The new Tibotec non-nucleoside reverse transcriptase inhibitor rilpivirine (TMC278) is just as effective as efavirenz in suppressing viral load, but less likely to cause side-effects, delegates heard today at the Eighteenth International AIDS Conference in Vienna.
Rilpivirine is likely to be submitted for licensing in the United States very quickly, and will also be combined in a once-daily tablet with Gilead’s drugs tenofovir and emtricitabine.
Dr Cal Cohen of Community Research Initiative New England, Boston, presented a pooled analysis of two international phase III studies, ECHO and THRIVE, which randomised nearly 1400 people with HIV with no previous experience of treatment to receive either rilpivirine 25mg once daily or efavirenz 600mg once daily in combination with two nucleoside analogues.
The ECHO study randomised 690 patients, and all received a nucleoside analogue backbone of tenofovir and emtricitabine. THRIVE randomised 678 patients, and the nucleoside backbone was chosen by the patient’s doctor. Around 60% of participants received tenofovir/FTC and 30% received AZT/3TC and 10% received abacavir/3TC.
Participants had relatively low CD4 counts (a median of around 250), and high viral load (median 5 log, or 100,000 copies/ml).
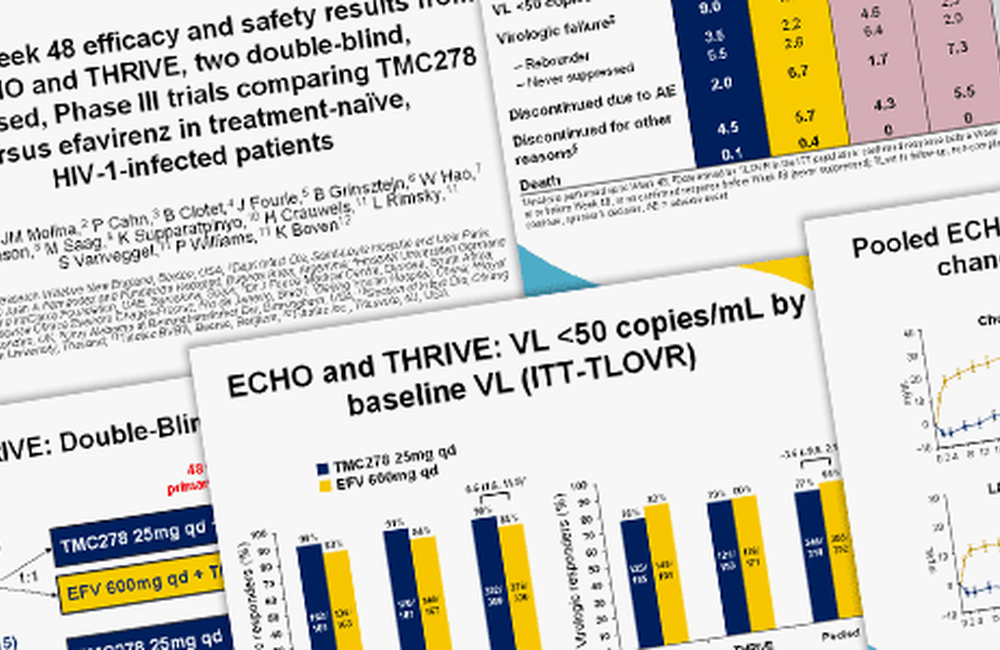
After 48 weeks of treatment the proportions with viral load below 50 copies/ml were almost identical (84.3% in the rilpivirine arm, 82.3% in the efavirenz arm), a non –inferior outcome.
Virological failures, defined as two viral loads above 50 copies/ml even if viral load was suppressed again at week 48) were more frequent in the rilpivirine arm (9% vs 4.8%), and this difference was largely driven by the higher failure rate in the ECHO study (11% vs 4.4%), in which patients received a variety of nucleoside backbones. The statistical significance of this difference was not reported.
Commenting on this difference, Cal Cohen said that there was no difference in response rates according to nucleoside backbone, nor by baseline viral load
In patients who experienced virological failure, different primary resistance mutations occurred; while efavirenz-treated patients developed the K103N mutation, rilpivirine-treated patients tended to develop the E138K mutation that causes resistance to the second-line NNRTI etravirine. Half of those who failed rilpivirine developed resistance to the drug, and of them, 90% were resistant to etravirine too.
Discontinuations due to adverse events were significantly more common in the efavirenz group (6.7% vs 2%) (p=0.005), and central nervous system adverse events (such as dizziness and abnormal dreams were significantly more common in the efvairenz, occurring two to three times more often in these patients (overall frequency 38% vs 17%). Rash was also more common in efavirenz-treated patients.
Further information
View abstracts and slides from this session on the official conference website.
Cohen C et al. Pooled week 48 efficacy and safety results from ECHO and THRIVE, two double-blind, randomised phase III trials comparing TMC278 versus efavirenz in treatment-naïve HIV-1-infected patients. Eighteenth International AIDS Conference, Vienna, abstract THLBB206, 2010.
