Key points
- PrEP is highly effective in preventing the transmission of HIV during sex.
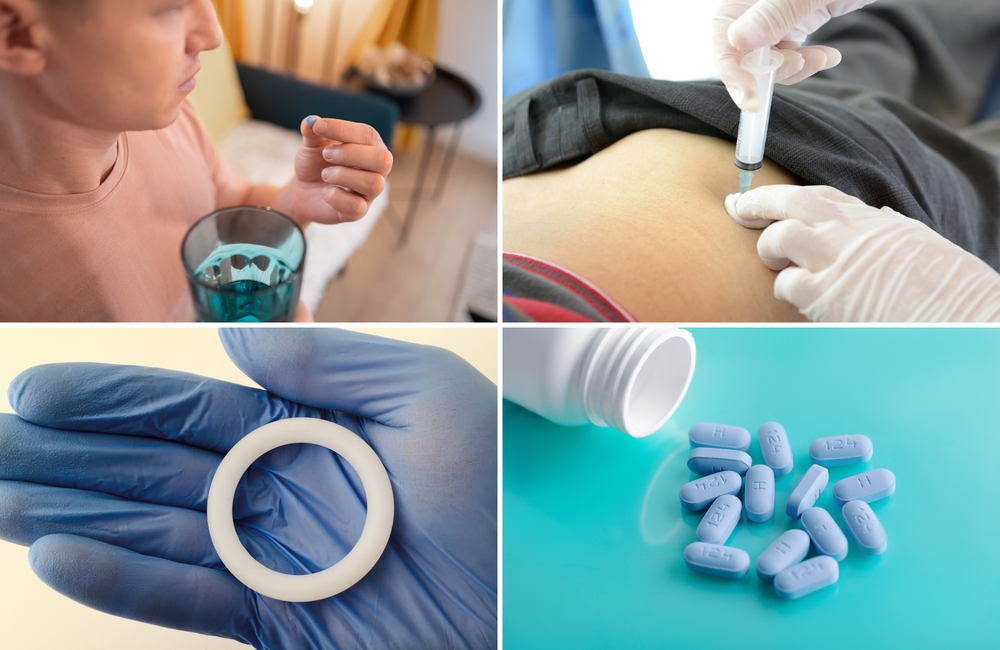
- There are several different forms of PrEP, including pills, injections and a vaginal ring.
- For PrEP to work well, it’s important to take it or use it consistently, as directed by your healthcare provider.
- While PrEP can prevent HIV, it does not protect against other sexually transmitted infections or pregnancy.
PrEP stand for pre-exposure prophylaxis. This means it prevents you from getting HIV by taking anti-HIV drugs. PrEP allows you to have the sex you want without the fear of contracting HIV.
The anti-HIV drugs in PrEP stop HIV from entering your cells and replicating. This prevents HIV from establishing itself and stops you from acquiring HIV.
PrEP options
There are several different types of PrEP:
- The most widely used type of PrEP is a tablet which contains two anti-HIV drugs, tenofovir disoproxil and emtricitabine. This is sometimes known as Truvada. You need to take this tablet every day or take several doses before and after sex to make sure that the drugs maintain high levels in your blood to prevent HIV infection.
- An alternative PrEP tablet contains tenofovir alafenamide and emtricitabine. This is taken daily and its brand name is Descovy. If you have concerns about your kidney or bone health, this may be more suitable than the other pill.
- Cabotegravir is a long-acting form of PrEP, taken by injection once every two months. Its brand name is Apretude.
- Lenacapavir is another long-acting form of PrEP, taken by injection once every six months. Its brand name is Yeytuo or Yeztugo, depending on which country you are in.
- The dapivirine vaginal ring is placed in the vagina and provides protection over the course of a month.
Would PrEP be right for you?
PrEP could be helpful if the sex you are having is not always as safe as you would like it to be. If it is sometimes difficult to use condoms or to be sure of your partner’s HIV status, PrEP could make the sex safer. If it’s likely that some of your sexual partners have HIV without realising it, then PrEP could help protect your health.
People are not expected to take PrEP forever. PrEP is most likely to be useful for a period of months or years when the risk of HIV is greatest. If you no longer feel at risk, you can discuss stopping PrEP with your healthcare provider. You’ll be able to re-start it later.
While PrEP provides protection against HIV, it does not protect against other sexually transmitted infections or prevent pregnancy. Condoms can provide protection against gonorrhoea, chlamydia, syphilis, hepatitis C and unwanted pregnancy.
PrEP isn’t the right choice for everyone. People who are able to consistently use condoms and other HIV prevention strategies don’t need PrEP.
