
Same life expectancy as HIV-negative people, but far fewer years in good health
Once again, a life expectancy study has shown that HIV-positive people who start antiretroviral therapy (ART) promptly and have good access to medical care live as long as their HIV-negative peers. But the researchers found that HIV-positive people were living with additional health problems for many of those years – on average, they had major co-morbidities 16 years earlier than HIV-negative people.
The study was presented last week to the Conference on Retroviruses and Opportunistic Infections (CROI 2020). Research was presented online after the scheduled meeting in Boston was cancelled due to concerns about the new coronavirus, COVID-19.
This US study looked specifically at people who had access to health care – all participants were enrolled in Kaiser Permanente, an integrated provider of health insurance and medical care in California, Virginia, Maryland and the District of Columbia.
Data came from 39,000 people living with HIV and 387,767 HIV-negative people. Each person with HIV was matched with ten HIV-negative people according to age, gender, ethnicity and year enrolled.
The results showed a steadily increasing life expectancy for people with HIV over the study period, 2000 to 2016. Whereas in the year 2000 people with HIV were, on average, expected to live 22 fewer years than HIV-negative people in the cohort, by 2016 this had narrowed to nine fewer years. By 2016, if the person with HIV started ART with a CD4 count above 500, they would be expected to live a little longer than those without HIV.
However, the researchers also looked for indications of chronic liver disease (including hepatitis B or C), chronic kidney disease, chronic lung disease, cardiovascular disease, diabetes or cancer.
They found that people with HIV live substantially fewer healthy years than people without HIV. In the period 2014 to 2016, an HIV-positive 21-year-old could expect to live without any of these health problems to the age of 36, whereas their HIV-negative peer would do so to the age of 52. The onset of liver disease occurred 24 years earlier for people with HIV, kidney disease 17 years earlier and lung disease 16 years earlier.
A potential limitation with this study is that people living with HIV tend to see their doctors regularly and be screened more often than other people. As a result, chronic health conditions may be diagnosed at an earlier age.
Related links
- Read this news story in full on aidsmap.com
- View the abstract on the conference website
- Visit our conference news pages for all our CROI 2020 coverage
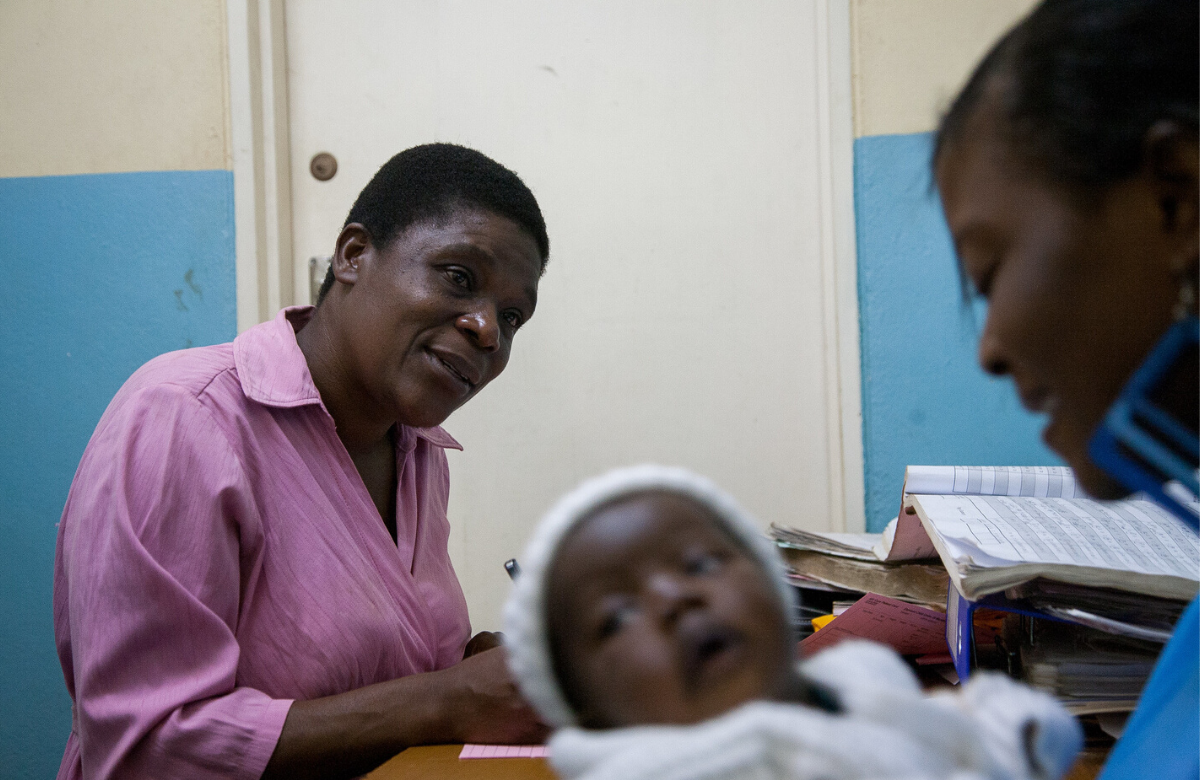
SEARCH study finds universal 'test and treat' reduces infant HIV
A large-scale community 'test and treat' campaign in Kenya and Uganda resulted in lower HIV transmission from mother to child and fewer infants living with HIV at the end of the study. The findings from the SEARCH study were presented to CROI 2020.
