Key points
- This page gives information on how soon HIV can be detected by a blood test and when you can be confident in the result.
- The window period of modern laboratory HIV tests is 45 days.
- The window period of rapid, point-of-care tests and self-tests is 90 days.
The window period refers to the time after infection and before seroconversion, during which markers of infection (p24 antigen and antibodies) are still absent or too scarce to be detectable. Tests cannot always detect HIV infection during the window period.
All tests have a window period, which varies from test to test. It also depends on the specimen that is being tested: window periods are usually reported based on a sample of blood plasma, but are longer when the specimen tested is fingerprick blood or oral fluid.
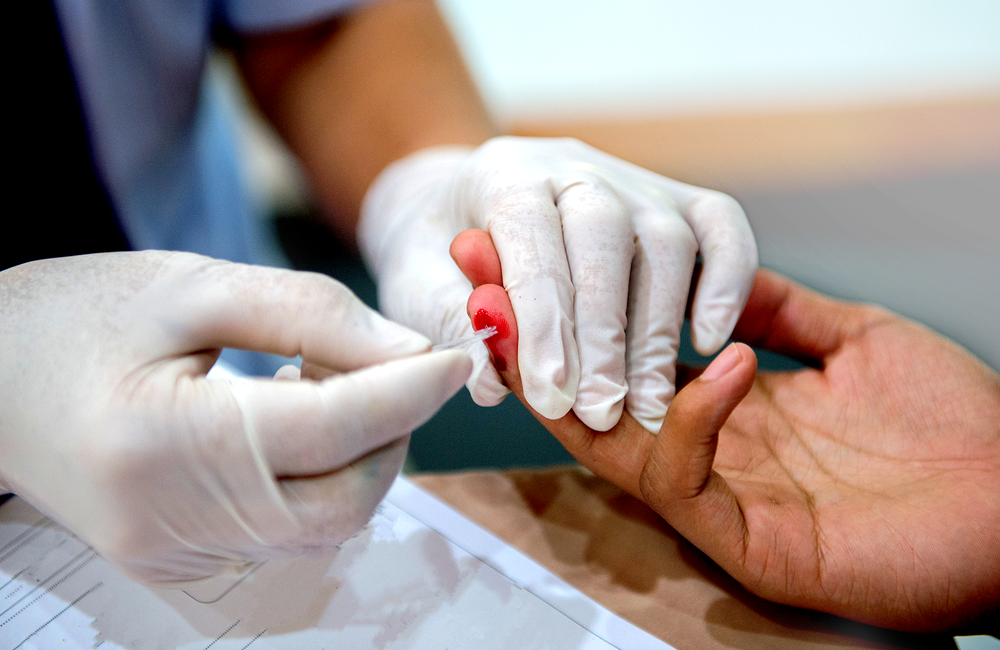
(Plasma is the colourless fluid part of blood, separated from whole blood using laboratory equipment. Fingerprick blood is produced by pricking the finger with a lancet, whereas oral fluid is obtained by swabbing the gums.)
There are two key questions to ask about a specific HIV test:
- How soon after someone is exposed to HIV can the test detect whether they have HIV? (Some, but not all, infections may be detected at this stage).
- How soon after exposure to HIV can an individual be confident that a negative test indicates they do not have HIV?
The information given in UK testing guidelines about window periods is based on answers to the second question – specifically, how long after exposure to HIV 99% of infections will be detected by a specific type of test. At this stage, it is highly likely that a negative result is accurate.
How long are the window periods of different HIV tests?
It is hard to say exactly how long the window period lasts, as there are variations between individuals and it is a difficult topic to research (recently infected people would need to know exactly when they were exposed to HIV and then give multiple blood samples over the following days and weeks).
Nonetheless, a study by Dr Kevin Delaney and colleagues calculated window periods for a range of HIV testing assays. All these analyses were based on plasma samples. Window periods are likely to be several days longer when testing samples of fingerprick blood or of oral fluid, as will be normal when using rapid, point-of-care tests and self-testing devices. Unfortunately, precise figures for how much longer the window periods are have not yet been published.
The researchers’ analysis confirms that fourth-generation laboratory tests (which detect both antibodies and p24 antigen) detect HIV infections between one and three weeks earlier than older antibody-only tests. Moreover, their data suggest that some countries’ guidelines which recommend retesting 90 days after a possible exposure to HIV are more cautious than they need to be.
