Three-quarters of Australian gay and bisexual men who report unprotected anal intercourse with casual male partners say that they “often” or “always” employ some sort of risk reduction strategy with those partners. Many attempt to select partners who they believe have the same HIV status as themselves (serosorting); a significant proportion use condoms most but not all of the time; and smaller numbers practice ‘strategic positioning’ or withdrawal before ejaculation.
The study shows that a simple, black and white division of gay men into low risk ‘condom users’ and high risk ‘men who don’t use condoms’ is misleading. However that is sometimes the impression given by behavioural surveys.
Martin Holt of the University of New South Wales presented the data to the 20th International AIDS Conference in Melbourne yesterday. It is derived from an analysis of the responses to two large-scale, cross-sectional community surveys of Australian gay and bisexual men in 2011 and 2012. A total of 15,615 completed the surveys.
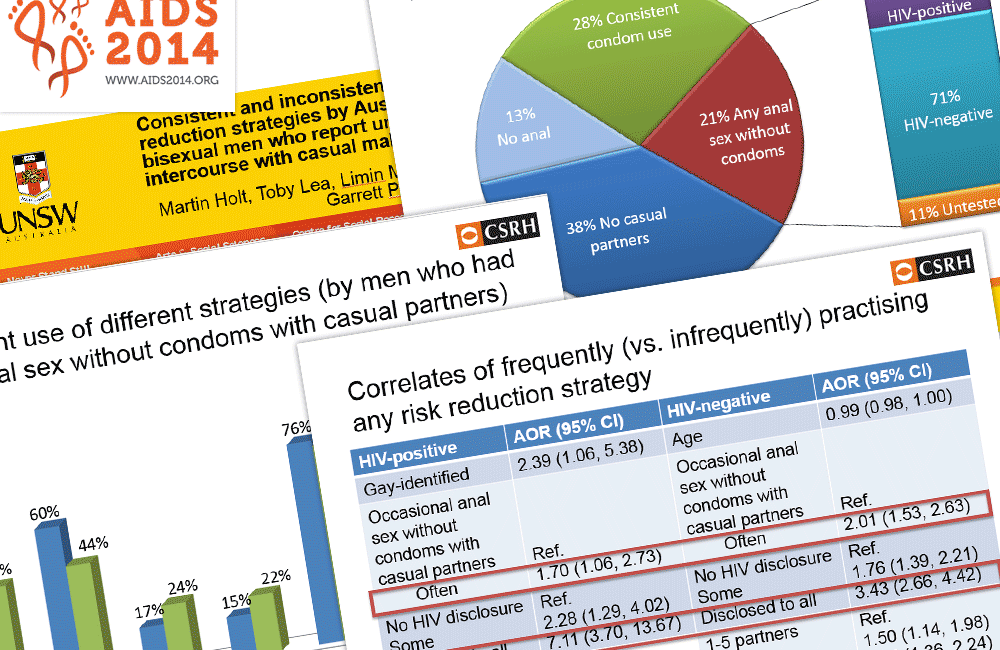
Overall, 38% had no casual partners (and are not included in this analysis, even if they did not use condoms with their partner), 28% always used condoms with casual partners and 13% had no anal sex.
That leaves 21% who reported anal sex without a condom with at least one casual partner in the previous year – this group was the focus of the study.
Moreover as risk reduction strategies differ according to HIV status, the analysis made comparisons between the 2339 men who had tested HIV negative and the 603 men who were diagnosed with HIV. The small number of men who had never tested for HIV were excluded from the analysis.
Holt was interested in risk-reduction strategies the men used “often” or “always” with casual partners, including:
- Condom use.
- Serosorting (having a partner perceived to have the same HIV status) when having anal sex without condoms.
- Strategic positioning when having anal sex without condoms – in other words, the HIV-positive partner taking the receptive position (bottom).
- Withdrawal before ejaculation during anal sex without condoms.
HIV-positive men who didn’t consistently used condoms with casual partners reported serosorting (60%), condoms (22%), strategic positioning (17%) and withdrawal (15%).
HIV-negative men were more likely to report using condoms most of the time, but serosorting was still the most widely reported tactic (44%), followed by condoms (41%), strategic positioning (24%) and withdrawal (22%).
Three-quarters of men reported using more than one strategy; the strategies most commonly combined were serosorting and condom use.
There was a very strong association between using these strategies and disclosing HIV status to sexual partners. This was the case both for HIV-positive and HIV-negative men.
For example, for HIV-negative men, those who disclosed to some sexual partners were almost twice as likely to practice a strategy as those who did not (odds ratio 1.76, 95% confidence interval 1.39 – 2.21) and those who disclosed to all partners were three times as likely to have a strategy (odds ratio 3.43, 95% confidence interval 2.66 – 4.42).
HIV-positive men who always disclosed were seven times more likely to use these strategies (7.11, 95% CI 3.70 – 13.67).
HIV-negative men who had a regular partner were less likely to practice any risk reduction strategy if their partner was untested or HIV negative.
Martin Holt concluded that interventions should aim to improve the consistency with which gay and bisexual men employ risk reduction strategies. Men should be encouraged to disclose their HIV status, to make effective agreements with their regular partners about casual sex and to choose the best strategy in different scenarios. Alternative approaches such as PrEP are likely to be appropriate for those men unable or unwilling to use existing strategies.
Holt M et al. Consistent and inconsistent use of HIV risk reduction strategies by Australian gay and bisexual men who report unprotected anal intercourse with casual male partners. 20th International AIDS Conference, Melbourne, 2014, abstract THAD0101.