If your partners definitely don’t have HIV, then PrEP isn’t needed. And if you have a partner who is living with HIV, taking HIV treatment and has an undetectable viral load, there is no risk of HIV transmission anyway. This is also called U=U.
Taking PrEP
Ideally, PrEP should be taken under medical supervision. This is because there are important things to consider before starting PrEP. You need to take an HIV test to check your HIV status. This is to ensure you don’t have HIV before you start taking PrEP.
It’s also recommended to take tests for sexually transmitted infections and pregnancy. If you are planning to use PrEP pills, you should also have tests for your kidney function and the hepatitis B virus. Healthcare providers may ask you some questions about your sexual behaviour and sexual partners before prescribing PrEP.
For PrEP to work, it needs to be taken correctly. This means having enough PrEP in your body at the times when you need protection. If you are taking pills, an occasional forgotten dose will not make PrEP ineffective. But for people who cannot adhere to their treatment and miss pills regularly, PrEP may not work. If you are taking injections, it is very important to attend your clinic as scheduled and receive the injections on time.
While taking PrEP, you will need regular clinic appointments to check for side effects and to repeat HIV testing, as well as for advice and support.
Is PrEP available?
Services which provide HIV testing, treatment for sexually transmitted infections or treatment for HIV may also provide PrEP – or have information on local services which do.
Not all types of PrEP are available in all countries. The most widely used type of PrEP is the tablet containing tenofovir disoproxil / emtricitabine (Truvada) and this is available in many countries. The other PrEP pill, tenofovir alafenamide / emtricitabine (Descovy), is available in a limited number of high-income countries.
At the time of writing, cabotegravir injections (Apretude) had been approved by drug regulators in over 60 countries in all parts of the world. Lenacapavir injections (Yeytuo, Yeztugo) have been approved by 14 drug regulatory agencies, including those of the United States, United Kingdom, European Union, Australia, Brazil, South Africa and Kenya.
You can check the PrEPWatch website to see which types of PrEP are approved for use in your country. But bear in mind that while drug regulators in your country may have approved a specific type of PrEP, it might not yet be available in clinics and local services. This is often because health organisations still need to make decisions on funding and reimbursement.
Which PrEP option would be right for you?
PrEP pills containing tenofovir disoproxil and emtricitabine (sometimes known as Truvada) are the most widely used and best studied type of PrEP. They are inexpensive and work well for most people.
However, if it would be difficult for you to take pills regularly without missing doses, then a long-acting form of PrEP might be a better option. If you would be able to stick to clinic appointments, then you could try PrEP injections. Or you may be able to use the vaginal ring – you insert it yourself and it stays in for a month at a time.
If you have concerns about your kidney or bone health, or if you are under the age of 18 (a critical time for bone growth), then PrEP pills containing tenofovir disoproxil and emtricitabine may not be the best option. One of the other types of PrEP might be more suitable.
People who have hepatitis B can take PrEP, but as one of the drugs in PrEP pills (tenofovir) is also active against hepatitis B, your doctor will need to take this into account. If you have hepatitis B and want to take a break from PrEP pills, you should discuss with your doctor how to safely stop taking them. This is not an issue with any of the other types of PrEP.
In terms of which type of PrEP is most effective in preventing HIV infection, studies show that PrEP pills and injections are both extremely effective when they are taken consistently, as prescribed. If you are comfortable taking pills and will remember to take them every day, PrEP pills are likely to work very well for you. Nonetheless, in studies, the fewest HIV infections were in people taking injectable PrEP – perhaps because it was more difficult to miss doses.
On the other hand, in studies so far, the dapivirine vaginal ring has provided a lower level of protection than other types of PrEP. It’s also important to bear in mind that the ring only protects against HIV during vaginal sex. It does not provide protection during anal sex.
There are specific pages on this website for each type of PrEP. They provide detailed information about how to start and stop using it, what to do if you miss a dose, required tests before starting PrEP, checkups while taking PrEP, side effects, drug interactions, drug resistance, using PrEP during pregnancy, which countries it is available in and how effective it is.
Click on the links to find out more about:
- Tenofovir disoproxil and emtricitabine pills (Truvada).
- Tenofovir alafenamide and emtricitabine pills (Descovy).
- Cabotegravir injections (Apretude).
- The dapivirine vaginal ring (DapiRing).
Image credits from top left: Kuboo/Shutterstock.com / saritwuttisan/iStock / iStock / Vaginal ring: Image by NIAID. Available at www.flickr.com/photos/niaid/25153111944 under a Creative Commons licence CC BY 2.0.
