Key points
- Herpes is transmitted by contact with skin where the herpes simplex virus is present. It causes painful blisters on the genital and surrounding areas.
- There’s no cure for herpes, but antiviral treatments can reduce the discomfort, severity, or frequency of herpes outbreaks.
- Having the herpes virus makes sexual transmission of HIV more likely if the person living with HIV is not undetectable. Herpes will not make a difference in HIV transmission if the person living with HIV has an undetectable viral load.
Herpes is caused by a common virus called herpes simplex virus (HSV). This is a common sexually transmitted infection throughout the world.
When you acquire the herpes virus, it stays in skin and nerve cells for life. However, you may not know that you have HSV. Most of the time, the infection does not cause symptoms, but the virus is still present, meaning that it can be passed on to others.
Oral and genital herpes
There are two main types of herpes virus, HSV 1 and 2. There are also two places that herpes can affect: your mouth/lips (oral herpes) and your genital/anal area (genital herpes).
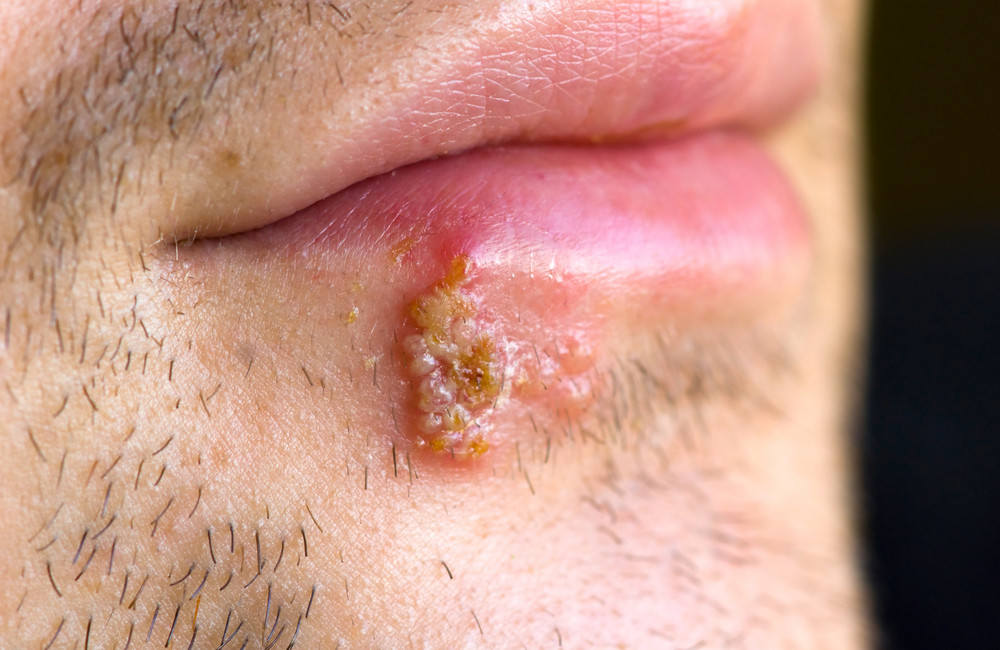
Oral herpes causes tingling or painful fluid-filled blisters on the edge of the lip where it meets the skin of the face (‘cold sores’). These can occasionally develop on the nostrils, on the gums or on the roof of the mouth.
Genital herpes involves painful, fluid-filled blisters in the genital or anal areas, sometimes accompanied by fever, headache, muscle ache and a general feeling of being unwell.
HSV 1 is most commonly associated with oral herpes, while HSV 2 is most commonly associated with genital herpes. But both viruses can cause either genital or oral herpes, and HSV 1 is now the leading cause of genital herpes in the UK.
Transmission and prevention
The virus can be transmitted from person to person by contact with skin where HSV is present. The virus passes easily through mucous membranes in the mouth, genital areas and anus, so can be passed on by kissing and other sexual contact. It can be passed from one part of the body to another, by touching the blisters or the fluid from them and then touching another part of the body. This can lead to particular problems if the infection is transferred to the eyes.
It is especially easy to get herpes when blisters are present, but it can also be transmitted when sores are not present. This is because the herpes virus may shed from the skin (called viral shedding) even when no outbreak is occurring. This viral shedding can infect partners, even with no other symptoms.
People who have genital herpes caused by HSV 2 typically have more viral shedding than people that have genital herpes caused by HSV 1. People with HIV are more likely to ‘shed’ virus, especially if they have a low CD4 count.
It is possible to pass herpes infection on to a baby through vaginal delivery. A caesarean section is recommended if you are pregnant and have an active outbreak of herpes at the time of delivery.
Avoid having sex (oral, anal or vaginal), if you have symptoms or feel them starting. Don’t share sex toys, or cover them with a condom or wash them between uses. Avoid kissing if you or your partner has a cold sore, or feel one coming. Avoid touching any affected area; thorough hand-washing will reduce the risk of spreading the infection if you do touch it.
Using a condom for anal, vaginal and oral sex offers a degree of protection from infection with herpes, or from passing on the virus to somebody else.
However, protection isn’t complete as the skin around the genital area may also carry the infection.
Some treatments may make it less likely for herpes to be transmitted. There’s more information on treatments later on this page.
