Further evidence on the efficacy of two-drug antiretroviral regimens as simplification options for people with suppressed viral load on three-drug regimens was presented last week at the 17th European AIDS Conference in Basel, Switzerland.
However, German HIV specialist Professor Hans-Jürgen Stellbrink of the University of Hamburg sounded a note of caution about two-drug treatment during a discussion session at the conference, warning that “we're practising evolutionary biology on the virus by treatment, exerting the maximum selective pressure on the virus, and what I’ve learnt over 33 years is not to reduce that selective pressure on the virus.”
Updated European AIDS Clinical Society (EACS) guidelines now recommend five two-drug switch options for virologically suppressed people:
- dolutegravir and rilpivirine (Juluca)
- dolutegravir and lamivudine (Dovato)
- boosted darunavir and lamivudine
- boosted atazanavir and lamivudine
- boosted darunavir and rilpivirine.
EACS recommends dual therapy only where viral load has been undetectable for at least six months, there is no evidence of lamivudine resistance and no chronic hepatitis B infection.
Asked whether all two-drug combinations are equal, Stellbrink observed “I don’t believe they are entirely the same, but I also believe there’s no magic in the number of drugs. It’s about the effect and tolerance.”
Professor Jacques Reynes of the University of Montpellier, France, pointed out that two-drug regimens might be vulnerable if the person taking them has archived resistance to previous drugs, raising questions about both lamivudine and rilpivirine.
“But also, rilpivirine remains pharmacologically vulnerable throughout treatment," Prof. Stellbrink added. "You have the food effect [rilpivirine must be taken with food to ensure consistent drug levels] and drug interactions throughout treatment. So at any point after a long time on treatment someone might have sub-optimal concentrations and fail.”
The main rationale advanced for the use of two-drug regimens is to reduce the burden of long-term toxicities such as impaired kidney function or bone loss caused by tenofovir disoproxil fumarate (TDF), and cardiovascular risk increased by abacavir. Asked if prescribers are harming patients by continuing to use abacavir or tenofovir in ageing populations, Prof. Stellbrink replied: “This is what we all feel, but the promise of dual therapy is less toxicity and so far, this hasn’t been proven.”
Clinical trials presented at the conference addressed switching to dolutegravir/lamivudine, dolutegravir/emtricitabine, rilpivirine and boosted darunavir, as well as switch options where historical lamivudine resistance is documented.
TANGO: dolutegravir/lamivudine as a switch option
Forty-eight week sub-group analyses of the TANGO study were presented by Dr Jean van Wyk of ViiV Healthcare. In this study, 741 virally suppressed people were randomised to switch to dolutegravir/lamivudine or continue a tenofovir alafenamide-based three-drug regimen. The 48-week primary outcomes from the study were presented at IAS 2019, showing that switching to dolutegravir/lamivudine resulted in non-inferior viral suppression.
The median age of study participants was approximately 40 years; 14% of the switch arm and 16% of the tenofovir alafenamide (TAF) arm were black; but women were severely under-represented – only 7% of the switch arm and 9% of the TAF arm were female. Nine per cent of the switch arm and 8% of the TAF arm had a baseline CD4 count below 350. Around two-thirds of participants were taking a regimen containing elvitegravir and TAF at study entry.
At week 48, 93.2% of the switch arm and 93% of the TAF arm had viral load below 50 copies/ml. There was no significant difference in virological suppression between the two arms when the results were analysed by age, ethnicity, sex, baseline CD4 cell count or baseline regimen.
Drug-related adverse events that led to withdrawal from the study were somewhat more frequent in the two-drug arm (4% vs 1%) but were all mild to moderate (grade 2) adverse events. Participants in both arms gained a mean of 0.8kg in weight by 48 weeks. Adverse events were more common in the two-drug arm than the TAF arm in people over 50 and in women, although the numbers available for analysis make it difficult to draw conclusions.
Very small changes in renal and bone markers were observed during the study. Total cholesterol, total cholesterol: HDL cholesterol ratio, LDL cholesterol and insulin resistance improved significantly in people who switched to the two-drug regimen.