The study randomised communities to a standard-of-care approach to HIV treatment or to intensified community testing, treatment for all and streamlined referral to care. By the end of the three-year study, 80% of people with HIV in intervention communities achieved viral suppression compared to 68% in standard-of-care communities.
SEARCH is the first large test and treat study to report its findings on vertical (mother to baby) transmission. It found that vertical transmission was more than halved compared to the standard of care. Only 1.8% of infants born to women with HIV in communities that received the universal test and treat intervention had acquired HIV by the end of the study, compared to 4.4% in control communities.
The study investigators point to two possible mechanisms through which the study intervention may have reduced infant HIV infections: earlier diagnosis and treatment initiation among women who acquired HIV during the study period; and earlier treatment initiation among pregnant women, due to universal treatment.
Related links

Unique transgender vulnerabilities require tailored and specific interventions
Globally, trans women continue to have high rates of HIV, with an estimated prevalence of around 19%. Some estimates also suggest prevalence in trans men is as high as 8%.
Dr Asa Radix presented data on 557 trans men in New York City. Less than half had ever tested for HIV. HIV prevalence was around 3% in those who had tested but those who had cis male sexual partners had a much higher prevalence rate of 11%.
Dr Makobu Kimani of the Kenya Medical Research Institute presented data from a PrEP cohort on 11 trans women and 42 men who have sex with men (MSM) in Kenya. At six months, over 40% of the trans women had protective drug levels, but none of the MSM did. Interviews revealed that higher adherence among trans women was linked to more agency to take PrEP, perceived awareness of HIV risk, and feeling that PrEP affirmed gender identity.
Around half the sample were engaged in sex work, an issue that was explored in more depth by Mariëlle Kloek from Erasmus University using data from Zimbabwe. Among a sample of 603 cis male and trans sex workers, HIV prevalence was very high: 38% in trans women, 38% in trans men and 28% in cis men.
Encouraging outcomes were reported by Dr Catherine Lesko from the Johns Hopkins School of Public Health regarding retention in care for trans women in the US. Analysis of the NA-ACCORD cohort showed that once trans women have successfully engaged in HIV care, they have similar or better care outcomes than cis men or women.
Moderator Dr Sari Reisner of Harvard University emphasised that it is crucial to make a clear distinction between gender identity and sexual orientation, disaggregating different groups in research and service provision (for instance, separating trans women from MSM) and understanding their specific experiences and needs. Reisner also highlighted that gender affirmative practices are essential to making trans people feel welcomed and respected.
