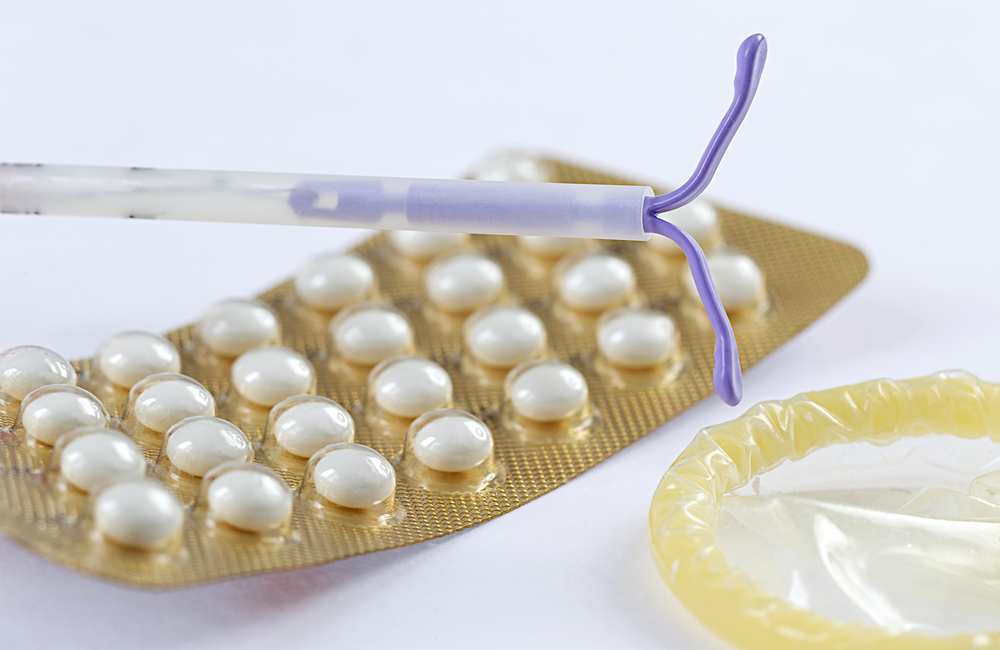
Key points
- Your choice of contraception will depend on your situation and preferences.
- There are possible interactions between some hormonal contraceptives and some anti-HIV drugs.
- Your HIV treatment needs to be taken into account when choosing a contraceptive.
Contraception is a way to prevent pregnancy. There are some particular issues for people living with HIV to take into account when choosing a contraceptive method.
Becoming a parent of a healthy, HIV-negative child is a realistic option for many people with HIV. However, you may want to plan when pregnancy happens, or prevent pregnancy from ever happening.
Choosing a contraceptive method
Your choice of contraception will depend in part on your situation and preferences. Some of the things you might want to think about are:
- Whether a contraceptive is compatible with your HIV treatment.
- How well a contraceptive method will suit your lifestyle.
- How often you have to use a contraceptive.
- If, and how soon, you want to become pregnant in the future.
- How to protect yourself and your partner from infections.
- The possible side-effects of different contraceptives.
- Your partner’s preferences.
There is plenty of information on the Brook, FPA and NHS Choices websites, but bear in mind these sites often don’t have information about HIV-specific issues.
Hormonal contraception and anti-HIV drugs
Some types of contraception contain one or more hormones. The extra hormones stop ovulation, so your body does not release an egg for fertilisation. They also thicken the mucus around the cervix, making it difficult for sperm to get into the womb.
They include:
- the combined pill
- the progestogen-only pill
- the patch
- the vaginal ring
- contraceptive Injections (Depo-Provera or Sayana Press)
- the implant
- the intrauterine system (IUS, Mirena or Jaydess).
Several anti-HIV drugs interfere with how hormonal contraceptives work, and contraceptives may not be as effective as usual. If there are drug interactions, you can be supported to change your HIV treatment so that you can use your preferred contraceptive method.
The interaction can occur because both the anti-HIV drug and the contraceptive are processed in the liver by the same enzymes, so the contraceptive is processed faster than usual. As a result, levels of the contraceptive hormones may be too low to always prevent a pregnancy. The anti-HIV drugs will continue to be effective and work well.
These hormonal contraceptives may be less effective, depending on the HIV treatment you are taking:
- the combined pill
- the progestogen-only pill, also known as the mini-pill
- patches – a small beige patch applied to the skin like a sticky plaster that is changed once a week
- implants – a small flexible rod that is inserted under the skin on the upper arm, and works for up to three years
- vaginal rings – a small flexible ring that is inserted in the vagina for three weeks of the month.
Some hormonal contraceptives are not affected by any anti-HIV drugs (see Long-acting reversible contraceptives below). And not all anti-HIV drugs interfere with contraceptives.