A fourth-generation laboratory test is recommended in UK and US guidelines. It uses a sample of blood plasma or serum and can detect immunoglobulin G (IgG) antibodies, immunoglobulin M (IgM) antibodies and p24 viral antigen (a protein contained in HIV's viral core that can be detected sooner than antibodies). Commonly used tests of this type include Abbott Architect HIV Ag/Ab, GS Combo Ag/Ab EIA and Siemens Combo HIV Ag-Ab.
- The median window period is 18 days (interquartile range 13 to 24 days). This indicates that half of all infections would be detected between 13 and 24 days after exposure.
- 99% of HIV-infected individuals would be detectable within 44 days of exposure.
UK guidelines state that 45 days is the window period for fourth-generation laboratory tests.
A fourth-generation rapid test is available (Determine HIV Early Detect or Determine HIV-1/2). While results for this assay when testing plasma were broadly similar to those of equivalent laboratory tests, the window period is likely to be several days longer when testing fingerprick blood, as the test is normally used.
A few third-generation rapid, point-of-care tests are available. They can detect immunoglobulin G (IgG) antibodies and immunoglobulin M (IgM) antibodies. Examples include the INSTI HIV-1/HIV-2 and Uni-Gold Recombigen HIV tests. The estimated window period for INSTI when testing plasma are as follows:
- The median window period is 26 days (interquartile range 22 to 31 days). This indicates that half of all infections would be detected between 22 and 31 days after exposure.
- 99% of HIV-infected individuals would be detectable within 50 days of exposure.
However, those estimates were based on testing plasma. In practice, tests are usually done on fingerprick blood and the window period is likely to be several days longer.
UK guidelines state that 90 days is the window period for all rapid, point-of-care tests.
Third-generation laboratory tests are no longer recommended for use. They can detect immunoglobulin G (IgG) antibodies and immunoglobulin M (IgM) antibodies, but not p24 viral antigen. Their window periods are similar to those of the INSTI third generation rapid test (plasma samples), but a little shorter (median 23 days).
UK guidelines state that 60 days is the window period for third-generation laboratory tests.
Many rapid, point-of-care tests are described as second generation. They can detect immunoglobulin G (IgG) antibodies, but not immunoglobulin M (IgM) antibodies or p24 viral antigen. As these two substances are detectable sooner after HIV infection than IgG antibodies, second-generation tests have longer window periods. Examples include OraQuick Advance Rapid HIV 1/2, Clearview HIV 1/2 STAT-PACK and SURE CHECK HIV 1/2.
- The median window period is 31 days (interquartile range 26 to 37 days). This indicates that half of all infections would be detected between 26 and 37 days after exposure.
- 99% of HIV-infected individuals would be detectable within 57 days of exposure.
However, those estimates were based on testing plasma. In practice, tests are usually done on fingerprick blood or oral fluid and the window period is likely to be several days longer.
UK guidelines state that 90 days is the window period for all rapid, point-of-care tests.
No self-testing devices were included in this study. However, most self-tests are modified versions of rapid, point-of-care test kits that were originally designed for healthcare professionals. Most are based on second- generation tests, so are likely to have relatively long window periods. A few, including the INSTI HIV Self Test, are based on a third-generation test.
Similarly, self-sampling was not included. In the UK, this usually involve the user sending a sample of fingerprick blood to be tested in a laboratory with a fourth-generation antibody/antigen test. Plasma is extracted from the sample using centrifugation. In theory, the test will be as accurate with plasma from a self-collected sample of fingerprick blood as from venous blood, including in relation to acute (recent) infection.
Are these figures always accurate?
In some situations, these figures should be interpreted with caution:
- When tests are done with samples of fingerprick blood or oral fluid (rather than blood plasma), their window periods are likely to be longer.
- Individuals who are taking pre-exposure prophylaxis (PrEP) or post-exposure prophylaxis (PEP) may have a delayed antibody response, extending the window period.
- The data are based on individuals with HIV-1 subtype B (the form of HIV most commonly found in Western countries) and it’s possible that tests are less sensitive to other subtypes.
British HIV Association, British Association for Sexual Health and HIV and British Infection Association. Adult HIV Testing Guidelines 2020.
Delaney KP et al. Time Until Emergence of HIV Test Reactivity Following Infection With HIV-1: Implications for Interpreting Test Results and Retesting After Exposure. Clinical Infectious Diseases 64: 53-59, 2017.
Delaney KP et al. Time from HIV infection to earliest detection for 4 FDA-approved point-of-care tests. Conference on Retroviruses and Opportunistic Infections, abstract 565, 2018.