Globally, UNAIDS estimates that by the end of 2021, 75% of all people with HIV in the world were accessing treatment.
But “accessing treatment” in fact just means that this number have initiated treatment at some point. It is not the number on treatment right now, because it does not try to estimate how many people starting treatment may have dropped out of care. Back in 2015, one study estimated that a quarter or more of people initiating antiretroviral therapy (ART) in low- and middle-income countries had stopped treatment within two years of initiation.
The British HIV Association last month heard that there are now considerably more people with HIV in England who are already diagnosed, but have dropped out of care, than people who remain undiagnosed.
It is hard enough to establish if people have dropped out of care in the context of England; it’s more so in lower-income settings where monitoring and surveillance may be less thorough and some populations are more mobile. But there are sometimes ways to find out if people starting ART are in fact re-starting it, and to derive estimates of treatment attrition from that.
Dr Mariet Benade and colleagues from Boston University and the University of the Witwatersrand in South Africa reviewed studies of HIV treatment initiation in Africa to answer one question: What proportion of the number of people coming forward for ART as new patients had in fact taken the medication before?
The study
Only studies published from 2018 onwards, with data from 2016 onwards, were selected for this review because before that time, ART was less widely available in Africa and previous use would have been less common.
The researchers reviewed 332 studies of ART initiation and, as they comment: “Perhaps the most striking finding of this review is the sheer lack of research evidence to answer our research question”. They only found ten studies that answered it.
"It is reasonable to conclude that between 20% and 50% of patients who present for ART are re-initiators.”
Those ten studies are so different from each other and assess prior ART use in such varied ways that a general average figure for previous use cannot be produced. Five of them were conducted in South Africa, two in Kenya and one each in Botswana, the Democratic Republic of Congo, and Ethiopia. One (the smallest) was among gay and bisexual men only, the others among men and women. The ten studies collect data on 3503 people, including 59% of women, whose average age at ART initiation was 34.
Their methods and aims were very varied. The one in Botswana involved testing out a national HIV prevention campaign, and house-to-house HIV testing and ART use was assessed at the start. The one in the Democratic Republic of Congo recruited both people already on ART and people starting it, and assessed the results of starting on or switching to dolutegravir. The Ethiopian study was a cross-sectional study to assess how many people were experiencing treatment failure six months after starting it. Both Kenyan and two of the South African studies compared initiating ART on the day of diagnosis versus starting it later; one compared ART delivered to people’s homes versus clinic dispensing; one looked at whether regular point-of-care viral load testing in people who had started ART resulted in less treatment failure, and the last looked at the proportion of people starting treatment who had prior drug resistance – this last study had the most rigorous methods of establishing prior ART use, as this was obviously crucial to the study objective.
Five of the studies relied on self-report; in other words, they asked people starting treatment, in one way or another, “Have you ever taken HIV treatment before?".
Three of the studies took undetectable viral load at presentation as evidence that people had taken ART. This is an interesting idea; it may over-estimate prior ART use if there are some elite controllers maintaining viral suppression off ART in the population; on the other hand, it is more likely to underestimate it, as people who have been off ART for more than a few months will no longer be virally suppressed. One study combined it with testing blood for evidence of ARVs and also with combing medical records to see if prior ART prescription was recorded. The resistance study used the ‘gold standard’ method of measuring drug levels in dried blood spots and hair samples, which can record use over a long period. Finally, the Botswana study only reported that 7% of people recruited had taken ART before without explaining how they reached that figure.
The findings
If we take the five studies that relied on self-report, the average proportion of people declaring prior ART use was 9.2%, with a range from 2% to 21%. In the four studies that used more objective measures, the proportion with evidence of prior ART use was 42%, ranging from 30% to 55% – with the study using drug levels in hair and dried blood spots producing the 55% figure.
This illustrates something that researchers into condom use, PrEP use and breastfeeding already know well: people coming forward for studies tend not to admit to behaviour that they think researchers or healthcare staff will disapprove of, or which they think may exclude them from the study. The authors say that “it is reasonable (and conservative) to conclude that between 20% and 50% of patients – and likely at least 30% – who present for ART are re-initiators.”
