Too few women and black people included in HIV research
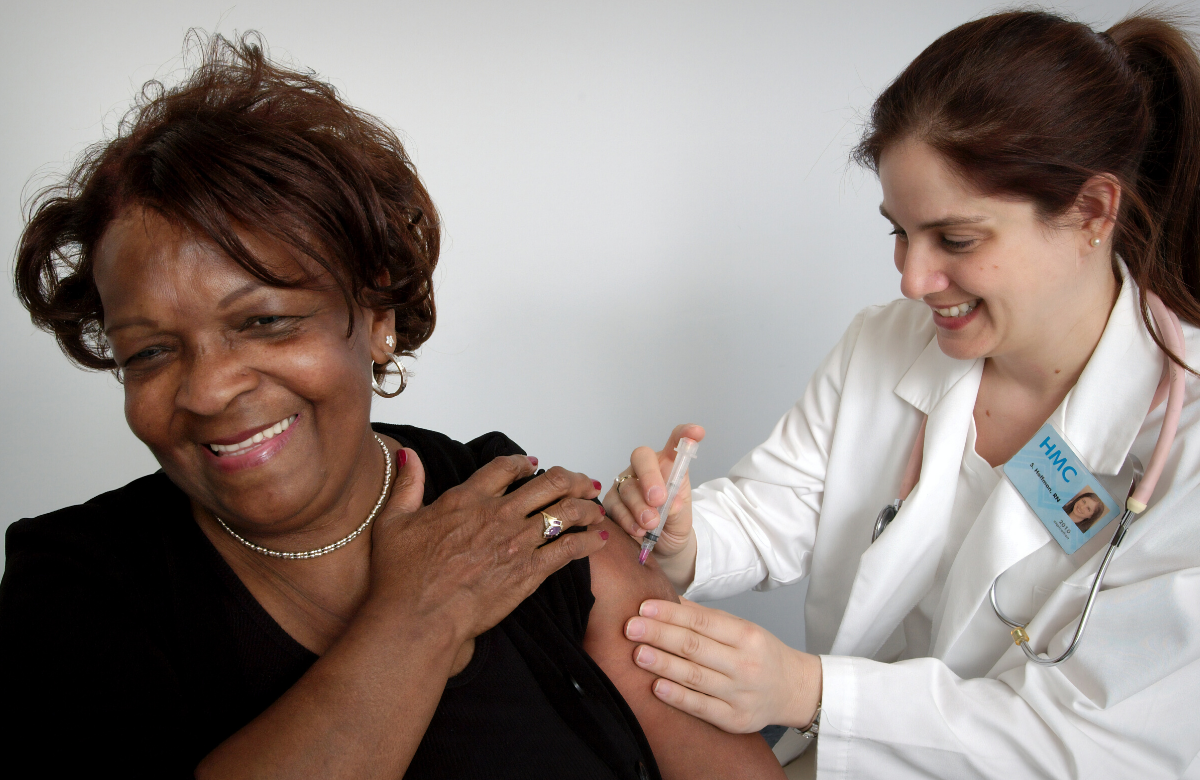
Recruitment to clinical trials for new anti-HIV medications is not representative of the global HIV epidemic, researchers say. These studies are overwhelmingly conducted in richer countries and white men are massively over-recruited.
This matters because differences in the ways in which drugs are absorbed, distributed and eliminated by the body could be missed. This could result in side effects not being noticed until medications are in wider use.
This appears to have happened with weight gain in people starting modern anti-HIV medications. The problem affects women and black people in particular and it wasn’t picked up by the initial studies.
In 24 studies that led to the regulatory approval of four different medications, 7% of participants were black women and 17% were black men. Forty-two per cent of the global population of people living with HIV are black women and 30% are black men.
Half of all study participants were white men, although they make up 6% of people living with HIV. Even in the high-income countries where most studies are done, less than a third of people living with HIV are white men.
The researchers say that researchers should aim for at least 50% female and 50% non-white participants to provide enough data on drug safety.
Access to the NHS for migrants

Understanding which NHS services are freely available for people born outside of the UK can be confusing. This page looks at the groups of people who are entitled to free NHS health care, the types of treatment that are free, health care that you may have to pay for, and information sharing between the NHS and Home Office.
Latest coronavirus update