Some other medications can interact with hormonal contraceptives, including some antibiotics and drugs used to treat epilepsy. Getting advice on possible drug interactions from your healthcare team is important. Let them know about any other drugs you are taking, including any contraceptives.
Long-acting reversible contraceptives
Long-acting reversible contraceptives are very effective birth control methods. Many people like these long-acting methods of contraception as they are the most reliable methods, offer the convenience of not having to take daily tablets, and can also be more discreet. Once fitted or administered, they will work for several months to ten years, so you don’t need to think about using them every day or every time you have sex.
The Intrauterine Device (IUD), Intrauterine system (IUS) and injectable contraceptives are not affected by HIV treatment. Some anti-HIV drugs may interact with contraceptive implants. Nonetheless, real world evidence shows that the implant is still highly effective in people living with HIV.
Intrauterine Device (IUD) and Intrauterine system (IUS)
The IUD is a small, T-shaped device made from plastic and copper that fits inside the womb (uterus). It is sometimes called a coil. It releases copper into the body, causing changes that prevent sperm from fertilising eggs. Once fitted, it works for five to ten years.
The Mirena IUS is a small plastic device also fitted in the womb, which contains hormones. Periods usually become lighter, sometimes stopping them altogether. Some people use it to reduce heavy, painful periods. Once it’s fitted, it works for five years.
For both the IUD and IUS, you will be offered a sexual health screen, and any sexually transmitted infections (STI) will be treated before a doctor or nurse fits the coil. They can be painful to fit and can be easily removed if it doesn’t suit you. Once removed, your fertility will return to normal immediately.
Contraceptive injections
Contraceptive injections contain the hormone progesterone and work by preventing ovulation. The most common type of contraceptive injection is called Depo-Provera (commonly known as the Depo). Sayana Press is another type of contraceptive injection. Each injection lasts for 13 weeks.
Contraceptive injections may reduce heavy periods and help with premenstrual symptoms. Most often, periods will stop completely, however, some people experience irregular or heavy periods or periods that last longer.
"In the UK, contraception is available free, provided by the National Health Service (NHS). "
Contraceptive injections can sometimes lead to a small loss of bone mineral density or thinning of the bones. Usually this isn’t a problem, but some anti-HIV drugs, HIV itself, and age can all affect bone mineral density. Depo-Provera has been shown to worsen bone loss from the anti-HIV drug tenofovir. It’s important to discuss this with your healthcare team when selecting a contraceptive method.
Unlike the other long-acting options, a contraceptive injection cannot be removed once it is injected so it will stay in your body for 13 weeks. After your last injection, there may be a delay of up to one year before your fertility returns to normal.
You can read more about long-acting contraceptives on the FPA website.
Implant
The implant (Nexplanon) is a small flexible plastic rod that's placed under the skin in your upper arm. It releases the hormone progestogen into your bloodstream and lasts for three years. It can be easily removed if it doesn’t suit you. Once removed, your fertility will return to normal immediately. There are some drug interactions between the implant and some anti- HIV medications, so it’s important to talk to your HIV clinic if you would like to use this method.
Condoms
Condoms are an effective way to prevent pregnancy when used consistently and correctly, and they are the only form of contraception that also protect against sexually transmitted infections. There are both external (used over the penis) and internal (used inside a vagina or anus) condoms.
Condoms can also prevent HIV transmission to HIV-negative partners if you do not have an undetectable viral load. If you have an undetectable viral load, you do not need to use condoms to prevent HIV transmission. People with an undetectable viral load cannot pass on HIV during sex.
Condoms are not as effective as long-acting reversible contraceptives. They need to be used properly and consistently in order for them to be effective. Some people choose another form of contraception as a back-up and to feel more in control. It is very important to use condoms correctly. You can find out how on NAM’s page, Condoms.
Diaphragms and caps
Diaphragms and caps (contraceptive devices you place in the vagina each time you have sex) are not recommended for people who have HIV. This is because they are normally used with a spermicide, a substance that can lead to irritation, genital sores and lesions. These sores or lesions, which you may not realise you have, can increase your risk of passing HIV on to an HIV-negative sexual partner if you do not have an undetectable viral load.
Hormonal contraception and gender-affirming hormones
For any trans masculine or non-binary people who are taking testosterone, exploring progesterone-only methods of contraception will provide good protection again unwanted pregnancy without affecting your hormones.
Getting contraception
In the UK, contraception is available free, provided by the National Health Service (NHS). You will not have to pay a prescription charge. Contraception is available from GPs, and from community contraceptive clinics and sexual health (GUM) clinics. Details of local clinics are available from NHS Choices. HIV treatment centres offer condoms free of charge.