They also comment that more studies may have the the number of re-initiators buried somewhere in their data, but that the researchers simply didn’t think it was important enough to publish. For instance, some studies exclude people who declare previous ART use at the point of enrolment without comment. But it is striking that many researchers seem not yet to take into account that, these days, prior use of antiretrovirals may be quite common among people presenting for HIV treatment in African countries.
Prior ARV use, the authors comment, may not only be for treatment, either: it is increasingly likely that people may previously have been on PrEP, and women with HIV may have taken a short course of ARVs to prevent mother-to-child transmission, but not stayed on it as treatment. In both cases, people may be unsure how to answer the question “Have you been on HIV treatment before?”.
If this review answers one question usefully, it is that asking people if they have previously used ARVs is not a reliable way of establishing whether people have previously dropped out of care. More objective measures must be sought, whether that is better and more co-ordinated monitoring and tracing of people who drop out, or developing cost-effective objective assays for prior ARV use.
The authors say even self-report is better than nothing, though: “In view of the potentially very high proportion of re-initiators among 'new' ART patients, it is critical that researchers begin to report the proportion naïve and non-naïve as a standard variable when describing patient cohorts, even if data come solely from self-report.”
They add: “In earlier years, when the proportion on non-naïve patients was low because treatment programmes were still rapidly expanding, the question of previous ART experience may not have been a priority. In view of the results from the few studies available, it is clearly a priority now.”
Benade M et al. Prior exposure to antiretroviral therapy among adult patients presenting for HIV treatment initiation or re-initiation in sub-Saharan Africa: a systematic review. MedRxiv pre-print, 21 October 2022 (open access). https://doi.org/10.1101/2022.10.19.22281280
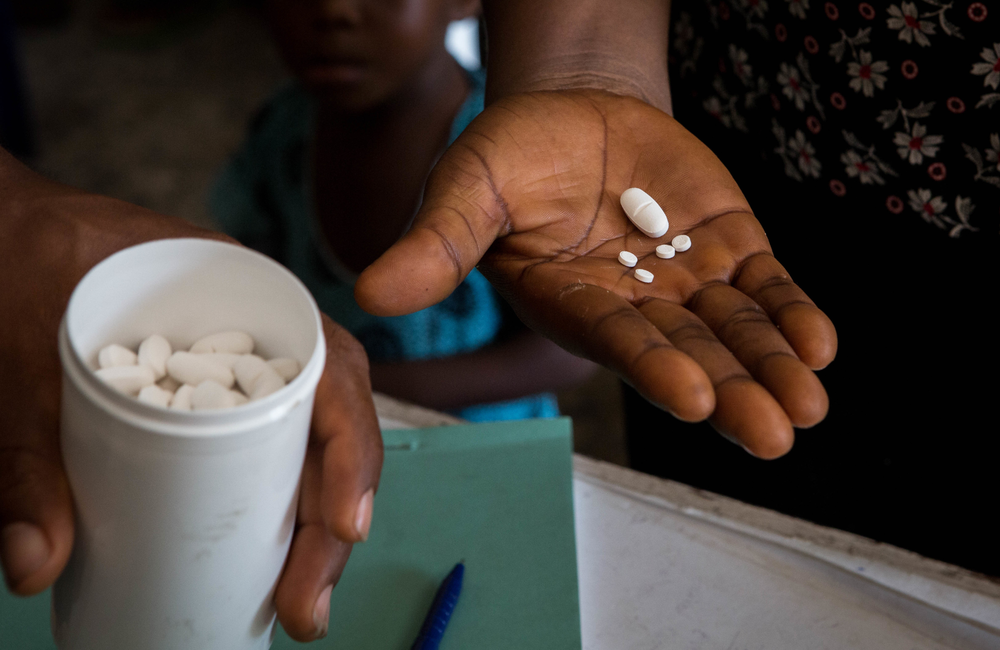
Full image credit: Fighting NTDs in Cross River State, Nigeria. Image by RTI International/Ruth McDowall. Available at www.flickr.com/photos/rtifightsntds/35759735125 under a Creative Commons licence CC BY-NC-ND 2.0.
