We do not know how much injectable cabotegravir, the first long-acting formulation of pre-exposure prophylaxis (PrEP), will be priced at when it comes on the market, probably late this year or early next year.
But a cost-effectiveness analysis presented to the virtual Conference on Retroviruses and Opportunistic Infections (CROI 2021) by Dr Anne Neilan of Massachusetts General Hospital found that in order to be remotely cost-effective in the United States, it would have to cost less than half of the list (maximum) price currently being charged for the only injectable drugs for antiretroviral therapy currently on the market, the cabotegravir/rilpivirine combination Cabenuva which was licensed by the US Food and Drug Administration in January.
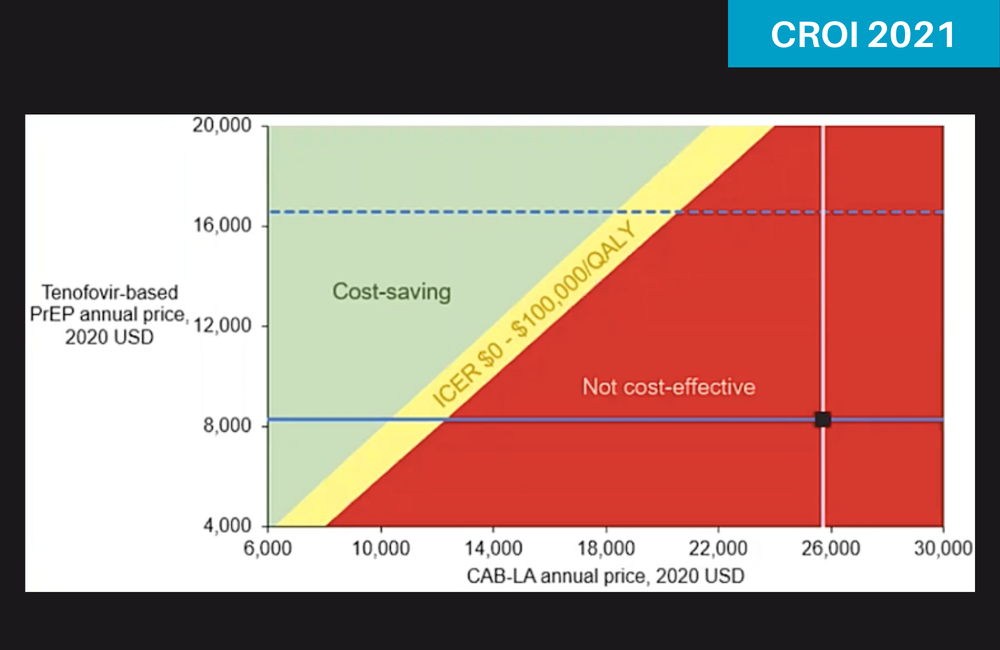
Given the current listed price of generic tenofovir disoproxil fumarate/emtricitabine (TDF/FTC) in the USA, which is $8300 a year, then injectable cabotegravir (CAB-LA) would have to cost no more than $10,200 to save money over the course of ten years relative to TDF/FTC, if used in a population similar to the participants in the HPTN 083 study.
At a price of $11,600 a year, it would cost just below $100,000 per extra quality-adjusted life year (QALY) saved, which is the maximum threshold for what’s usually regarded as cost-effective in the US.
In Europe and many other countries, generic TDF/FTC or TDF/3TC (lamivudine) can be bought for as little as £19-£56 a month, which is about $300-$900 a year. Although Neilan’s model did not compare CAB-LA with generics at such prices, its logic implies that because of the superior effectiveness of CAB-LA preventing HIV infections, it could still be cost-effective or cost-saving in the long run, even in a European scenario, but only at a price of perhaps $2000-$3000 a year.
“How much will the US health system be prepared to pay for improved efficacy?” Neilan asked.
The model
It is important to note that her model compares the cost-effectiveness or cost-saving of-CAB LA to current oral PrEP – in other words, how much the heath system would spend or gain over the ten-year period if everyone currently on oral PrEP switched to injectable PrEP.