Herpes and HIV infection
In a person with HIV who is not taking HIV treatment, herpes may make them more infectious. This is because untreated sexually transmitted infections can increase HIV viral load in genital fluids and because HIV is present in herpes blisters.
However, if the person with HIV is taking effective HIV treatment and has an undetectable viral load, they will not pass HIV on. Herpes will not make a difference to this. Taking your HIV treatment can also reduce the frequency of herpes outbreaks but has less of an effect on viral shedding.
HIV-negative people who have herpes blisters are more vulnerable to HIV infection, as the blisters provide a break in the skin through which HIV can enter.
Diagnosis
HSV is easiest to detect when the infection is still active, so it is best to seek medical advice as soon as you develop symptoms. It can be diagnosed by examining the affected skin, and by taking a swab of the fluid from a blister. A blood test can detect the virus, but this isn’t routinely used. A routine sexual health check won’t look for herpes unless you let staff know you have symptoms or are concerned.
Symptoms
Many people who have herpes will not have any symptoms at all. Others will have symptoms within a few days of infection.
An outbreak of herpes involves painful blisters or sores which affect the mouth or genitals. Herpes lesions (sores) often start as numbness, tingling or itching. This feeling indicates that the virus is travelling up a nerve to the skin. There it causes small bumps that rapidly develop into small inflamed and fluid-filled blisters. These burst and crust over, typically taking a week to heal in people with healthy immune systems.
The first occurrence of genital herpes can be severe and long-lasting and, in some cases, cause serious, systemic illness. This is more likely in people who are not on HIV treatment and whose immune system is very weakened.
Sometimes, people experience an initial outbreak within days of acquiring herpes. For others, they may have unknowingly been living with herpes for years before experiencing any outbreaks or symptoms.
From time to time, flare-ups (outbreaks) can occur. These are not usually as severe as an initial outbreak. Often, outbreaks become milder and less frequent as time goes on, usually after about two years. Genital herpes that is caused by HSV 2 recurs more often than genital herpes caused by HSV 1 and usually causes more severe outbreaks.
In people living with HIV, especially if they have a very low CD4 cell count (under 50), herpes outbreaks tend to be more frequent, more severe and last longer. Sometimes the lesions can become infected with other bacteria.
Some people find certain triggers will bring on an outbreak, such as being unwell, tired or stressed, friction in the genital area from sex or tight clothing, menstruation, drinking alcohol, smoking, and exposure to the sun or sunbed.
Treatment
There is no treatment that can eradicate (cure) infection with herpes viruses, but there are several antiviral treatments to treat herpes. They work by reducing the amount of viral replication while you are taking them. The most commonly used treatments are aciclovir, valaciclovir and famciclovir.
The best strategy for managing herpes may change over time depending on how frequently you have outbreaks, the severity of symptoms, and your sexual activity. Some people take antiviral medications on an as-needed basis when an outbreak occurs, called episodic therapy. Other people who experience more frequent or severe outbreaks may take antiviral medications daily, on an ongoing basis to prevent outbreaks. This is called suppressive therapy.
There are things you can do to help lessen the discomfort of an outbreak even without medications. These can be particularly helpful during an initial or severe outbreak. Taking painkillers or applying a topical anaesthetic, such as lidocaine, may be helpful. Using petroleum jelly on the blisters, bathing the affected area in salty water, or applying an ice pack or cold wet teabags, may also help. (Do not put ice directly on your skin.) Pouring water over your genitals while peeing can reduce the pain. Avoid tight clothing and drink plenty of fluids.
Episodic therapy
Antivirals can be taken as ‘episodic’ treatment, each time you feel the symptoms of the start of an outbreak (usually tingling and numbness). This can reduce both the severity and length of the outbreak.
The sooner you start treatment, the more effective it is likely to be. Although effective at preventing outbreaks of herpes, once an outbreak of genital herpes is established antivirals often provide little benefit. It is recommended people with HIV start antiviral treatment for HSV as soon as possible after an outbreak starts.
"Many people who have herpes will not have any symptoms at all. Others will have symptoms within a few days of infection."
Antivirals are usually taken in tablet form. Depending on the medication and dose, they may be prescribed for anywhere from one to five days, with you taking anywhere from one to five doses per day. For more serious outbreaks of oral herpes and genital or anal herpes, the treatment may be used for seven to ten days, and in the most serious cases, aciclovir can be given intravenously.
For many people with HIV, the standard episodic treatment course will work well. However, if you have a weakened immune system, you may need a longer course of antivirals.
Antiviral treatments for herpes infection work well in people with HIV when used to treat outbreaks. There is some evidence they work less well to suppress herpes virus shedding in people living with HIV than people who don’t have HIV.
Suppressive therapy
Daily antivirals can also be prescribed as ‘suppressive’ treatment on an ongoing basis. Suppressive treatment is usually prescribed in people who experience six or more outbreaks a year. In people with frequent outbreaks, suppressive treatment can reduce the frequency of these recurrences by 70-80%, and many people have no outbreaks when on suppressive therapy.
People living with HIV might need larger doses of medication to suppress their symptoms than those who are HIV negative. If you still experience outbreaks while taking suppressive therapy, talk to your doctor. They may increase your dose or switch the type of antivirals you are taking.
Research shows that taking suppressive therapy can also reduce (but not eliminate) the risk of transmitting genital herpes caused by HSV 2 to partners who do not have it.

