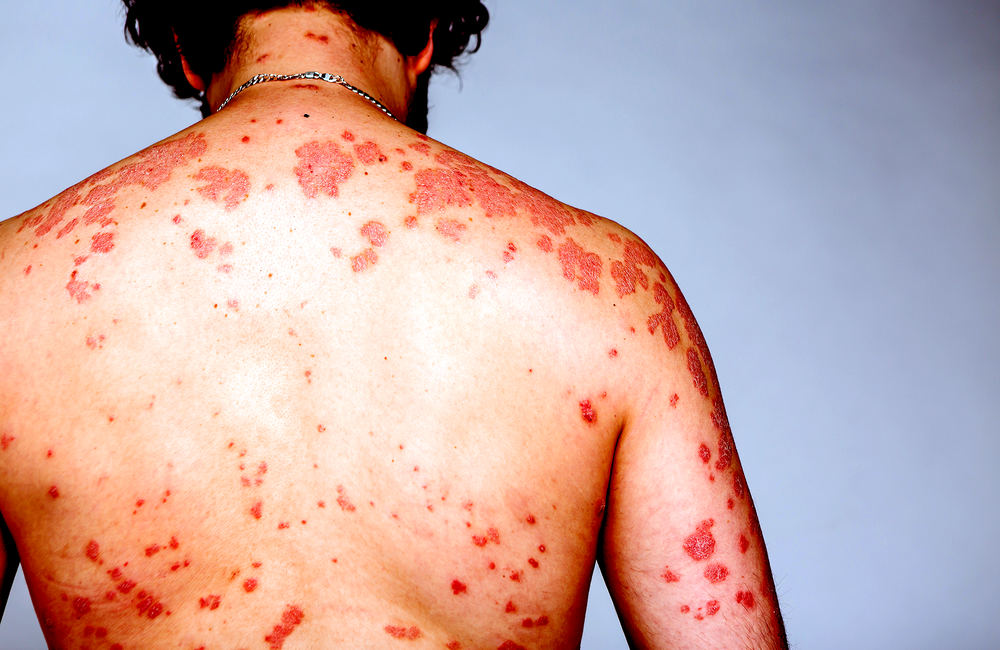
A Swiss study of people who were diagnosed during early HIV infection has found that a quarter of them presented or developed a wide variety of non-typical early symptoms of HIV infection, many of them serious and a few life-threatening. Gastrointestinal and neurological symptoms were particularly common in these manifestations of recent HIV infection. However, although these symptoms were often misdiagnosed at first, they did not, in this study at least, significantly delay the diagnosis of HIV infection.
The study
The Zurich Primary HIV Infection Study is an observational study that, since January 2002, has documented symptoms and laboratory results in any patient who is diagnosed with early HIV infection. This is defined as:
Acute HIV infection:
- In the presence of symptoms suggesting HIV infection, a negative or indeterminate HIV antibody test with a positive HIV p24 antigen and/or positive HIV RNA (viral load) test.
- In the absence of symptoms suggesting HIV infection, someone with a documented positive HIV antibody test in the last 90 days since a known date of exposure.
Recent HIV infection:
- Symptoms suggesting HIV infection and a positive HIV antibody test, but a negative incidence assay
- With no symptoms, someone with a documented positive HIV antibody test in the last 90-180 days since a known date of exposure.
The study was partly prospective, i.e. although the majority of people were diagnosed with HIV because they had symptoms, they were followed up for six months and any manifestation of early HIV infection also included.
There is no widely agreed definition of ‘typical’ acute HIV illness, so the researchers in this study had to use their own definition, taken from a search of the literature. They collected the 17 symptoms and two laboratory abnormalities most commonly found in early HIV infection. By far the most common symptom cited is fever, so the definition of typical acute HIV illness was either fever with one or more of the 18 other conditions on the list, or two or more of these conditions in the absence of fever.
Apart from fever, the top five typical symptoms in this study were elevated liver enzymes, malaise/fatigue, pharyngitis (sore throat), rash, and swollen lymph nodes. Weight loss, headache, muscle and joint pain and low blood platelet count have been in the top five in other studies.
Atypical early HIV illness/presentation was then categorised as:
- asymptomatic;
- an AIDS-defining opportunistic disease;
- a symptom or symptoms not on the typical list;
- other signs such as unusual laboratory abnormalities.
If patients had one of these, they were counted as ‘atypical’ even if this was accompanied by other symptoms that were on the typical list.
Results – asymptomatic patients
Out of 290 patients, 202 (70%) had typical HIV symptoms and 74 (25%) had atypical symptoms; only 14 individuals (5%), seven in the acute category and seven in the recent category, had no symptoms of early HIV infection.
This is not unexpected given that the most common reason to be in the study was presentation with suggestive symptoms. It is important to keep this in mind because it is lower than the usual estimates of the proportion of people who do not get any symptoms on infection, which ranges between 10% and 60% depending on how tightly the definition of acute HIV illness is drawn and how carefully it is looked for. This means that the atypical and often severe presentations of HIV infection documented in this study are less common than the 30% prevalence found here; they may actually occur in anything between 2% and 15% of acute HIV infections.