The model does not take account of people who do not want to take oral PrEP but would be interested in the injectable version, and it does not directly compare no PrEP with injectable PrEP. A model that did this might find more favourable cost-effectiveness for CAB-LA.
The model was a stepped one in which:
- The cost and effectiveness of TDF/FTC were compared with no PrEP.
- The cost of on-patent tenofovir alafenamide (TAF/FTC) PrEP (Descovy) was then compared with TDF/FTC.
- The cost and effectiveness of CAB-LA was then compared with Descovy.
This built a picture of how much extra cost spent on the three progressively more expensive PrEP medications could be justified.
The model was based on the demographic and behavioural characteristics of US participants in the HPTN 083 study, and estimated that the US population with these characteristics totalled 480,000 gay and bisexual men and trans women at high risk of HIV.
The outcomes of the model were the number of primary HIV transmissions averted (the model did not attempt to account for secondary transmissions); the gain in QALYs that would result; how much this would altogether cost or save, if the cost-saving of the averted HIV infections was subtracted from the PrEP cost; and finally the incremental cost-effectiveness ration or ICER, which is the amount of money each PrEP prescription would cost, divided by the cost of each individual HIV infection that would happen otherwise.
The ICER is the crucial calculation when deciding if a medical intervention is cost-effective. It is understood that some medical interventions are worth paying a net monetary cost for if they add significantly to life expectancy or public health. There is no hard-and-fast definition of cost-effectiveness, but in the US an upper boundary of $100,000 per QALY gained is often quoted, which was the definition used in this study. In Europe this tends to be much lower, in the region of £20,000 or so per QALY gained. It is even better, of course, if the ICER is negative rather than positive, i.e. the new intervention provides a net saving to the health service – a cost-saving intervention.
The ICER is rarely calculated for just a year, as an intervention may lead to better health over many years. The time horizon calculated here, of costs/savings achieved in ten years, is relatively short; the cost-effectiveness models worked out for PrEP cost-effectiveness in the UK, for instance, had timelines of 40 years.
The inputs
The inputs or assumptions fed into each model are crucial; a model may produce contra-factual results if the inputs are not backed up by strong evidence. In this case there was a strong evidence-base behind them, either taken directly from HPTN 083’s data or from listed drugs prices.
The inputs were as follows:
- Population size: 480,000
- Average age at baseline: 30
- Annual HIV transmissions within population without PrEP: 18,000
- Annual HIV incidence without PrEP: 5.3%
- Annual HIV incidence on TDF/FTC or TAF/FTC: 1.3%
- Annual HIV incidence on CAB-LA: 0.3%
- Retention: 28% who started PrEP would still be on it after six years. Rejoining was not calculated.
The starting costs were derived from prices in federal supply catalogues. The one big unknown was the price of CAB-LA as it is not yet for sale.
So Dr Neilan’s team used the list price of injectable cabotegravir/rilpivirine, which is now licensed for HIV treatment as Cabenuva. This was assumed to be a maximum.
Annual drug costs were as follows:
- Generic TDF/FTC: $8300, plus $400 programme costs = $8700
- Branded TAF/FTC: $16,600, plus $400 programme costs = $17,000
- CAB-LA: $25,800, plus increased programme costs (due to more apppointments) of $700 = $26,500
- Antiretroviral therapy for people who acquire HIV: ranging from $32,000 a year for first-line therapy to $69,000 for third-line and subsequent therapy.
The reason for the introduction of TAF/FTC was of course to avoid the well-known effects of TDF on kidney function and bone density. It was assumed 2% of TDF/FTC users would have to stop due to side effects each year and the side effects would incur added costs of $5000 a year in these people.
A separate analysis was also done on all gay and bisexual men and trans women with at least moderate risk of HIV in the US: the size of this population was calculated at 1.9 million and their average annual HIV incidence 1.5%, with incidences on PrEP adjusted accordingly.
Outputs
Over ten years, this model calculated that there would be 178,000 new HIV infections if there was no PrEP; 122,000 if either TDF/FTC or TAF/FTC was used; and 107,000 if CAB-LA was used.