Simplification to dolutegravir and lamivudine with historical lamivudine resistance
Spanish researchers looked at whether it was safe for people with historical evidence of lamivudine resistance to switch to dolutegravir/lamivudine if virologically suppressed. Research in treatment-experienced people has shown that lamivudine can still suppress viral load even in the presence of the M184V mutation associated with resistance to the drug. Also, it is unclear to what extent drug-resistant variants persist in the HIV reservoir and whether these have any clinical relevance.
To test the impact of a switch and to learn more about the relevance of resistance, 20 people with historical evidence of the M184V mutation or the K65R mutation (associated with tenofovir resistance) and 21 people without historical resistance were followed for 48 weeks after switching to dolutegravir/lamivudine. The study excluded people with evidence of the M184V mutation in proviral DNA samples, on the grounds that this virus might be replication-competent and could lead to rebound of drug-resistant virus. All participants were dolutegravir-naïve and had had suppressed viral load for a median of 7.8 years.
At week 48, 18 out of 21 of the historical resistance group and all the no-resistance group had a viral load below 50 copies/ml. Two people in the historical resistance group discontinued treatment due to protocol violations and one due to adverse events, but no cases of virologic rebound were observed in the historical resistance group.
Ten cases of transient viral rebound above 50 copies/ml were observed during the 48-week follow-up period; in all cases viral load was re-suppressed. Six out of ten cases occurred in participants with no history of lamivudine resistance.
New two-drug switch option: rilpivirine and boosted darunavir
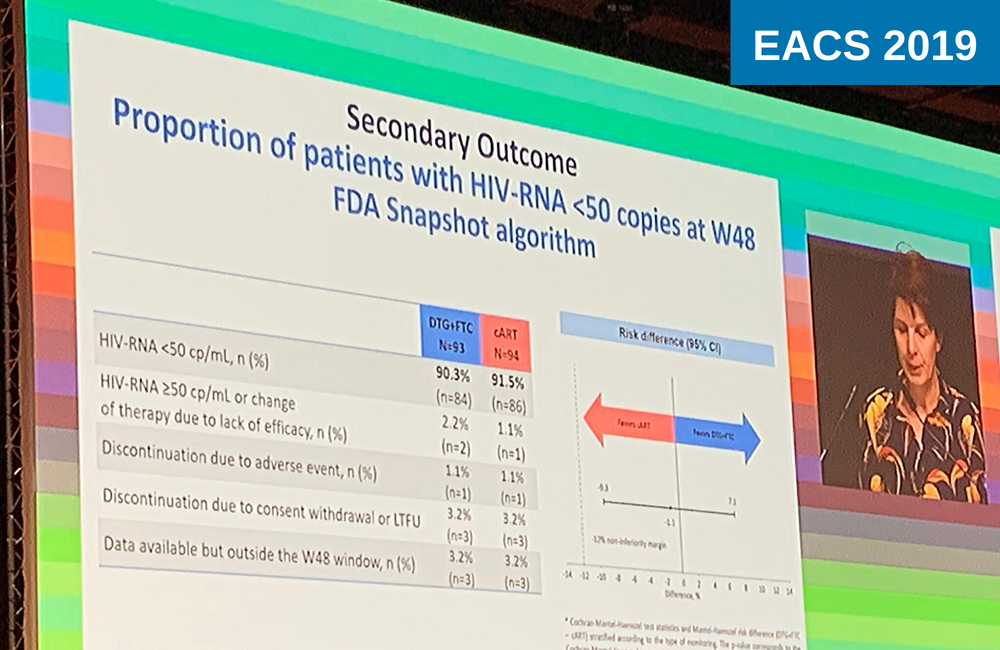
A new dual-therapy option, rilpivirine and darunavir (boosted by cobicistat) was tested as a switch regimen in virologically suppressed people in the randomised PROBE 2 trial conducted in Italy.
The study enrolled 160 people living with HIV who had viral load suppressed below 50 copies/ml for at least six months prior to enrolment, and no known resistance to protease inhibitors or non-nucleoside reverse transcriptase inhibitors (NNRTI). Participants were randomised to receive rilpivirine (25mg) and darunavir/cobicistat (800/100mg) once daily or to continue their existing three-drug regimen for 24 weeks, after which the three-drug group also switched to the investigational regimen.
