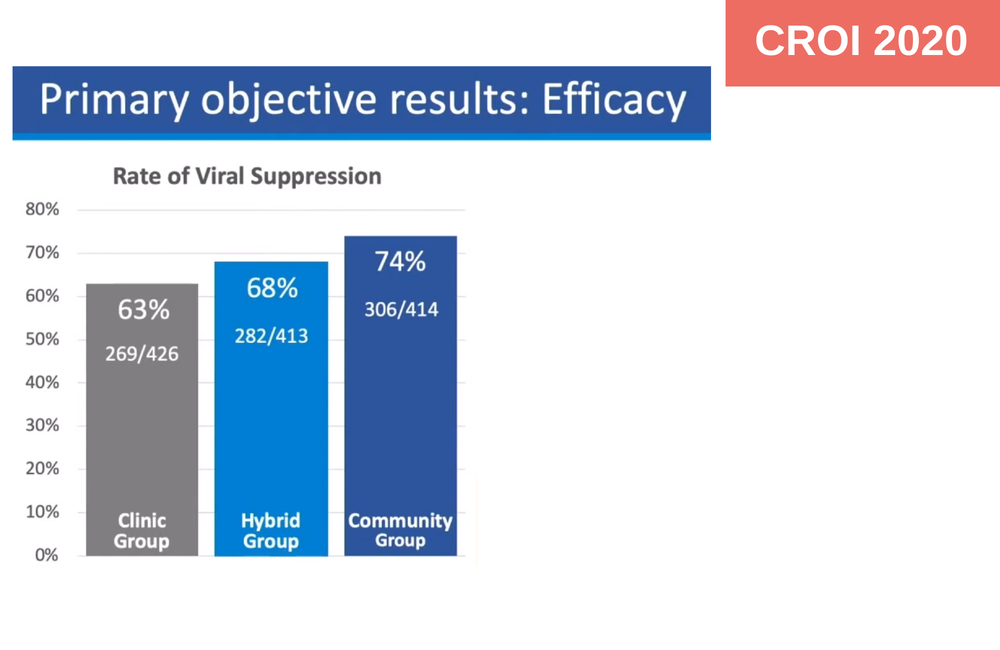
Starting antiretroviral treatment on the day of diagnosis in a community setting and picking up medication from a mobile van resulted in superior rates of viral suppression, especially in men in South Africa, the randomised DO ART trial has found.
The findings were presented at the 2020 Conference on Retroviruses and Opportunistic Infections, which is taking place online this year in response to the risk of coronavirus transmission.
Men living with HIV in sub-Saharan Africa are less likely to be diagnosed, less likely to be in care and in some settings, less likely to be on antiretroviral treatment.
Improving diagnosis and engagement in care among men living with HIV is essential to achieve the goals of 90% diagnosed, 90% on treatment and 90% virally suppressed that guide international efforts to reduce HIV transmission and mortality.
But engaging men in care has proved challenging in many countries. Work commitments, stigma, and clinical services geared towards the needs of women and children are often cited by men as obstacles to care.
Even community-based testing and treatment that involves door-to-door visits has run into a consistent challenge: men are less likely to be at home when health workers call.
This is a critical challenge, as shifting testing and treatment into the community is a cornerstone of efforts to expand treatment access without overwhelming health facilities.
To test the impact of several models of community-based testing and treatment, Dr Ruanne Barnabas of University of Washington and colleagues in South Africa and Uganda designed the Delivery Optimization for Antiretroviral Therapy (DO ART) study.
The study compared three approaches to testing and treatment in high HIV prevalence communities in Uganda and South Africa:
- Clinic-based care (standard-of-care arm).
- Community-based HIV testing and ART start (the community arm). Community-based treatment was initiated by nurses, with quarterly monitoring and medication refills through mobile vans.
- ART started at a clinic, with medication refills through mobile vans in the community (hybrid arm).
The primary outcome of the study was the proportion of people living with HIV who were virally suppressed (< 20 copies/ml) after one year. The secondary objectives of the study were to evaluate the impact of community-based ART delivery specifically in South Africa and among South African men.
Participants were recruited to the study after testing HIV positive in the community. The study randomised 1531 people living with HIV who were not on treatment and who had detectable viral loads. Men made up half the study population (51%), participants had a high median CD4 cell count (450 cells/mm3) and the majority were aged 30-49 years (55%).
Viral suppression was superior after 12 months in participants randomised to community care and dispensing when compared to clinic-based care; 74% were virally suppressed in the community group compared to 63% in the clinic group (relative risk 1.18, 95% CI .07-1.28, p =0.00053). When the analysis was confined to South African participants, community-based dispensing and care also resulted in superior outcomes (72% vs 60%, RR 1.26, 95% CI 1.04-1.51, p = 0.0038).
The hybrid model of care was non-inferior to clinic-based care (68% vs 63%, RR 1.08, 95% CI 0.98-1.19, p = 0.0045) in the entire study population and in South African participants (67% vs 60%, RR 1.12, 95% CI 1.00-1.15, p = 0.0026).
When the two models of community delivery were analysed in South African men, both were found to be superior to clinic-based care (community vs clinic, 72% vs 51%, RR 1.39, 95% CI 1.17-1.66, p < 0.0001; hybrid vs clinic, 65% vs 51%, RR 1.26, 95% CI 1.04-1.51, p = 0.016).
Across the entire study population, community- or hybrid ART delivery eliminated gender differences in viral response (65% in men and 69% in women in the hybrid group, 72% and 73% in the community group).
Barnabas RV et al. Community ART increases viral suppression and eliminates disparities for African men. Conference on Retroviruses and Opportunistic Infections, abstract 49LB, March 2020.
View the abstract on the conference website.
Watch the webcast on the conference website.
Update: Following the conference presentation, this study was published in a peer-reviewed journal:
Barnabas RV et al. Community-based antiretroviral therapy versus standard clinic-based services for HIV in South Africa and Uganda (DO ART): a randomised trial. The Lancet Global Health, 8: e1305-e1315, October 2020.
