While the majority of cases of syphilis in the UK are still in gay and bisexual men who have sex with men and transgender women, the proportion of cases in heterosexuals and particularly women has risen in the last decade.
In the last full year of data (2024) the UK Health Security Agency reports that diagnoses of syphilis in England have risen by 4.6% compared with 2023, whereas there have been significant declines in chlamydia (down 13%) and gonorrhoea (down 16%). Syphilis cases in gay and bisexual men slightly declined, from 6435 to 6330, but there was a 24% increase in heterosexual men.
Women still only represent a relatively small number of cases (828 – just over 6%). But while there was no increase in women last year, in the last decade, cases have more than trebled (up 217%) in women compared with rises of 53% in gay and bisexual men and 130% in heterosexual men.
There has also been an increase in cases of vertical transmission, resulting in babies born with congenital syphilis – a very serious condition.
Women with syphilis in Manchester
At the recent joint conference of the British HIV Association (BHIVA) and the British Association of Sexual Health and HIV (BASHH) in Liverpool, Dr Rachel Kirby of The Northern sexual health clinic in Manchester analysed the characteristics of 40 women diagnosed in the region who attended services such as The Northern, the sex worker support service MASH, and antenatal and other services in the area.
The majority were of White ethnicity but there was an over-representation of Black women relative to the population, and an under-representation of Asian women.
The majority (22 out of 40) had been diagnosed outside sexual health services, mainly in antenatal services. Most of the women were diagnosed at the late latent stage of syphilis, when the body has come to a temporary but not permanent accommodation to the infection. People are less infectious sexually at this stage, but syphilis can still be passed on from mother to baby in the womb.
Six of the 40 women (15%) did not receive treatment or did not complete the course (which consists of one penicillin injection for early syphilis or two for late) and 57% did not return to their three-month follow-up appointment to see if they had been cured.
The research team compared psychosocial characteristics of women diagnosed with syphilis with the characteristics of women diagnosed with chlamydia in the same area. They were much more likely to be engaged in sex work (34% versus 2%), be homeless or in unstable housing (11% versus zero), currently using recreational drugs (45% versus 5%) and to have experienced domestic violence (33% versus 8%) and child sexual abuse (18% versus 10%).
Dr Kirby told the conference that their study indicated the need for a comprehensive psychosocial assessment of women presenting to or at risk of syphilis, more training for medical colleagues who are not sexual health specialists, the preservation of street outreach services, and the provision of doxyPEP for women, which at present is not recommended in guidelines.
Syphilis – and doxyPEP – in Leeds sex workers
One outreach service for commercial sex workers that has started to provide doxyPEP is located just over the Pennines in Leeds. A poster by Dr Amy Evans and colleagues at Leeds Sexual Health documented an outbreak of syphilis among female sex workers, their partners and clients, starting in September 2024. Unlike in Manchester, these were all cases of early syphilis – which suggests a recent introduction into the community. A multidisciplinary team was formed of clinicians, public health workers and local government to deal with the outbreak.
By April 2026 the team had diagnosed 18 confirmed cases of primary and early secondary syphilis in 17 women (one re-infected), 10 cases in male contacts, one secondary case in a contact of one of these men, and a couple more cases, one male, one female, pending verification.
Unlike the cases in Manchester, 80% of the women, whose average age is 33, were of White British ethnicity. Like the Manchester women, though, they were a very vulnerable group. All but one of the 18 women diagnosed (94%) had smoked crack; the same proportion had worked on the streets some or all of the time; 13 out of 18 were homeless or had insecure housing; and ten out of 18 had injected drugs.
The multidisciplinary team addressing the outbreak decided to provide doxyPEP for women using their service, but this was not a simple task for such a group, neither in terms of providing information and securing consent, nor in terms of dispensing. There is now one high-street pharmacy which can provide 48 tablets at a time to clients who have formally given their consent; alternatively, those receiving methadone from local pharmacies can nominate their chosen pharmacy to provide 20 tablets at a time; and finally Leeds Sexual Health can provide doxyPEP from their outreach van or at their clinic premises.
