Key points
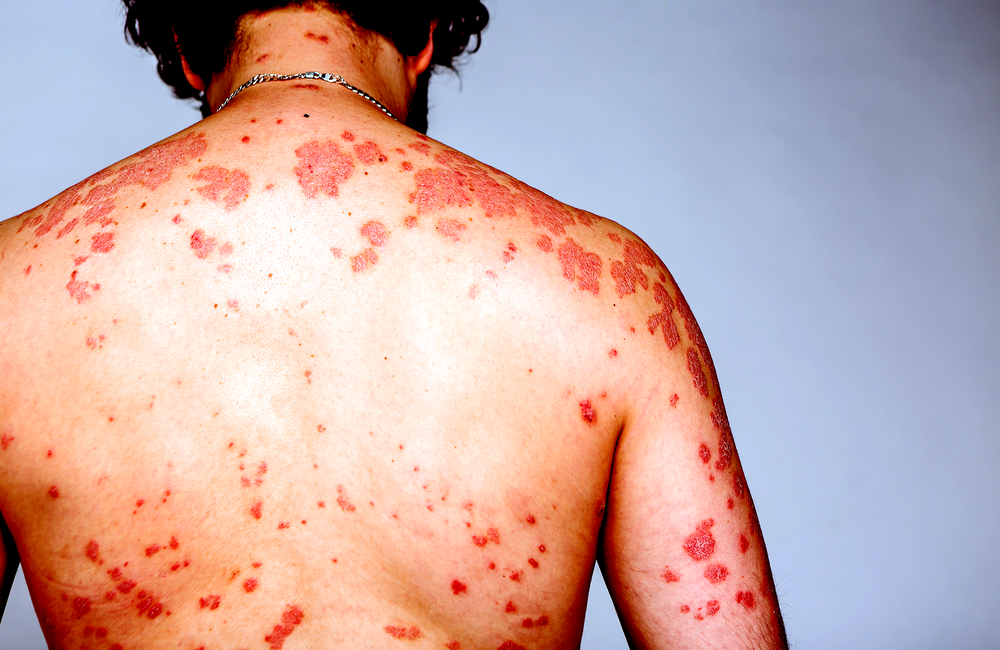
- A rash can be a symptom of recent HIV infection.
- Other infections can also cause skin problems.
- They may also be a side-effect or allergic reaction to an anti-HIV drug.
- Allergic drug reactions need urgent medical attention.
There are three main causes of skin problems in people living with HIV: interactions between the immune system and HIV, infections, and side-effects of drugs.
Some HIV-related skin conditions or treatment-related side-effects can be very serious and require urgent medical attention.
The immune system and HIV
When people first get HIV, they may experience flu-like symptoms as part of something called a seroconversion illness. This illness may include a non-itchy, red rash lasting 2 to 3 weeks. During ongoing infection, the immune system becomes damaged and this may lead to red and itchy (pruritic) skin. This may be treated with steroid creams or antihistamines. Skin problems may also occur when the immune system starts to recover due to HIV treatment (especially acne and folliculitis, infection of the follicles). It may be a sign of improving health of the immune system, as it responds to the anti-HIV drugs.
Skin problems caused by infections
Infections are generally divided into three main groups: bacterial, fungal or viral infections. Some people will experience skin problems unrelated to their HIV diagnosis, as these are a common health issue. Some of the conditions described here are most common in people with a low CD4 cell count. Starting HIV treatment will help reduce the likelihood of them occurring.
Eczema (dry or irritated skin) has many causes and may be treated with antihistamines. To relieve any dry skin condition, moisturise frequently to stop the skin drying out further. Avoid long baths and the use of soap, shower gels and other potential irritants. Instead, use aqueous cream (E45) or moisturiser to wash with. Corticosteroid creams can reduce swelling and redness, and antihistamines can reduce itching. Try not to scratch, as this can make eczema worse and cause scarring.
Dermatitis (inflammation of the skin) is identified by red patches and a flaky rash. It may be caused by contact with an irritating substance or by eczema. Seborrhoeic dermatitis (inflammation of the skin’s oil glands, caused by an overgrowth of yeast on the skin, or a reaction to the yeast) often occurs in hairy parts of the body. It causes red, itchy, flaky, inflamed skin. Mild cases cause dandruff. It’s common in symptomatic HIV, and it can be harder to treat in people living with HIV. Dermatitis may be treated with steroid ointments or tablets, or with anti-fungal creams or tablets. Some scalp problems can be treated with anti-dandruff or anti-fungal shampoos.
