Key points
- These are the recommended tests for routine use in the UK.
- They test for p24 antigen as well as antibodies, so are better suited for detecting recent infection.
- Their sensitivities and specificities are excellent.
The most accurate and reliable routinely used diagnostic HIV test is a laboratory test that can detect both HIV antibodies and p24 antigen. They are called combination or combo tests because they detect both substances. They are “fourth-generation” tests, with more advanced technology than the earlier generations.
HIV antibodies are produced by the human body in response to HIV infection. In the weeks after exposure to HIV, the immune system recognises some components of the virus and begins to generate HIV antibodies in order to damage, neutralise or kill it (this period is known as ‘seroconversion’). These antibodies persist for life.
An HIV antigen, known as p24, is a structural protein that makes up most of the HIV viral core. High levels of p24 are present in the blood during the short period between HIV infection and seroconversion, before fading away. Since p24 antigen is usually detectable a few days before HIV antibodies, a test that can detect p24 has a slightly shorter window period than a test that only detects antibodies.
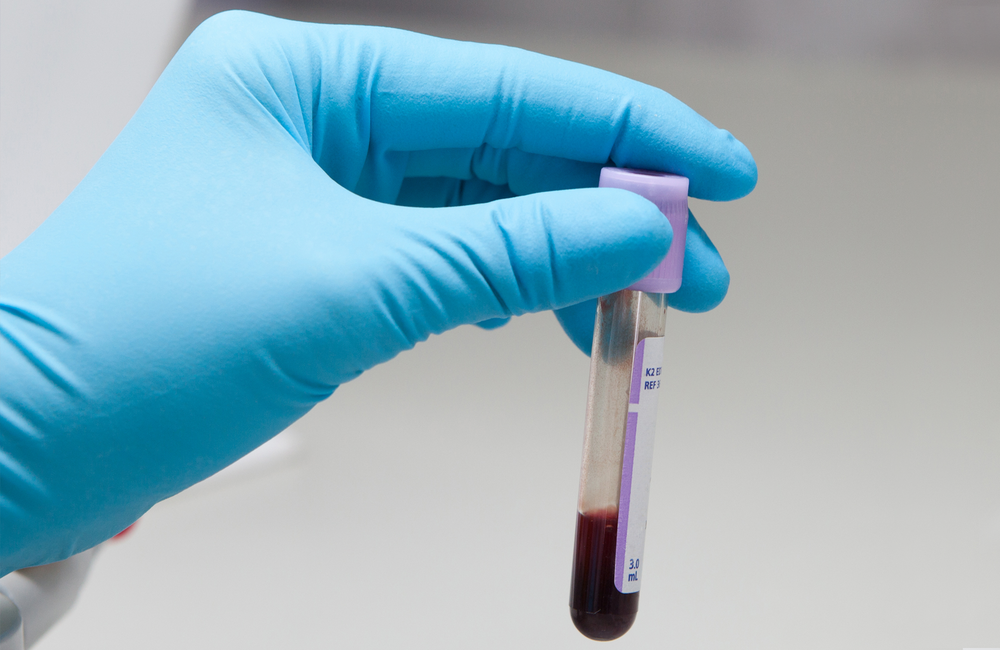
Fourth-generation combination tests are usually performed on plasma or serum (two components of blood, separated from whole blood using laboratory equipment). A blood sample is taken through a needle from a vein in the arm. Samples from many individuals are analysed at the same time, in a machine at a laboratory.
"Like any screening test, a reactive result (a preliminary positive result) must be verified with confirmatory tests."
These tests may also be referred to as “fourth-generation” tests or as an ELISA (enzyme linked immunosorbent assay). The first- and second-generation laboratory tests are no longer in use. The third-generation laboratory test only detects antibodies and is no longer recommended for routine use in the UK.
Tests of this type include: Abbott Architect HIV Ag/Ab combo, ADVIA Centaur HIV Ag/Ab Combo, Genscreen ULTRA HIV Ag-Ab, VIDAS HIV panel and Vitros HIV combo. In product names, ‘Ag/Ab’ indicates that the test looks for both antigen and antibody.
Some tests may also be described as fifth-generation. They detect the same biomarkers but can also distinguish between samples positive for p24 antigen and for antibodies, and also between HIV-1 and HIV-2. They include the Bio-Rad BioPlex 2200 HIV Ag/Ab and Elecsys HIV Duo.
Also available is a rapid, point-of-care combination test, the Alere HIV Combo. There’s information about this test on another page.
Window periods and accuracy
The window period is the time immediately after infection, during which tests cannot always detect antibodies or p24 antigen, and so may give a false negative result. It is hard to say exactly how long the window period for any test lasts, as there are variations between individuals and it is a difficult topic to research (recently infected people would need to know exactly when they were exposed to HIV and then give multiple blood samples over the following days and weeks). Nonetheless, it is estimated that the median window period for fourth-generation tests is 18 days, with half of all infections being detected between 13 and 24 days after exposure. While occasionally this period will be a little longer, 99% of HIV-infected individuals would be detectable within 44 days of exposure.
Fourth-generation laboratory tests are extremely accurate. The key measures of accuracy are sensitivity (the percentage of results that are correctly positive when HIV is actually present) and specificity (the percentage of results that are correctly negative when HIV is not present). In terms of sensitivity, a Centers for Disease Control and Prevention (CDC) review identified four studies of two different assays, with sensitivity always above 99.7% for established infection. A Health Protection Agency evaluation found that nine out of the ten tests they evaluated had a sensitivity of 100%, while a French evaluation found that ten of twelve tests had a sensitivity of 100%. The lowest sensitivity was 99.8%.
Similar results were found for specificity. Both tests checked by the CDC had a specificity of 99.5% or above; all tests in the Health Protection Agency evaluation had a specificity of 99.7% or above, and the French study found that all tests produced after the year 2000 had a specificity of 99.8% or above.
Like any screening test, a reactive result (a preliminary positive result) must be verified with confirmatory tests. The laboratory should re-test the sample with a different assay before communicating the preliminary results. Then a new sample should be taken and tested, in order to rule out a clerical error (such as two patients’ samples being mixed up).
The British HIV Association say that test results should normally be available within 48 hours. The main delay in getting results is due to the fact that samples are analysed in batches, and it may take a lab several days to accumulate enough samples to analyse. The actual process of conducting the test usually takes a few hours.
Fourth-generation tests are extremely sensitive and specific. They are more reliable in detecting early infection than rapid tests. They are appropriate to use when immediate provision of results is not necessary, and when people are likely to come back for their results. Because testing is handled by a central lab, quality control programmes are easier to implement.
Delaney KP et al. Time Until Emergence of HIV Test Reactivity Following Infection With HIV-1: Implications for Interpreting Test Results and Retesting After Exposure. Clinical Infectious Diseases 64: 53-59, 2017.
Centers for Disease Control and Prevention. Laboratory testing for the diagnosis of HIV infection: updated recommendations, 2014.
Perry KR et al. Improvement in the performance of HIV screening kits. Transfusion Medicine 18:228-240, 2008.
Ly TD et al. Could the new HIV combined p24 antigen and antibody assays replace p24 antigen specific assays? Journal of Virological Methods 143:86-94, 2007.