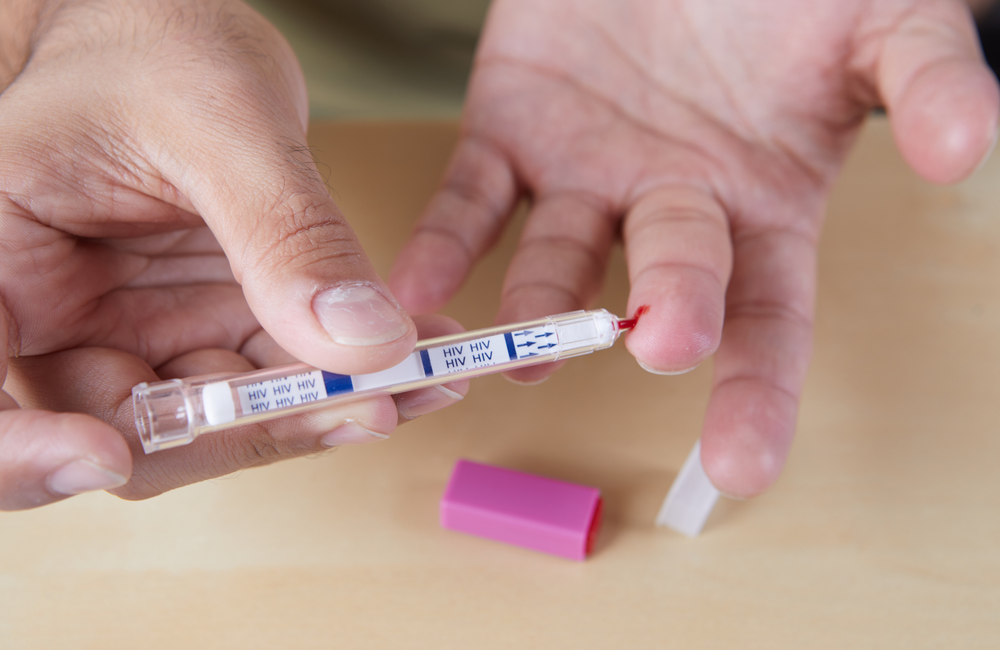
Trans people are more likely to test for HIV, and test more often, when provided with self-tests, according to research from England and Wales published in EClinicalMedicine.
Ninety-five per cent of trans participants who received a self-test tested for HIV compared to 26% of those who did not, while those who were offered repeat tests reported three times the rate of HIV testing compared to those who received a one-off test.
The mixed-methods study found that self-testing is highly acceptable to trans people, with reported benefits including increased autonomy, privacy, and convenience, and avoidance of healthcare services perceived to be discriminatory and that increase gender dysphoria.
Trans men made up the majority of participants in a relatively small sample. While this weights the findings towards trans men, it also increases knowledge and understanding of a group rarely included in HIV research.
“As trans people face barriers to HIV services and poor HIV health outcomes, services delivering HIV self-testing to trans people in the UK should be implemented to support this group,” the authors write. “Tailored and targeted HIV self-testing interventions are likely to be acceptable and feasible to deliver.”
Trans people face barriers to HIV testing not experienced by other groups, and recent research indicates that many trans people in the UK have never tested for HIV. HIV self-testing is a relatively new method of testing for HIV, whereby people test themselves using a rapid diagnostic test. HIV self-testing has been reported to reduce barriers to testing and has been recommended in World Health Organization guidelines since 2016. However, concerns persist that HIV self-testing may reduce rates of STI testing and create unintended harms, such as coerced testing and intimate partner violence.
Prior to this study no European evidence regarding trans people and HIV self-testing existed. Keen to rectify this situation, a research team led by Dr T Charles Witzel of the London School of Hygiene and Tropical Medicine conducted a study to determine the impact and acceptability of HIV self-testing among trans people in England and Wales.
They used data from the SELPHI trial, a randomised controlled trial evaluating HIV self-testing with over 10,000 cis men and 118 trans men and trans women, all of whom have sex with men. Their study focused on the 118 trans participants.