Photodermatitis is a skin condition where the skin reacts to exposure to the sun by turning darker in colour. It's most common in darker-skinned people, but anyone with HIV may experience photodermatitis.
Tinea is a fungal infection that causes flaky red skin and moist white patches. It is treated with anti-fungal creams. Keep skin clean and dry and avoid irritants, e.g. deodorants.
Impetigo is a bacterial skin infection indicated by yellow, crusty red sores. Skin follicles may also become infected, leading to boils or abscesses, which are treated with antibiotics.
Folliculitis (small lumps or pustules in the follicles – the hair’s root) is a skin infection, most likely caused by yeast, which is treated with anti-fungals. Prurigo nodularis is a skin condition involving outbreaks of itchy, crusted lumps on the skin. The itching can be intense and severe. These are both mainly seen in people with very low CD4 cell counts.
Small pearly pimples may be caused by viral infections such as the pox virus, Molluscum contagiosum, or by fungal infections such as cryptococcosis. Molluscums can spread very quickly and require treatment at your HIV clinic.
Warts, particularly genital and anal warts caused by the human papillomavirus (HPV) are often seen in people living with HIV. See our factsheet on genital warts and HPV for more information.
Herpes and the AIDS-defining cancer Kaposi’s sarcoma also affect the skin.
Drug side-effects
People with HIV often develop skin-related side-effects, such as rash.
The NNRTI nevirapine (Viramune) causes rashes in about 15 to 20% of people. This rash is usually mild and disappears as your body gets used to the drug. The risk is higher in people with a healthier immune system, so it is not recommended for women with CD4 counts above 250 or men with counts higher than 400. To minimise the chance of side-effects, your doctor may recommend that you start at a lower dose and increase to the full dose over two weeks. Nevirapine is no longer recommended as standard HIV treatment in the UK.
"Infections are generally divided into three main groups: bacterial, fungal or viral infections."
Developing a rash is quite a common side-effect of other anti-HIV drugs too, but in most cases it is mild and goes away on its own. Tell your doctor if you develop a rash, so the cause can be investigated.
A very small number of people develop a very serious drug reaction called Stevens Johnson syndrome (SJS) after starting treatment with nevirapine (Viramune) or etravirine (Intelence). Skin reactions such as SJS may cause severe rash, crusting or ulcers of the mouth or genitals, burning skin and large layers of skin to flake off. See your HIV clinic immediately (or A&E if out of hours) if you develop a rash together with any of these symptoms:
- fever
- feeling generally unwell or extremely tired
- muscle or joint ache
- blistering of the skin
- mouth ulcers
- swelling of the eyes, lips, mouth or face
- breathing difficulties
- yellowing of the skin or eyes
- dark urine
- pale stools
- pain, aching or sensitivity on the right-hand side of the body, below the ribs.
Rash is also a sign of an allergic reaction to the anti-HIV drug abacavir (Ziagen). Abacavir is also in the combination pills Kivexa, Triumeq and Trizivir. If this reaction occurs, you should contact your doctor immediately. If you stop taking abacavir because you developed the allergic rash you must not take the drug again as this can cause potentially fatal side-effects.
Having an allergic reaction to abacavir has been associated with the presence of a particular gene. Before starting treatment with abacavir you should have a test to see if you have this gene. If you do, you must not take abacavir. If you do not have the gene, it is very unlikely that you will have an allergic reaction to the drug, but you should still contact your clinic if you develop a rash or feel unwell after starting the drug. Fever and rash are the most common symptoms of this hypersensitivity reaction. However, it is possible to have such a reaction without these. Other key symptoms include nausea, vomiting, diarrhoea, abdominal pain, shortness of breath, cough, headache and muscle weakness.
Other drugs which are regularly used to treat infections commonly seen in people with HIV can also cause rash and skin reactions. These include Septrin (cotrimoxazole), dapsone, pyrimethamine, clindamycin, atovaquone, the aminopenicillins, thiacetazone and sulphadiazine.