Related links
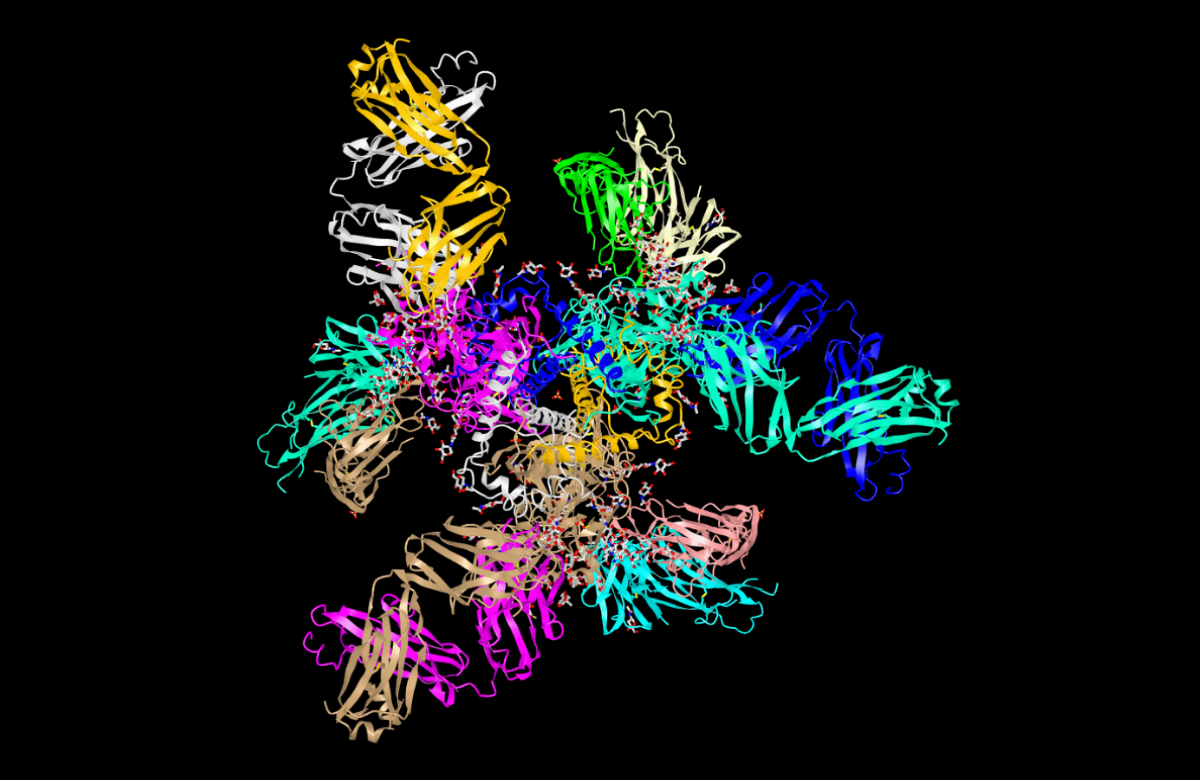
HIV vaccine that generates broadly neutralising antibodies passes first human safety study
Most vaccines work by inducing the B-cells of the immune system to make antibodies. Although previous trials have shown that some HIV vaccines can induce anti-HIV antibody responses, they have proved to be either ineffective (as in the recent HVTN 702 study) or only marginally effective (as in the RV 144 vaccine study).
Broadly neutralising antibodies (bNAbs) could form the basis of powerful vaccines and treatments, partly because they are active against a wide variety of viral strains. Last year, a vaccine study successfully induced monkeys to produce bNAbs. The successor to that study is underway in humans.
This year, CROI heard about a different technology: a study by the US National Institutes of Health that used a viral vector vaccine. This consisted of the shell of the adenovirus AAV-8, with its viral genes replaced by lengths of DNA that code for the production of VRC07, a bNAb that has been widely used in studies to develop HIV treatment, PrEP and a cure.
In a phase I safety study, the vaccine was given to eight HIV-positive volunteers. The first three volunteers were given a dose of 50 billion vector genomes per kilogram of body weight. Three months later, two more volunteers were given a vaccination containing ten times as many vectors per kilo (500 billion). The last three volunteers were given fifty times the original dose (2.5 trillion vectors/kg).
All volunteers given the vaccine produced VCRC07 antibodies, to a greater or lesser degree. However, as this is a safety study, we do not know yet whether the VRC07 levels produced are sufficient for an anti-viral effect.
This study offers the first proof that a vaccine can induce the production of bNAbs in humans.
Related links

Black MSM are 60% less likely to have suppressed HIV than white men in Atlanta
The Engagement Study – a community-based prospective cohort study – collected clinical and behavioural data from 398 HIV-positive black and white MSM living in Atlanta between 2016 and 2017. Half the sample were black; 33% of black men and 19% of white men were found not to be virally suppressed.
Age was a non-modifiable factor that contributed to differences in viral suppression, with younger men more likely not to be virally suppressed. Other factors were modifiable: access to health care, income, housing stability and marijuana use. Together, these factors completely accounted for the racial disparity.
Presenting, Dr Justin Knox from Columbia University concluded, “If we are serious about reducing racial disparities in HIV treatment outcomes, these results show that there are clear opportunities to target modifiable factors that would have an impact.”
Related links

Immune modulator clears pre-cancerous anal lesions
Anal cancer and its precursor, anal dysplasia (abnormal cell and tissue growth), is more common among people living with HIV compared with the general population.
The phase II SPACE study evaluated low-dose pomalidomide as a treatment for high-grade anal lesions. The study included ten HIV-positive and 16 HIV-negative men. All participants had biopsy-confirmed grade 3 high-grade lesions, which had lasted at least one year and a median of three years.
Just over half of study participants experienced complete or partial resolution of high-grade anal lesions after being treated with low-dose oral pomalidomide for six months, rising to 63% after an additional six months of post-treatment follow-up.