SELPHI participants were recruited online via social media and apps (Facebook, Grindr, Scruff and Growlr), and were initially randomised into two groups. The first group received an HIV self-test, while the other group were provided with a link to standard testing services. A proportion of those who received a self-test were randomised a second time and offered either repeat self-testing (an additional self-test every three months) or standard testing services. All participants were followed up for two years, and 20 trans participants (seven women, 12 men and one non-binary person) also took part in in-depth interviews with a peer researcher to discuss their experiences of the trial and HIV testing more generally.
Of the 118 trans participants in the trial, 94 (80%) were trans men. The authors highlight this as a limitation, as it meant they were unable to provide analyses for trans women specifically, as well as skewing the results towards the experiences of trans men. They also note that they did not recruit non-binary people, citing research with this group as a critical future priority.
The majority of the participants were White (79%) and born in the UK (79%). The median age was 29, and 37% were university-educated. Around a third (31%) had never previously tested for HIV, indicating substantial unmet testing need. Baseline characteristics did not differ significantly between the groups randomised in the trial.
None of the trans participants tested positive for HIV during the study. Ninety-five per cent of the self-testing group tested for HIV compared to 26% who received standard care, making the self-testing group 3.43 times more likely to test for HIV (95% CI 1.72, 6.81, p < 0.001).
During the two-year follow-up period, those who received repeat tests reported 3.66 times the rate of HIV testing compared to those who received a one-off self-test (95%CI 1.86, 8.01; p < 0.0001).
"Reported benefits including increased autonomy, privacy, and convenience, and avoidance of healthcare services perceived to be discriminatory."
These findings were reflected in the sub-analyses focused on trans men, who were 3.32 times more likely to test if they received a self-test compared to those who didn’t, and 2.98 times more likely to test if they received repeat self-tests rather than a one-off test.
HIV self-testing was highly acceptable for the trans men and women who received self-tests: 97% found the instructions easy to understand, 97% found the test simple to use and 100% reported a good overall experience.
Importantly, self-testing did not negatively impact on STI testing rates, although these were generally low among all trans participants. No participants in either group reported negative impacts on wellbeing or relationships, and none reported feeling pressured or persuaded to test when they did not want to. However, two participants in the repeat testing group (one trans man and one trans woman) reported pressuring or persuading someone else to test when they did not want to.
The findings from the in-depth interviews suggested that the primary reason for using an HIV self-test among trans people was to avoid having to access clinical HIV testing services which they find inaccessible and inappropriate to their needs.
Interviewees reported staff working in sexual health clinics frequently misgendering them, treating them as a burden, erasing their sexual orientation and/or gender identity and disregarding their perceptions of risk. They reported that services (even those billed as LGBT-inclusive) are usually not set up in a way that recognises their unique needs as trans patients, which can contribute to feelings of gender dysphoria. In contrast, services designed for and by trans people were highly valued.
One trans woman said:
“They don’t have in their system that I am a trans woman. So they always think that I’m a [cis] woman. Because I don’t have vagina yet, so they always give me the test for vagina. So I have to go always to the reception desk to tell them, sorry, but I don’t have vagina yet.”
Interviewees also cited the increased autonomy, privacy and convenience as advantages of self-testing.
Overall, the study highlights that self-testing is an acceptable testing intervention for trans people which has the potential to dramatically increase testing uptake and frequency among this key population. Modes of delivery should be further explored, with the authors suggesting peer self-testing initiatives and self-testing delivered alongside services providing gender-affirming care in order to widen engagement with trans people. It is also crucial that sexual health services remodel clinical processes and provide staff training to ensure their services are trans-inclusive. This is especially important since many of these services provide HIV treatment and care as well as testing.
Witzel TC et al. Impact and acceptability of HIV self-testing for trans men and trans women: A mixed-methods subgroup analysis of the SELPHI randomised controlled trial and process evaluation in England and Wales, EClinicalMedicine, 32: 100700, February 2021 (open access).