Doctors in New York and Germany have published details of small groups of people living with HIV who were treated for COVID-19. The doctors’ cautious conclusions are that people living with HIV are not at higher risk of death or severe illness, but the New York study did flag up a possible concern about bacterial pneumonia.
The German study included 33 people living with HIV diagnosed with COVID-19. Most were men who were doing well on HIV treatment, with an average age of 48, but 20 had other health problems such as high blood pressure, chronic obstructive pulmonary disease (COPD) or diabetes. Twenty-five of the cases were classed as mild, 29 patients have recovered and three have died.
In New York, the 21 patients were a little older and not always doing so well on HIV treatment – half had CD4 counts below 300. Comparing coronavirus patients who had HIV and those who did not, it appeared that those with HIV were more likely to go into intensive care and to need a ventilator, although the numbers are small and we can’t draw any firm conclusions.
Also, three people with HIV and one HIV-negative person developed bacterial pneumonia (in addition to pneumonia caused by the coronavirus). As all four died, the researchers say that doctors need to be particularly vigilant about bacterial pneumonia in people with HIV who have COVID-19.
Taking this new information into account, the British HIV Association (BHIVA) and the European AIDS Clinical Society have updated their statement on the risk of COVID-19 for people living with HIV. “So far there is no clear evidence for a higher COVID-19 infection rate or different disease course in people with HIV than in HIV-negative people,” they say. However, they add that in some studies, HIV-positive people who have needed to go to hospital because of the coronavirus have tended to be younger than other coronavirus patients.
They also point to the factors that are associated with an increased risk of severe coronavirus illness – being older, being a man and having certain chronic medical problems such as cardiovascular disease, chronic lung disease, obesity and diabetes. Many people living with HIV do have these risk factors so have reason to be vigilant.
Wanted: new writers for aidsmap

We’re looking to recruit people to write for aidsmap as part of our Emerging Voices programme. Emerging Voices gives new writers the opportunity to gain experience and develop their skills and in a professional and supportive environment. Applications close on 14 June.
Depression and cognitive impairment

Memory, attention span, speed of processing information, ability to plan and organise daily life, and fluency in using language are all aspects of cognitive function. A new study in people with HIV shows that depression has an impact on cognitive function.
The study involved 448 Americans living with HIV who were assessed once a year, for five years on average – the long-term follow-up is a strength of this study. The one-in-six participants who had the highest burden of depression when they joined the study had steeper declines in cognitive function in the following years. Particularly affected were recall and memory; planning, organising a task, problem solving and decision making; and language abilities.
In the short term, the researchers also found that cognitive function was poorer on days when people had symptoms of depression, even mild depression. There were particular problems with fine motor skills (dexterity and co-ordination used for handwriting or using small objects) and the speed with which people could process information.
Weight gain and HIV treatment