People who were asymptomatic were more likely to be women, younger, and have transmitted HIV drug resistance. They also had an average viral load at first test of about 130,000 copies/ml, whereas symptomatic patients (typical or not) had an average viral load of 4-5 million copies/ml.
Results – atypical symptoms
Most people (83%) with symptoms were in the acute category and, of these, 69 (28.5%) were classed as atypical. Of the 17% in the recent category, 40% of symptoms were classed as atypical.
People with atypical symptoms were more likely to have non-B HIV subtype, to be heterosexual, and to have no accompanying STIs (sexually transmitted infections). This is interesting both because the majority of studies of acute HIV infection have been conducted in people with HIV subtype B, and because some subtypes, such as D and A/E, seem to be more virulent than subtype B.
People with atypical symptoms were much more likely to be hospitalised because of them: 43% with atypical symptoms versus 11% with typical ones.
There was a long list of atypical HIV illnesses seen. The most common involved either the gut or the central nervous system, but symptoms also involved the eyes, the lungs, the kidneys and genitals, and the skin. There were constitutional symptoms such as severe weight loss and blood abnormalities such as pancytopenia (a general lack of blood cells).
AIDS-defining conditions were seen in 23% of people with atypical presentation. The most common AIDS-defining condition was severe oral or oesophageal candida (thrush), seen in 14% of untypical presentations. Most of the other AIDS-defining illnesses consisted of gut or liver infections with cytomegalovirus (CMV), one of the herpes virus family; there was also a single severe case of another herpes virus infection, shingles, a nerve inflammation initially diagnosed as Lyme disease, and a profound drop in platelet count, which was accompanied by a generalised HSV (herpes) infection. Two of the cases of oesophageal candida also involved neurological symptoms. One patient had severe diarrhoea and wasting with no cause present other than HIV.
The next most common symptom group was non-AIDS-defining gastrointestinal symptoms, seen in 14% of atypical presentations. Half of these consisted of tonsillitis. Three gastrointestinal cases required surgery: one involved a patient with severe gastric bleeding, an anal abscess and gall-bladder inflammation who turned out to have an HIV viral load of 100 million copies/ml. One patient presented with bacterial pneumonia, acute arthritis and acute kidney failure: another was originally diagnosed with appendicitis and underwent an exploratory operation; and one had a herpes-related inflammation of their entire digestive tract which required a hemicolectomy (part-removal of the colon).
Central nervous system symptoms were seen in 12% of atypical presentations. These ranged from transient facial paralysis in three patients through prolonged vertigo in one patient, to three patients who had acute psychiatric episodes (two of these were in the recent rather than acute category). Two patients had severe brain inflammation (encephalitis) and one meningitis; one had a stay in intensive care.
Other symptoms involved skin symptoms (9%) including dermatitis and cellulitis (soft-tissue infection); the lungs (6%, including three cases of pneumonia, aside from the case above); blood abnormalities (6%, including three cases of pancytopenia) and urogenital symptoms (3%, including two other patients with kidney failure, apart from the case above).
Although some patients were severely ill, no-one in the study died.
The mean CD4 count in all atypical presentations (including asymptomatic) was 421 cells/mm3. In the majority of cases of atypical illness, CD4 counts were above 350 cells/mm3 and in a number of cases, including some of the most severe ones, above 500 cells/mm3. Exactly 50% of patients had a viral load at presentation of over 100,000 copies/ml.
Diagnoses
Although 38 of the patients with atypical symptoms were correctly diagnosed with acute HIV, the remainder received a variety of diagnoses before being tested for HIV. These included: 17% with other viral diseases such as mononucleosis (Epstein-Barr virus); 6% with bacterial infections such as streptococcus; 3% (ten patients) with syphilis; gastroenteritis of unknown cause, and single diagnoses of a variety of diseases such as endocarditis, Lyme disease, appendicitis, diverticulitis, and lymphoma. Twelve per cent of patients were diagnosed by HIV testing with no other diagnosis recorded.
Despite this, in this study initial misdiagnosis did not appear to delay HIV diagnosis. Time to HIV diagnosis after first presentation was 29 days in people with typical symptoms and 32 days with atypical symptoms. People attending an STI clinic were diagnosed earlier (21 days after presentation) than people attending hospital A&E (32 days) or GPs (33 days).
The researchers note that there is hardly a single individual symptom in the list of typical HIV symptoms that is not presented as often, or nearly as often, in patients who turn out to be HIV negative. It is the combination of symptoms that counts alongside the likelihood of recent exposure to HIV, and this study extends our knowledge of how it may present.
This study is a reminder that HIV can present in a wide variety of different ways and can cause a significant acute illness, underlining the importance of testing after any suspected exposure or post-exposure prophylaxis (PEP) after a really recent one.
Braun DL et al. Frequency and spectrum of unexpected clinical manifestions of primary HIV-1 infection. Clinical Infectious Diseases, early online publication: doi: 10.1093/cid/civ398. 2015.