Sixty-two per cent of the rilpivirine+darunavir group and 70% of the control group were male, participants had had undetectable viral load for a median of seven years and were taking their third antiretroviral therapy regimen at the time of randomisation. Approximately two-thirds were taking NNRTI-based therapy at randomisation, half with a nucleoside reverse transcriptase inhibitor (NRTI) backbone containing TDF and around a third with TAF.
The primary outcome of the study was viral suppression at 24 weeks. 91.3% of the rilpivirine+darunavir arm and 93.8% of the three-drug control arm had viral load < 50 copies/ml at week 24, a difference of -2.5% (95% CI -10.5-5.65), within the non-inferiority margin of 4%.
Discontinuation due to adverse events occurred more frequently in the rilpivirine+darunavir arm but most of the adverse events were not related to the study drugs (lung cancer, death, acute psychiatric disorder). Participants randomised to rilpivirine+darunavir had significantly higher median total cholesterol and LDL cholesterol levels after 24 weeks when compared to participants on three-drug regimens that contained TDF, but lipid levels did not differ significantly between the rilpivirine+darunavir group and non-TDF regimens in the control arm.
Rilpivirine+darunavir/cobicistat has been recommended as a new switch option in the 2019 EACS European treatment guidelines.
Simplification to dolutegravir and emtricitabine – SIMPL'HIV study
Swiss researchers investigated the use of emtricitabine with dolutegravir as a two-drug switch regimen in the SIMPL’HIV study. Dr Delphine Sculier of Geneva University Hospital presented the 48-week primary outcomes.
Emtricitabine was chosen as an alternative to lamivudine as it has a longer cellular half-life. Some retrospective studies have shown that emtricitabine is associated with lower risk of virological failure and drug resistance. The SIMPL’HIV study is the first test of emtricitabine as an element in a two-drug regimen.
The study randomised 187 people with suppressed viral load to continue their existing three-drug regimen or switch to dolutegravir/emtricitabine. The study excluded people who had switched to a previous antiretroviral regimen due to unsatisfactory virological response and anyone with resistance to an integrase inhibitor, but did not exclude people with the M184V mutation, which causes resistance to emtricitabine and lamivudine. Only one participant had documented resistance to emtricitabine.
Eighty-five per cent of the emtricitabine group and 81% of the three-drug group were male, approximately 80% of participants were white and approximately two-thirds were taking an integrase inhibitor and two NRTIs at enrolment.
The primary outcome of the study was viral suppression at week 48. Viral suppression by intent-to-treat analysis was 93.5% in the dolutegravir/emtricitabine arm and 94.7% in the three-drug arm, showing non-inferiority of the two-drug arm. Two cases of viral rebound were observed in the two-drug arm and one in the three-drug arm.
There was no significant difference in adverse events between the two study arms although serious adverse events were less frequent in the two-drug arm. However, it is unclear to what extent serious adverse events were drug related as they were not specified. Creatinine clearance declined significantly in the dolutegravir/emtricitabine group (adjusted difference -4.3 ml/min/1.73m2, p = 0.006). Follow-up in the study will continue to week 144.
De Miguel Buckley R et al. Dolutegravir and lamivudine for maintenance of HIV viral suppression in adults with and without historical resistance to lamivudine: 48-week results of a pilot clinical trial (ART-PRO). 17th European AIDS Conference, Basel, abstract PS7/5, 2019.
Maggiolo F et al. RPV+DRV/cobi as 2DR option in HIV-infected subjects on virologic suppression. 17th European AIDS Conference, Basel, abstract PS7/1, 2019.
Sculier D et al. Dolutegravir/emtricitabine dual therapy is non-inferior to standard combination antiretroviral therapy in maintaining HIV suppression throughout 48 weeks (SIMPL'HIV study). 17th European AIDS Conference, Basel, abstract PS8/3, 2019.
Van Wyk J et al. Switching to DTG/3TC fixed dose combination (FDC) is non-inferior to continuing a TAF-based regimen (TBR) through 48 weeks: subgroup analyses from the TANGO study. 17th European AIDS Conference, Basel, abstract PS7/2, 2019.