The cost of health care, before taking the reduction in HIV cases into account, rose as PrEP was used. Total medical care for the 480,000 people over the ten years would cost $33 billion with no PrEP; $45 billion if TDF/FTC was used; $60 billion if TAF/FTC was used; and $76 billion if CAB-LA was used.
But if TDF/FTC PrEP was used it would keep an extra 9700 people alive in good health over the ten years (i.e. it would add 97,000 QALYs); TDF/FTC would add another 2000 QALYs on top of that, due to side effects being avoided; and CAB-LA would add another 26,000 QALYs on top of that.
To put it another way: over ten years, if there were no PrEP, the total years enjoyed in good health by the subject population would be 4,500,000. But if they all started CAB-LA PrEP, they would have 4,654,000 years in good health.
So would these extra years of good-quality life be worth the cost?
Bluntly, at the starting prices used, no. Not even for generic TDF/FTC. This would cost $122,000 per QALY saved; already above the threshold for cost-effectiveness, though not so far over the threshold that it’s impossible to imagine it being cost-effective or even cost-saving if the price of generic PrEP were to be sufficiently reduced.
The ICER of TAF/FTC was “dominated”, in other words it was more expensive and delivered fewer benefits than the alternatives. Remember that this is a layered model in which the question is: what are the extra costs (or benefits) of each new form of PrEP over the previous one? The small reduction in costs due to eliminating side effects would not only not be outweighed by the fact that the price of TAF/FTC is double that of TDF/FTC, it would not even be outweighed by the extra cost of CAB-LA, due to its much bigger positive effect on QALYs. So it was left out of the model and TDF/FTC compared directly with CAB-LA.
The incremental ICER of CAB-LA in comparison with the ICER of TDF/FTC was $1,069,000. In other words, at starting prices, that would be the startling cost of each added QALY if each person using TDF/FTC substituted CAB-LA.
But these were just starting prices. The question is, at what price does CAB-LA start to become cost-effective compared with TDF/FTC? When does the gain in QALYs start to outweigh its extra monetary cost?
The answer is that if the annual price of generic TDF/FTC stayed the same at $8300, then CAB-LA would become cost-effective at $11,600 a year, or $3000 more than generic PrEP. And it would actually become cost-saving, i.e. represent a net monetary benefit to the healthcare system over ten years, if it cost $10,200 a year, or $1900 a year more than TDF/FTC.
If it was given to all 1.9 million gay and bisexual men and trans women at moderate risk of HIV, it could cost no more than $1000 more than TDF/FTC to be cost-effective.
The diagram can also be read the other way: if TDF/FTC cost less, what would CAB-LA have to cost in order to still be a net money saver? As you can see from the diagram Neilan showed, if TDF/FTC cost $4000 a year, then CAB-LA would be cost saving at just over $6000 a year.
Her diagram does not extrapolate downward to the much lower prices of generic PrEP in Europe, but if the model is linear, then it implies that at an annual TDF/FTC cost of $500 a year – which is £30.00 a month – then CAB-LA might become cost-saving at a price of something like $2500 (£1790, €2090) a year or $417 a shot.
Again, this is if everyone switched from TDF/FTC to CAB-LA: if CAB-LA led to a net increase in the number of people using PrEP, then it could save more money and justify a slightly higher price.
This is not impossible to achieve. CAB-LA was based on previous injectables medications such as the contraceptive Depo-Provera. This now costs a maximum of $150 per three-monthly shot, according to Planned Parenthood.
Anne Neilan commented in conclusion: “CAB-LA should be priced to compete with generic, rather than branded, tenofovir-based PrEP. The availability of effective alternatives limits the additional price payers should be willing to pay for CAB-LA as PrEP.”
Neilan AM et al. Cost-effectiveness of long-acting PrEP among MSM/TGW in the US. Conference on Retroviruses and Opportunistic Infections, abstract 150, 2021.
Download the abstract eBook from the conference website.
Update: Following the conference presentation, this study was published in a peer-reviewed journal:
Neilan AM et al. Cost-Effectiveness of Long-Acting Injectable HIV Preexposure Prophylaxis in the United States. Annals of Internal Medicine, 175: 479-489, April 2022.
https://doi.org/10.7326/M21-1548