What causes weight gain after starting treatment? Who is most likely to gain weight? What drugs are associated with weight gain? Find out in our new research briefing.
Injectable PrEP
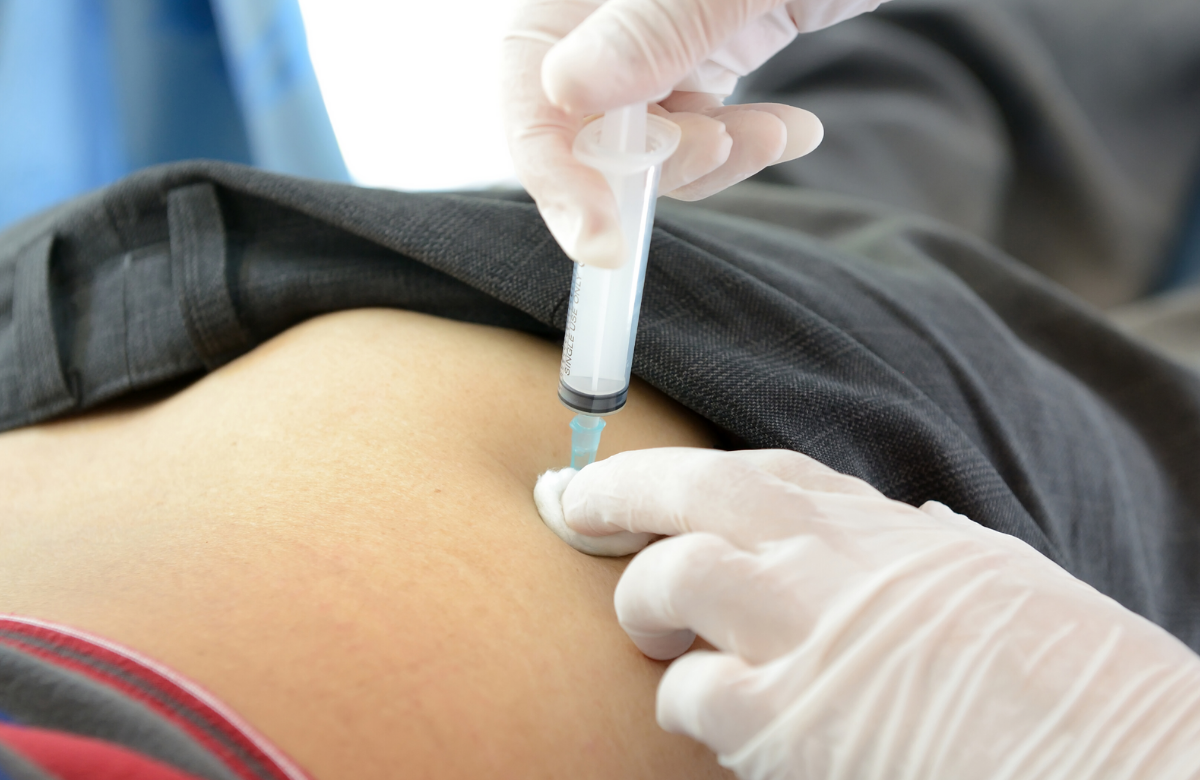
The biggest news for some time about PrEP is the positive result of a study into injectable PrEP – an injection into the buttocks of the drug cabotegravir, once every two months.
For the moment, only the briefest and most preliminary of results have been released. In the trial, 4600 gay and bisexual men and transgender women either got the injections or the usual tenofovir/emtricitabine PrEP pill. Twelve study participants receiving the cabotegravir infections and 38 taking the pills became infected with HIV. We need to see more details, but the difference could be due to problems some study participants had with taking the pills every day.
A separate study testing the injections with women in African countries is ongoing.
Studies have already shown injectable HIV treatment (of the drugs cabotegravir and rilpivirine) to be effective. This combination is likely to be approved by medicine regulators soon, although injections will probably need to be once a month until there is more evidence on longer schedules.
Lots of people will welcome injectable HIV treatment and PrEP, but many potential users have complex and ambivalent feelings about switching to this new method, French researchers have found.
aidsmapCHAT

If you missed our aidsmapCHAT broadcasts, you can catch up with them on our website and social media. aidsmapCHAT was our series of live, weekly discussions on news and updates on COVID-19 from around the world for people living with HIV.
Editors’ picks from other sources
Larry Kramer, playwright and outspoken AIDS activist, dies at 84 | New York Times
He worked hard to shock the country into dealing with AIDS as a public health emergency. But his confrontational approach could sometimes overshadow his achievements.
South Africa: Almost 11,000 HIV-positive patients in Gauteng have skipped ARV collection during lockdown | TimesLIVE
“Since the lockdown the average percentage reduction in medicine collections for TB is 1.4% and 19.6% for HIV,” read a statement from the Gauteng health department.
Will COVID-19 make modernising HIV criminal laws harder? | TheBody
TheBody asked several HIV criminal law modernisation advocates about what the novel coronavirus pandemic could mean for HIV laws, and vice versa. Most were cautiously optimistic that their years of educating lawmakers and law enforcement could make it easier to prevent new, draconian laws around criminal transmission of the COVID-19 virus.
What to do if you're HIV positive and are admitted to hospital with COVID-19 – advice from the British HIV Association (BHIVA) | BHIVA
In response to questions from the HIV community on what to expect, and what to do, if you are an HIV-positive person who is admitted to hospital with COVID-19, the British HIV Association (BHIVA) has given the following advice to answer the main points that have been raised.
COVID-19 crisis raises hopes of end to UK transmission of HIV | The Guardian
Sexual health experts see in lockdown restrictions a ‘once-in-a-lifetime’ chance. “If we can now find the remaining people with HIV through testing and put them on treatment,” says Dr Alan McOwan, “we could remove anyone who is infectious from the population with long-lasting effects. We won’t get this two-month window of no sex again.”