As people subject to unpredictable risk, the women are advised to take a minimum of one dose per week and no more than one a day. The doxyPEP is being offered alongside two-monthly pregnancy and STI testing, HIV PrEP, and vaccinations for hepatitis B, gonorrhoea and HPV.
Diagnosing syphilis in non-routine settings
Syphilis is often missed in other settings, too. Fleur Preedy of Brighton and Sussex Medical School reviewed cases diagnosed in ‘non-routine’ settings in the local NHS trust. ‘Routine’ means settings where either the patient has come for an STI test or where a test is part of a standard package, as in antenatal care.
Between 2020 and 2025 the trust performed 56,816 antibody tests for syphilis, 86% of them in routine settings. This left 8149 tests taken in non-routine settings. Of these, 143 were positive – about one in 50 non-routine tests and one in 400 of all tests.
Three settings returned the highest proportion of positive tests. Among 609 tests taken in patients admitted to infectious disease wards, nearly 7% were positive for syphilis. In acute (A&E) settings, just under 3% were positive and in out-patients being treated for infectious diseases, 2.5%. No more than 1% of tests taken in other departments were positive, apart from rheumatology (1.3%).
When the researchers looked back at medical notes, they found cases where opportunities to test for syphilis had been missed. An analysis of six patients (four gay men, one heterosexual man and one woman) showed delays in diagnosis after presentations of quite severe symptoms. These ranged from abscesses to inflamed joints, weight loss, hearing loss, neuropathy and abnormal liver function results, and a delay in diagnosis ranging from one to 40 months.
Syphilis is called “the great imitator” as it can cause highly varied symptoms suggestive of many other conditions, and these patients underwent some unnecessary investigations, some invasive or involving exposure to radiation. “Severe psychological distress” was noted in a couple of the patients. The patient with the longest wait for diagnosis was a gay man in his 50s with fatigue, a rash and neurological symptoms who was refused a syphilis test several times by his GP and audiologist. Through his own research he suspected he had syphilis and eventually ordered a private test, but was left with permanent hearing loss.
Syphilis in pregnancy and babies
Syphilis, once diagnosed, can be successfully treated and severe complications are quite rare in adults. This is not the case for babies born with congenital syphilis, a condition that causes significant mortality and morbidity.
In the UK, this is a rare condition, with just 2.5 cases per 100,000 live births (one in 40,000) but globally is nearly 200 times more common, with 473 cases per 100 live births (one in 211). The US sees over 100 cases per 100,000 live births, concentrated among Black populations in the southern states.
Syphilis screening is recommended for all pregnant women. Between 2020 and 2024 syphilis was diagnosed in 1341 pregnant women, according to a poster by Dr Helen Peters of the Integrated Screening Outcomes Surveillance Service (ISOSS).
Most were successfully treated, but in 72 cases women were treated less than four weeks before delivery; in 10 cases this was because they initially screened negative and acquired syphilis later in pregnancy. Fifty-two were never treated, including 25 who were only diagnosed in labour.
In an oral presentation, Peters reported that there had been 13 cases of babies born with congenial syphilis in the last full-data year of 2023. However, this is more than twice the number seen each year between 2015 and 2018. Overall, between 2015 and 2024, 79 vertical transmissions were reported.
Fourteen of these were stillbirths and seven more died less than a week after birth. Babies born with syphilis may have immediate symptoms such as skin lesions and peeling skin, severe nasal congestion, enlarged liver and spleen and general failure to thrive, but in other cases symptoms may not appear for two years, and children may then present with skeletal deformities and neurological symptoms. While prompt penicillin treatment can cure congenital syphilis, it cannot reverse damage done before treatment.
