Data from three, large representative samples of the UK population over the last two decades show a significant rise in the uptake of HIV testing, especially among men who have sex with men (MSM), individuals with more sexual partners and African people. Nonetheless, in each of these target groups, half of those questioned had not taken an HIV test in the past five years, showing how far the UK needs to go in order to reduce rates of undiagnosed HIV.
The figures are among those published from the National Survey of Sexual Attitudes and Lifestyles (Natsal) in The Lancet this week. As this study recruited a large, representative sample from households throughout Great Britain, it is more likely than most other studies to give an accurate picture of HIV testing behaviours across the population.
The study
Sexual health researchers typically recruit samples of people who are in contact with specialised sexual health services or who attend locations associated with particular sections of the population (e.g. gay bars). The National Survey of Sexual Attitudes and Lifestyles is one of the only studies that has had the financial resources and political backing needed to enrol a representative sample of the wider population. An individual with no identifiable risk factors for HIV is as likely to be recruited as a person with multiple risk factors.
In 2010 to 2012, interviewers approached people aged 16 to 74 years who were living in households across England, Scotland and Wales. Two-thirds of those who were contacted agreed to take part, with 15,162 individuals completing the survey. The sample was statistically adjusted so that it matched the profile of the population in the country’s census in terms of geographical spread, age and gender (e.g. slightly fewer men than women had been recruited).
Respondents took part in hour-long interviews, with sensitive questions about sexual health being asked on a self-completed computer survey, to ensure confidentiality.
Although the survey is cross-sectional (it doesn’t follow individuals over time), it has now been conducted on three occasions – in 1990, 2000 and 2010. A total of 45,199 people have taken part in the three studies, providing a unique insight into changing sexual behaviour over more than two decades. (For an overview of the study's findings, please see another Aidsmap article or infographics on the study website).
HIV testing
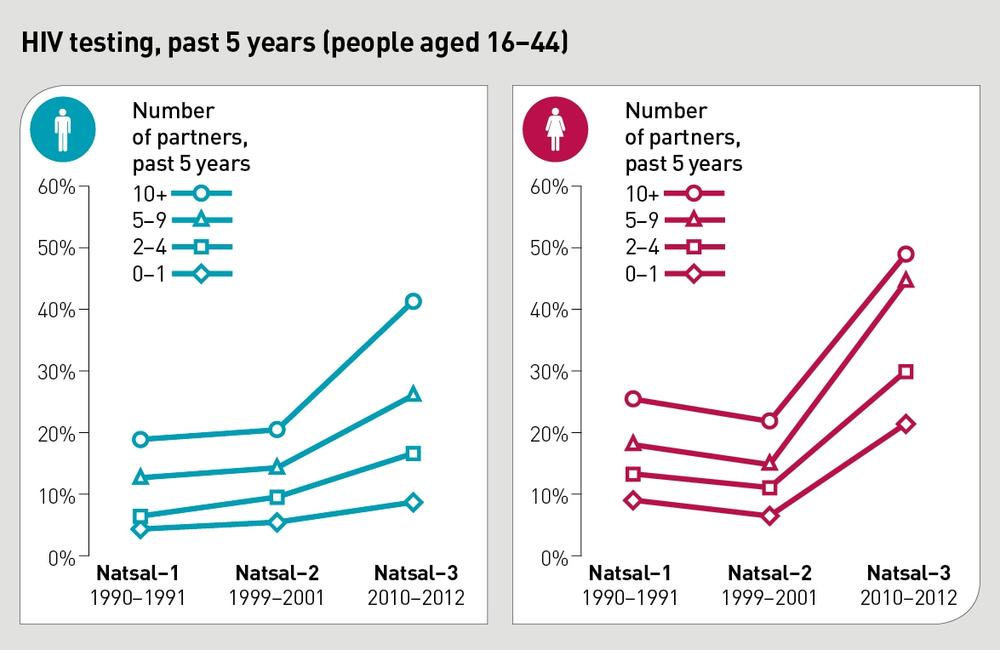
Each Natsal study has asked whether participants had taken an HIV test in the previous five years. The number doing so has risen over the years.
Whereas 6.6% of men had tested in 1990, 9.2% had done so in 2000, rising to 16.9% in 2010. A greater increase in testing has been seen in women – 10.5% in 1990, 8.7% in 2000, and 27.6% in 2010.
And this rise has been most noticeable in people who may be at an elevated risk of HIV infection. For example, in 2010, 55.9% of men with more than ten sexual partners in the past five years, and 65.6% of women with more than ten partners, had taken an HIV test.
There was also a strong rise among MSM (individuals who reported same-sex behaviour in the previous five years), but this still falls far short of current recommendations for all MSM to test at least once a year. Having taken a test in the previous five years was reported by 33.6% in 1990, 39.3% in 2000 and 51.6% in 2010.
In other words, in the most recent survey, half the gay and bisexual men had not tested at all in the previous five years. Moreover, only a quarter (27%) had tested within the previous year.
HIV testing has also gone up among black people, and specifically, among black African people. In 2010, 43.9% of African men and 46.1% of African women had tested in previous five years.
The data also show more testing in other target groups in current HIV testing guidelines – people attending sexual health clinics, people diagnosed with a sexually transmitted infection, women attending antenatal services and women terminating a pregnancy.
Prevalence of HIV infection
The 2010 survey also provides reassurance that the prevalence of HIV infection remains low in the UK, and largely restricted to individuals with known risk factors for HIV infection.
A sub-set of 4550 respondents were asked to provide a urine sample for anonymised testing of HIV and other infections. (Although testing urine samples for HIV antibodies isn’t sufficiently accurate for use in clinical practice, it is used in epidemiological research.)
Across the whole population aged 16 to 44 years, 2 in 1000 men (0.2%) and 1 in 1000 women (0.1%) had HIV.
This amounts to nine survey respondents – five of them were men who have sex with men, three were women of black ethnicity, and one was a black heterosexual man. Almost all said they had previously tested for HIV.
While there was a similar picture for gonorrhoea infection, chlamydia was much more commonly found (1.1% of men and 1.5% of women), much of it in individuals who had only had one sexual partner in the previous year. Human papillomavirus (HPV) was the most commonly detected infection, with high-risk strains (16 and 18) found in 15.9% of women.
Whereas epidemiologists already have a lot of data on sexually transmitted infections in people who attend sexual health services, the data from Natsal provide valuable information on the extent of infection in people who don’t attend those services, as well as on risk factors for infection. The data have already been used by Public Health England to refine their estimates of undiagnosed infections in the wider population.
Sonnenberg P et al. Prevalence, risk factors, and uptake of interventions for sexually transmitted infections in Britain: findings from the National Surveys of Sexual Attitudes and Lifestyles (Natsal). The Lancet 382: 1795 - 1806, 2013. (Full text freely available.)