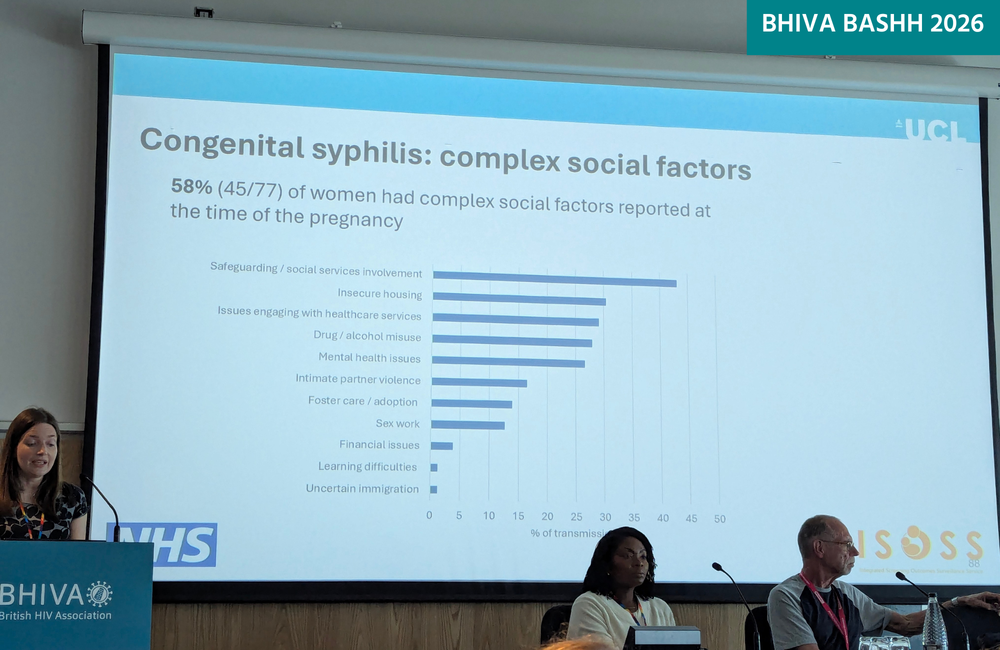
The mothers of the babies born with syphilis were quite young on average (27), predominantly of White ethnicity (a significant number were east European) and 58% of them had complex social factors reported at the time of pregnancy (compared with 38% of mothers with syphilis generally). Fifty-seven per cent were involved with social services, 38% were in insecure housing, 36% had drug or alcohol issues, 21% reported intimate partner violence and 17% had engaged in sex work.
“These findings,” Peters said, “highlight the importance of education for good sexual health in pregnancy… the need to raise awareness amongst healthcare professionals, and considerations for national screening strategies.”
Kirby R et al. Syphilis in Cisgender Women: Exploring the Challenges in Diagnosis, Treatment and Psychosocial Needs. Sixth Joint Conference of the British HIV Association (BHIVA) and the British Association for Sexual Health and HIV (BASSH), abstract O14, Liverpool, 2026.
Evans A (presenter Walker V) et al. Street sex worker outbreak and response 2: early syphilis. DoxyPEP: can we do it? Sixth Joint Conference of the British HIV Association (BHIVA) and the British Association for Sexual Health and HIV (BASSH), abstract A052, Liverpool, 2026.
Smith S (presenter Preedy F) et al. A retrospective review of syphilis testing in non-routine hospital settings between 2020 and 2025. Sixth Joint Conference of the British HIV Association (BHIVA) and the British Association for Sexual Health and HIV (BASSH), abstract O13, Liverpool, 2026.
Peters H et al. Characteristics and care of women diagnosed with syphilis in pregnancy in England, 2020 to 2024. Sixth Joint Conference of the British HIV Association (BHIVA) and the British Association for Sexual Health and HIV (BASSH), abstract A054, Liverpool, 2026.
Francis F et al (presenter Peters H). Factors contributing to increasing numbers of congenital syphilis in England 2015-2024. Sixth Joint Conference of the British HIV Association (BHIVA) and the British Association for Sexual Health and HIV (BASSH), abstract O12, Liverpool, 2026.
